Session Information
Session Type: Poster Session B
Session Time: 8:30AM-10:30AM
Background/Purpose: Medication adherence is essential to establishing and maintaining disease remission among SLE patients. Patients’ beliefs about treatment influence engagement and adherence to therapy. We previously found racial disparities in medication adherence between White and non-White SLE patients, but racial differences in beliefs about medications have not been well explored. In this study, we investigated differences in medication beliefs and their association with medication adherence between White and non-White SLE patients.
Methods: Patients meeting ACR or SLICC SLE criteria completed the 18-item Beliefs about Medicines Questionnaire (BMQ), which measures four belief domains: disease-specific medication necessity, disease-specific medication concern, general medication overuse, and general medication harm. Adherence was measured using the Domains of Subjective Extent of Nonadherence (DOSE- nonadherence) questionnaire. Due to small numbers of patients who identified as Asian and Hispanic, they were grouped with Black patients and analyzed as non-White. We compared median BMQ scores between White and non-White patients, and explored differences in BMQ scores between adherent and non-adherent patients by race.
Results: This analysis included 102 patients (48 White, 48 Black, 5 Asian, 1 Hispanic, mean age 50, 96% female, 33% < college education, 54% private insurance). For the 18 individual questions, 11 produced answers that were statistically different between the White and non-White patients. Compared to Whites, non-White patients had more general beliefs that medications are harmful (8.5 [interquartile range (IQR) 7-10] vs 7 [IQR 5-9], p=0.005) and overused (11 [IQR 9-12] vs 8.5 [IQR 8-10], p=0.003).
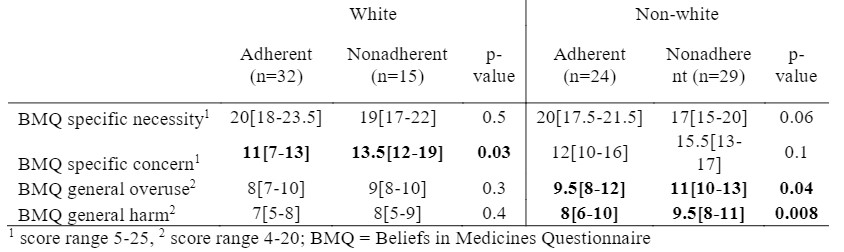
While 71% of White patients reported adherence, only 44% of non-White patients reported adherence. Among White patients, those who were nonadherent reported more SLE-specific medication concerns. In contrast, among non-White patients, those who were non-adherent reported more general beliefs that medications are harmful and overused (Table 1).
Conclusion: We found significant differences in medication beliefs between White and non-White SLE patients with the greatest difference in general beliefs about medications. These racial differences in medication beliefs were also present in adherence data, with non-adherence in the White group being driven by specific concerns about SLE medications while non-adherence in the non-White group was driven by general concerns about medications. These results suggest adherence interventions tailored to race may be more effective, with a focus on building trust in the non-White community. Future studies should investigate the relationship between medication beliefs and SLE outcomes. The extent to which racial differences in medication beliefs may be driven by mistrust in the medical system and systemic racism also deserves further study.
To cite this abstract in AMA style:
Anderson D, Eudy A, Clowse M, Sadun R, Rogers J, Criscione-Schreiber L, Doss J, Volis C, Coles T, Sun K. Racial Differences in Medication Beliefs Among SLE Patients [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/racial-differences-in-medication-beliefs-among-sle-patients/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/racial-differences-in-medication-beliefs-among-sle-patients/