Session Information
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Reproductive health intention screening is critical in women with systemic rheumatic diseases, as both disease activity and medication use can impact pregnancy outcomes. However, studies report that < 50% of patients with rheumatic diseases receive contraception counseling. We introduced a simple reproductive health intention screen, One Key Question ® (OKQ), to our academic rheumatology practice and examined subsequent practice patterns.
Methods: We developed an electronic medical record (EMR) smart phrase with OKQ (“Would you like to become pregnant in the next year?”) with responses that would prompt documentation of contraception, teratogenic medication use and referrals for OB/GYN care when appropriate. Reproductive age (18-50 year-old), female patients with a systemic rheumatic disease were flagged in the EMR for screening before appointments. We introduced OKQ at Rheumatology Grand Rounds, in email notifications, and with exam room reminder cards. Documentation of OKQ was at the rheumatologists’ discretion. We measured reproductive health intention screening over 6 months following introduction of OKQ, conducted chart reviews, and used descriptive statistics and a logistic regression model to compare patients who were screened (with OKQ or other documentation) vs. a randomly selected subset of patients who had been flagged for screening but did not have OKQ documented.
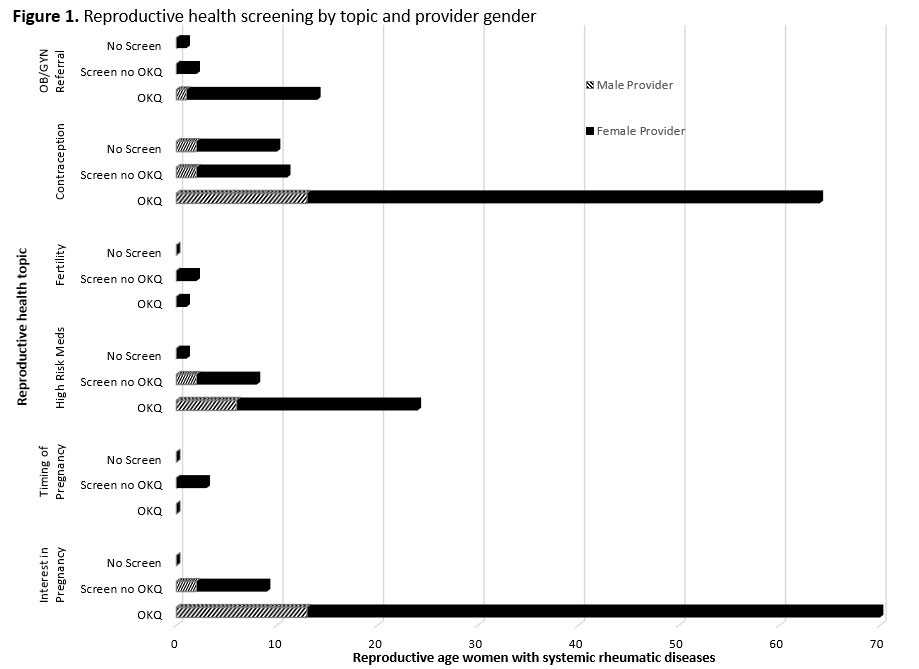
Results: Over the 6-month pilot with 43 rheumatologists (56% female), among 1092 reproductive age women with rheumatic diseases, 11 providers (82% female) used OKQ to document reproductive health preferences for 83 women (8%). In the subset of 96 charts flagged for screening but without OKQ documented, 15 providers (67% female) documented reproductive health screening (without OKQ) for 18/96 women (19%). Patients had 2.4 times higher odds of being screened if they saw a female vs. male rheumatologist (95% CI 1.21-4.85). OKQ use resulted in documentation of a broader range of reproductive health topics by rheumatologists of both genders (Figure 1). Adjusting for provider gender, a 1-year increase in patient age was associated with 5% lower odds of screening (95% CI 0.02-0.09). Highly effective contraception was associated with reproductive health screening (p< 0.0001). Although use of a high-risk medication was not associated with screening (p=0.22) (Table 1), rheumatologists who screened their patients were more likely to document risks of teratogenic medications (p< 0.0001).
Conclusion: Despite introducing a simple, standardized intervention, < 10% of reproductive age women with rheumatic diseases were comprehensively screened using OKQ, < 20% of an eligible subset were asked selected reproductive health-related questions, and >50% of unscreened patients had no documented contraception. Younger age and seeing a female rheumatologist resulted in higher odds of screening. While some providers may have screened patients without documenting the response, the data suggest that a high proportion of patients are not being screened. While uptake was suboptimal, this intervention improved the depth and breadth of reproductive health documentation among those who were screened.
To cite this abstract in AMA style:
Pryor K, Albert B, Ritter S, Tarter L, Coblyn J, Bermas B, Dutton C, Pace L, Janiak E, Feldman C. Reproductive Health Intention Screening in Women with Systemic Rheumatic Diseases: Low Uptake and Gender-Specific Provider Patterns Following a Standardized Intervention [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/reproductive-health-intention-screening-in-women-with-systemic-rheumatic-diseases-low-uptake-and-gender-specific-provider-patterns-following-a-standardized-intervention/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/reproductive-health-intention-screening-in-women-with-systemic-rheumatic-diseases-low-uptake-and-gender-specific-provider-patterns-following-a-standardized-intervention/