Session Information
Date: Monday, November 14, 2016
Title: Rheumatoid Arthritis – Clinical Aspects - Poster II: Co-morbidities and Complications
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Rheumatoid arthritis (RA) associated interstitial lung disease (ILD) carries a risk for serious infection due to lung disease, immunosuppressive therapy, and RA disease itself.
Methods: All patients with RA-ILD (ACR 1987 criteria for RA) seen at a single center from 1998-2014 were identified and manually screened for study inclusion. Follow-up data were abstracted until death or December 31, 2015, including immunosuppressive medications at and after ILD diagnosis. Serious infection was defined as an infectious process requiring both antimicrobial therapy and hospitalization. Risk of infection was analyzed by person-year (py) methods using a 30-day washout period after discontinuation of individual medications.
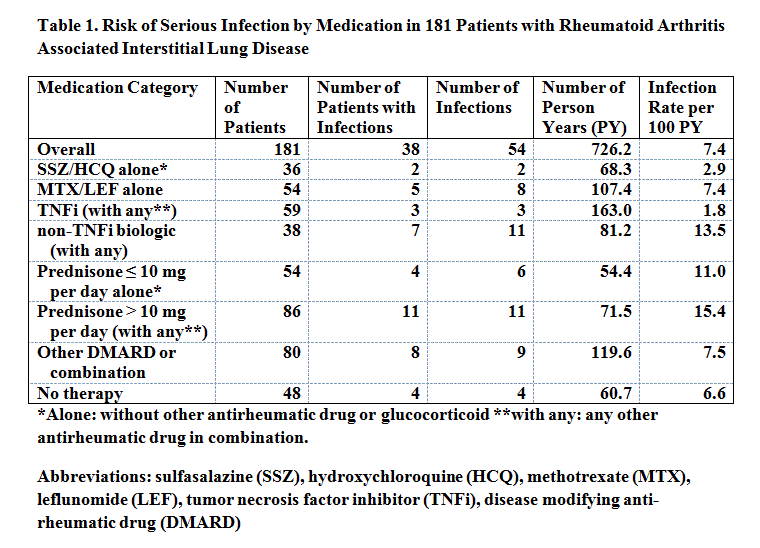
Results: Of the 181 included patients, 87 (48%) were female and 96% were Caucasian. The mean age at ILD diagnosis was 67.4 (±9.9) years with a median time of 4.9 (range: -10.9 to 48.1) years from RA to ILD diagnosis. Median follow-up time was 3.1 (range: 0.01 to 14.8) years. Sixty-seven (37%) were never smokers. Ninety-eight (54%) had usual interstitial pneumonia (UIP), 73 (40%) had non-specific interstitial pneumonia (NSIP), and 10 (6%) had RA-related organizing pneumonia (OP). A total of 54 serious infections were identified of which pneumonia was the most common with (3.9 per 100 py) followed by opportunistic infections (1.5 per 100 py) and septicemia (1.0 per 100 py). Overall infection risk was higher in OP (27.1 per 100 py) than UIP (7.7 per 100 py) or NSIP (5.5 per 100 py) (P<0.001), and did not differ in UIP and NSIP (p=0.24). Pneumonia and septicemia were also significantly more common among OP patients (although number with OP was small) than in UIP and NSIP (p=0.002 and p=0.007, respectively), but there were no differences between groups in opportunistic infections (p=0.63). Immunosuppressive regimens were summarized into distinct groups (see table), of which tumor necrosis factor inhibitors with or without disease modifying anti-rheumatic drug (DMARD) or glucocorticoids was the most common (163.0 py). Sulfasalazine and/or hydroxychloroquine (SSZ/HCQ) were used as the referent group for comparisons and had an infection rate of 2.9 per 100 py. The highest infection rate observed was with a daily prednisone use > 10mg per day with or without additional DMARDs with a rate of 15.4 per 100 py. There were no significant differences observed between baseline and no immunosuppression, methotrexate/leflunomide (MTX/LEF), tumor necrosis factor inhibitor (TNFi) or other DMARD combination. Prednisone > 10mg (RR: 4.40; 95%CI: 1.38, 27.7) and non-TNFi biologic (RR: 3.87; 95%CI: 1.22, 24.3) had the highest risk.
Conclusion: Patients with RA-ILD are at high risk of serious infection. Prednisone use at >10 mg per day was associated with higher rates of infection, and lowest risk was in patients on SSZ/HCQ and TNFi. Channeling bias cannot be excluded.
To cite this abstract in AMA style:
Zamora-Legoff A, Krause M, Crowson CS, Ryu JH, Matteson EL. Risk for Serious Infection in Rheumatoid Arthritis Associated Interstitial Lung Disease [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/risk-for-serious-infection-in-rheumatoid-arthritis-associated-interstitial-lung-disease/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/risk-for-serious-infection-in-rheumatoid-arthritis-associated-interstitial-lung-disease/