Session Information
Date: Tuesday, November 12, 2019
Title: Osteoporosis & Metabolic Bone Disease – Basic & Clinical Science Poster
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Rheumatoid arthritis (RA) is an independent risk factor for osteoporosis (OP) and fracture. Although several OP risk factors are well-described in RA, many mechanisms by which the disease impacts bone mineral density (BMD) remain unknown. Measuring the direct contribution of RA disease activity on BMD is complicated by concomitant risk factors for BMD loss such as glucocorticoid treatment, inactivity and systemic inflammation. We evaluated the association of RA disease activity as measured by the Disease Activity Score 28 Joints with Erythrocyte Sedimentation Rate (DAS28ESR) and femoral neck BMD by dual energy x-ray absorptiometry (DXA), after controlling for known osteoporosis (OP) risk factors.
Methods: Data were from the University of California, San Francisco RA Cohort, an observational cohort established in 2006. In this cross-sectional analysis, all participants with femoral neck BMD and at least 1 DAS28ESR measurement were included. Mean DAS28ESR from study entry to date of DXA was calculated, and participants were placed into disease activity categories, based on validated cut-points (Remission/Low, Moderate and High). Mean values for other time-varying exposures from enrollment to DXA date were also calculated. Multivariable linear regression was performed to identify the independent association of DAS28ESR with BMD, controlling for age, race/ethnicity, RA duration, body weight, RA and OP medications, and high positive anticyclic citrullinated peptide (CCP) status (previously identified as an independent predictor of low BMD in RA).
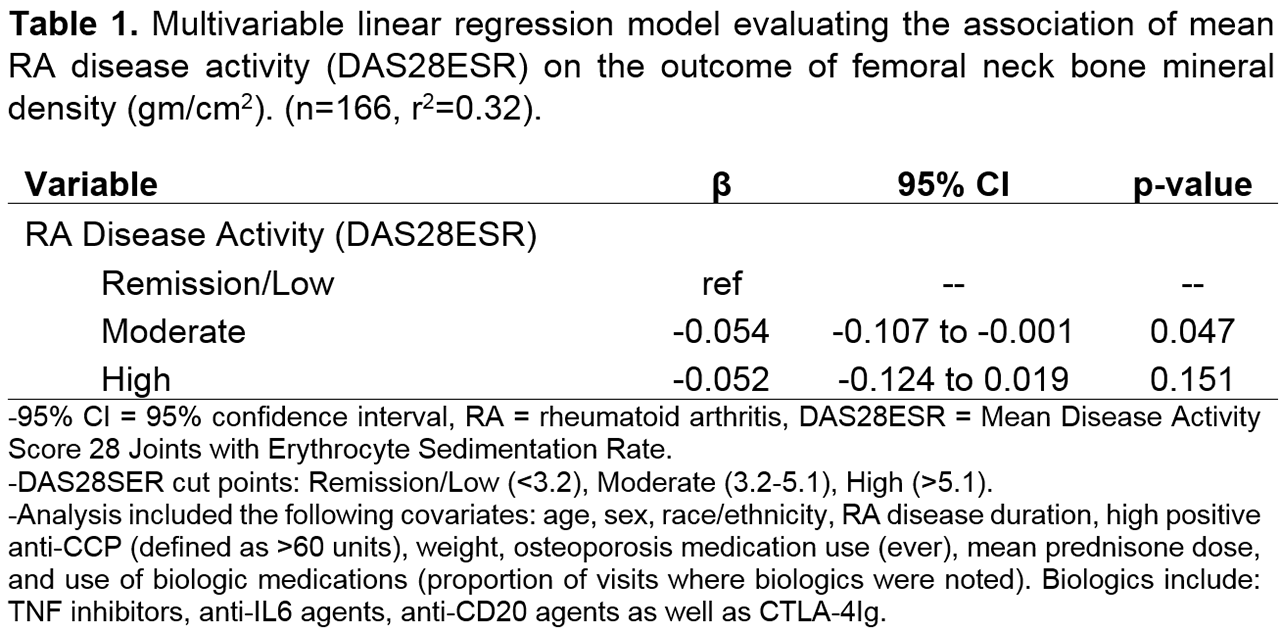
Results: 166 participants with a mean age of 63±10.3 years; 87% female; 46% Latino and 35% Asian; and mean RA duration of 15±8 years were included. The majority were rheumatoid factor (RF) (n=145, 87%) and high anti-CCP positive (n= 109, 65%). The mean prednisone dose was 3.9±3.6 mg/day, 58% (n=97) were exposed to biologics and 57% (n=95) were exposed to OP medications over the course of the study. BMD categories based on femoral neck BMD were: 45% Normal BMD (n=76), 45% Low BMD (n=75), 10% OP (n=16). The distribution of DAS28ESR categories was: 20% low/remission (n=37), 60% moderate (n=100) and 18% high (n=30). In the multivariable model, moderate and high disease activity were both independently negatively associated with femoral neck BMD (β=-0.054 and -0.052 g/cm2 respectively), but only moderate disease activity achieved statistical significance (p< 0.05).
Conclusion: Controlling for known OP risk factors, higher RA disease activity is independently associated with lower BMD. These results suggest that treating RA patients to achieve the target of low disease activity or remission may improve BMD. Longitudinal studies are needed, however, to further explore these associations.
To cite this abstract in AMA style:
Wysham K, Graf J, Shofer J, Black D, Andrews J, Shoback D, Katz P. Rheumatoid Arthritis Disease Activity Is Associated with Low Femoral Neck Bone Mineral Density in a Diverse Cohort of Patients [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/rheumatoid-arthritis-disease-activity-is-associated-with-low-femoral-neck-bone-mineral-density-in-a-diverse-cohort-of-patients/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/rheumatoid-arthritis-disease-activity-is-associated-with-low-femoral-neck-bone-mineral-density-in-a-diverse-cohort-of-patients/