Session Information
Date: Monday, October 22, 2018
Title: 4M084 ACR Abstract: Pediatric Rheum–Clinical I: Outcomes & Comorbidities (1846–1851)
Session Type: ACR Concurrent Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose: Innovative changes towards targeted treatment have improved the outcome dramatically for juvenile idiopathic arthritis (JIA) but the question remains how well these patients perform during long-term follow-up.
The aim of the study was to assess the disease activity, remission rate and damage 18 years after JIA onset in a population-based setting.
Methods: 510 consecutive cases of JIA with disease onset between 1997 and 2000 from Denmark, Norway, Sweden and Finland were prospectively included in a close to population-based 18-year (mean 17.5 years; range 14.2-20.2) follow-up study. The follow-up visit included an update on the demographic and clinical data such as a joint examination and remission status (preliminary Wallace criteria).
Results: In total 434/510 (85%) eligible JIA participants with a mean age (±SD) of 24.0 (±4.4) years were included. Of those, 76 participants (15%) were lost to follow-up. Out of the included participants 329 (76%) attended a follow-up visit, and 105 participants (24%) were evaluated by a telephone interview.
The distribution of the JIA categories was as follows: 3% systemic, 27% persistent oligoarticular, 20% extended oligoarticular, 16% polyarticular RF negative, 1% polyarticular RF positive, 7% psoriatic, 10% enthesitis-related arthritis (ERA) and 15% undifferentiated JIA.
Treatment with synthetic disease-modifying anti-rheumatic drugs were given to 66 participants (15 %) and biologics to 84 patients (19%) at the follow-up.
For the 329 participants the median active joint count was 0 (range 0-15), however during the 18 years of disease course the median cumulative joint count was 8 (range 1-59). The median composite juvenile arthritis disease activity score JADAS71 was median 1.5 (range 0-31.6) with the ERA category having the highest median score of 4.5 (range 0-16.5) (p=0.003). In the cohort 48% had a JADAS71 score <1 indicating inactive disease.
Articular damage (JADI-A) was found in 20% of the participants who had a follow-up visit and 12.5% had developed extra-articular damage (JADI-E), most commonly as ocular damage, found in 26/41 (63%). The highest JADI-A and JADI-E scores were found in the polyarticular RF negative and psoriatic categories.
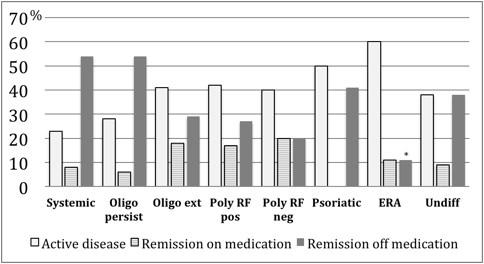
Remission off medication (CR) was documented in 44%, but still 39.8% had active disease (Fig. 1). Extensive variability was found among the categories. Achievement of CR was most often seen in persistent oligoarticular and systemic arthritis in contrast to the lowest rate observed in ERA (*:p<0.001, fig 1).
Conclusion: A significant proportion of the JIA cohort does not reach remission despite new treatment options. Notably more than one third receive systemic treatment even 18 years after disease onset. The worst outcome was evident in the ERA category and in general the JIA disease burden in adulthood remains extensive.
Figure 1: Disease status 18 years after disease onset (n=329)
To cite this abstract in AMA style:
Glerup M, Rypdal V, Arnstad ED, Ekelund M, Peltoniemi S, Aalto K, Rygg M, Toftedal P, Nielsen S, Fasth A, Berntson L, Nordal E, Herlin T. Remission Status after 18 Years of Follow-up in the Population-Based Nordic Juvenile Idiopathic Arthritis (JIA) Cohort [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/remission-status-after-18-years-of-follow-up-in-the-population-based-nordic-juvenile-idiopathic-arthritis-jia-cohort/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/remission-status-after-18-years-of-follow-up-in-the-population-based-nordic-juvenile-idiopathic-arthritis-jia-cohort/