Session Information
Title: Systemic Lupus Erythematosus - Clinical Aspects and Treatment: Cardiovascular Disease and Pregnancy
Session Type: Abstract Submissions (ACR)
Background/Purpose: Women with SLE have increased rates of subclinical atherosclerosis. We have investigated which risk factors may be related to the increase in subclinical atherosclerosis, as measured by carotid plaque and IMT in women with SLE (cases) and without SLE (controls), over 5 years.
Methods: Baseline data including demographics and cardiovascular risk factors (CVRF) were collected from 151 cases and 126 controls in the Study of Lupus Vascular and Bone Long-term Endpoints (SOLVABLE). SLE factors measured included the modified American College of Rheumatology/Systemic Lupus International Collaborative Clinics Damage Index (excluding CV outcomes), Systemic Lupus Erythematosus Disease Activity Index 2000, disease duration, complement C3 and C4 levels, and self-reported use of corticosteroids, hydroxychloroquine, and immunosuppressants. Plaque and IMT were measured by B-mode ultrasound at baseline and at a follow-up visit. Plaque progression was defined as any increase in plaque number at follow-up. Logistic and linear regression were used to identify predictors of progression in plaque and increase in IMT, respectively; multivariate models included adjustment for the a priori CV risk factors age, hypertension, and total cholesterol/HDL ratio.
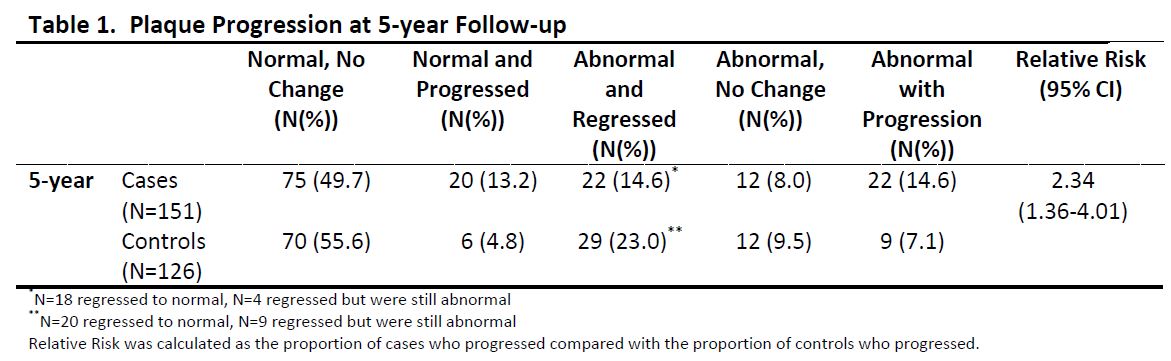
Results: The mean ± SD follow-up time was 5.36 ± 0.60 years in cases and 5.63 ± 0.66 years in controls. Mean IMT change per year was 0.0037 ± 0.024 in cases and -0.0001 ± 0.029 in controls (p=0.25); 71% of cases and 63% of controls had an increase in IMT at follow-up. Of cases, 28% had more plaque at follow-up, compared with 11.9% of controls with a relative risk for plaque progression of 2.34 (95%CI 1.36-4.01) (Table 1). Only in cases, higher fasting glucose (β=0.005 for glucose higher by one SD, 95%CI 0.0001-0.009) was significantly associated with increase in IMT in adjusted models. In adjusted models, the presence of SLE, higher cumulative and baseline corticosteroid dose were significantly associated with plaque progression in cases (Table 2). No CVRF were associated with either increase in IMT or plaque progression in controls, in the adjusted models.
Conclusion: SLE itself infers a greater risk for subclinical atherosclerosis progression over 5 years in women, as measured by an increase in carotid plaque. Higher baseline and cumulative corticosteroid dose were associated with an increased risk for plaque progression, suggesting that earlier and more aggressive treatment of SLE may be beneficial. No CVRF were associated with plaque progression in controls. Only higher baseline fasting glucose level independently predicted increase in IMT in cases.
Disclosure:
A. Lertratanakul,
None;
P. W. Wu,
None;
A. Dyer,
None;
W. Pearce,
None;
E. Barinas-Mitchell,
None;
T. Thompson,
None;
R. Ramsey-Goldman,
None.
« Back to 2014 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/risk-factors-for-changes-in-subclinical-atherosclerosis-as-measured-by-carotid-intima-media-thickness-imt-and-plaque-over-5-years-in-women-with-systemic-lupus-erythematosus-sle/