Session Information
Date: Tuesday, November 12, 2019
Title: Pediatric Rheumatology – ePoster III: Systemic JIA, Fever, & Vasculitis
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Mental health disorders are thought to be common in patients with rheumatic disease, but studies examining behavioral issues in patients with juvenile idiopathic arthritis (JIA) have shown mixed results. This may be because JIA comprises a heterogeneous group of diseases and few studies examine psychopathology in different subtypes and disease activity states. This study aims to evaluate emotional and behavioral symptoms in children with juvenile spondyloarthritis (SpA) and polyarticular arthritis (PolyA) as compared to a national normative population using the Child Behavior Checklist (CBCL), and the relationship between CBCL scores and disease activity.
Methods: In this cross-sectional study, patients with JIA aged between 6 and 17 years were recruited at follow-up visits from our Pediatric Rheumatology clinic from April 2018 to April 2019. Patients meeting the ILAR criteria of enthesitis-related arthritis, undifferentiated arthritis or psoriatic arthritis and those with IBD-related arthritis or reactive arthritis were classified as SpA, while PolyA included those meeting the ILAR criteria for polyarticular JIA or extended oligoarticular JIA. Patients with active IBD and severe psoriasis (involvement of BSA >10%) were excluded. After enrollment, parents filled out the CBCL for their children while both providers and parents contributed to the Juvenile Arthritis Disease Activity Score (JADAS) using the clinical JADAS10. We abstracted demographic and clinical data from the charts and presented the findings for the two arthritis groups. Primary outcome measures were CBCL total competence, internalizing, externalizing and total problem raw scores. We compared the outcomes from each group to the national CBCL normative data. As exploratory analyses, we also looked at OCD problem scores, self-harm, and individual internalizing and externalizing syndrome scores which were identified apriori. To investigate the relationship between CBCL scores and disease activity, we ran a generalized linear regression model for all arthritis patients with JADAS as the main predictor to control for age, sex and medical co-morbidities.
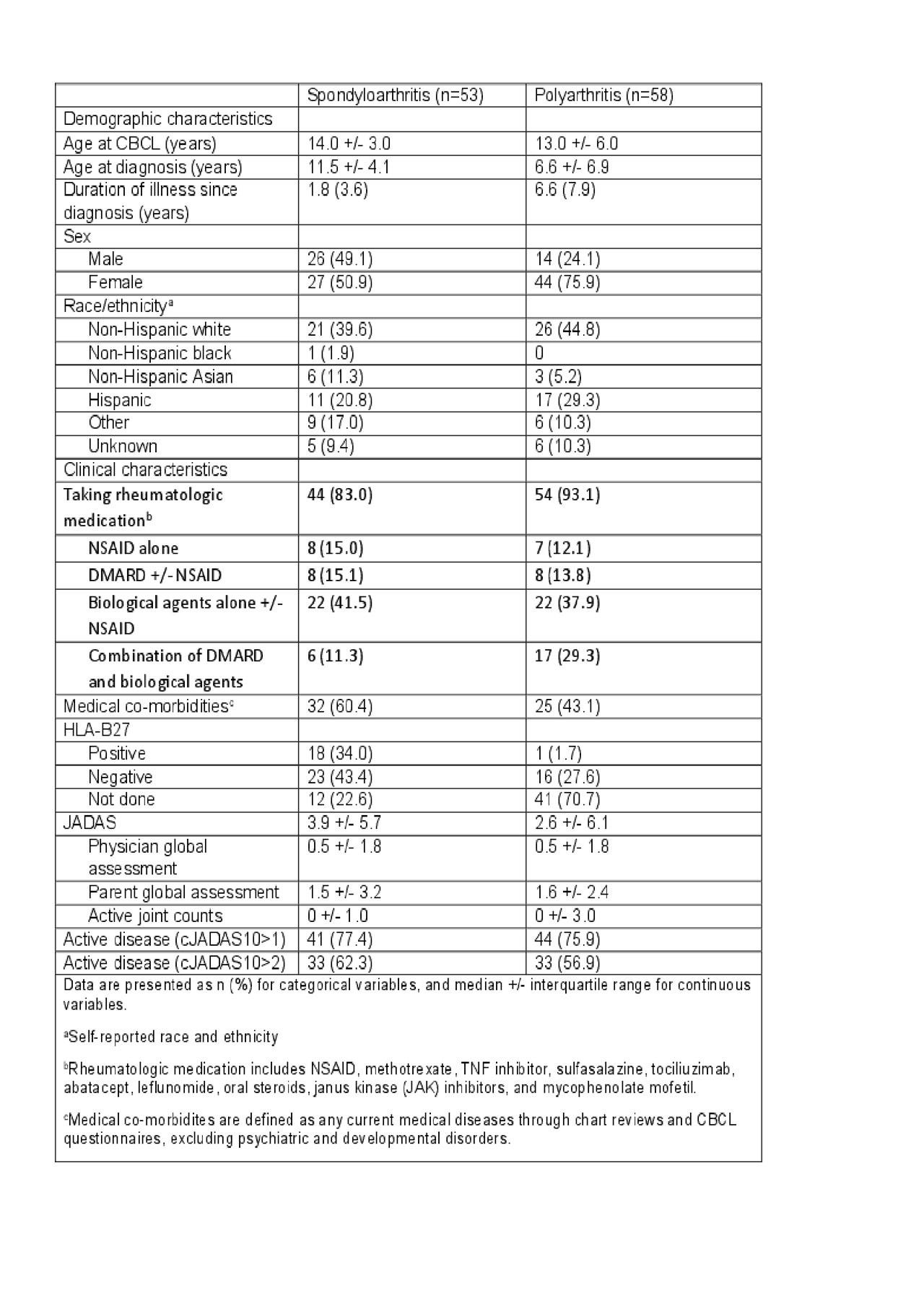
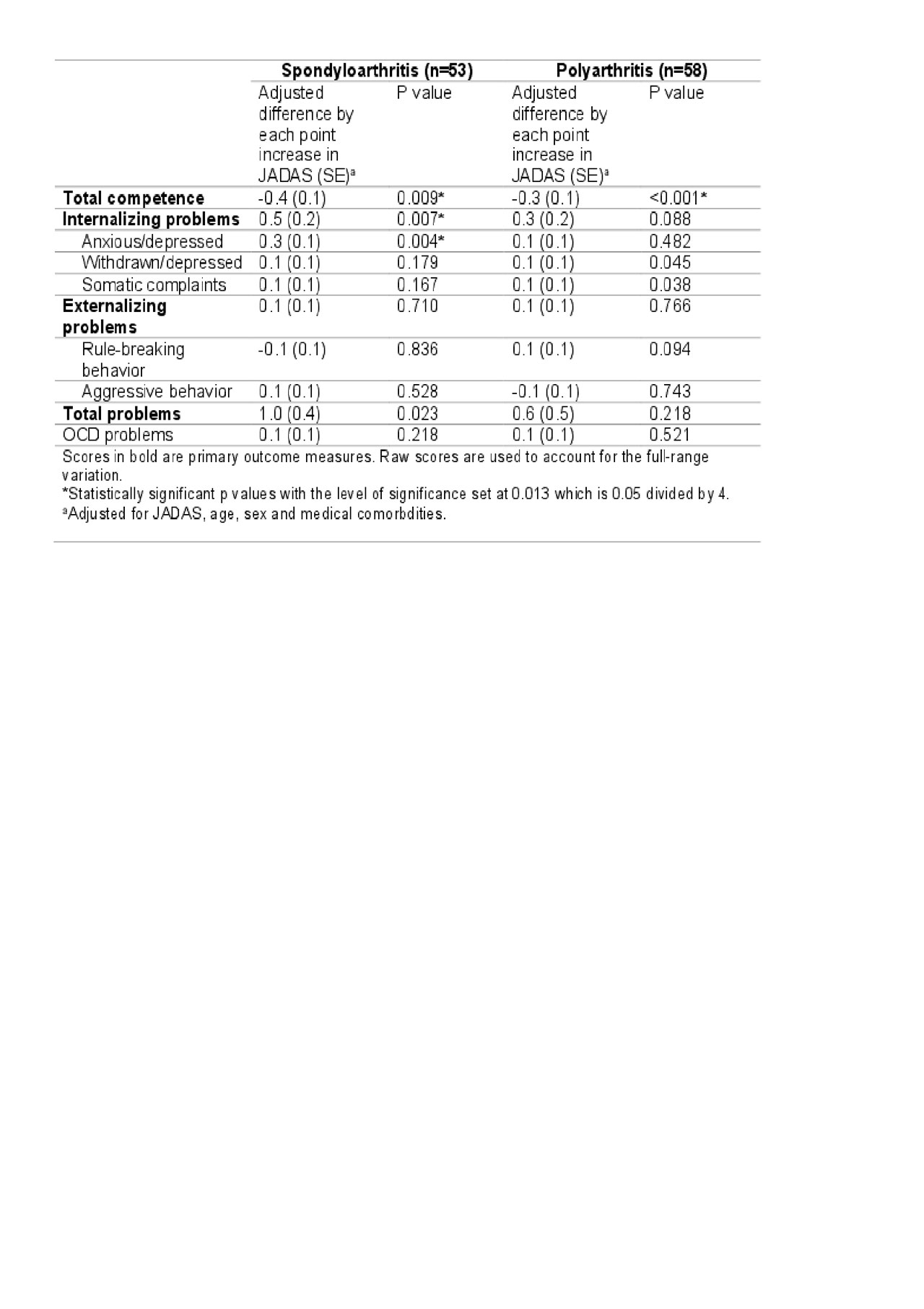
Results: Our study includes 111 patients (53 with SpA and 58 with PolyA) and 1753 healthy controls. Median age at enrollment is 13-14 years. Most of our patients were on arthritis medications at the time of completing CBCL (table 1). When compared to healthy controls, patients with SpA or PolyA had worse total competence and internalizing scores (mainly driven by somatic complaints) but better externalizing scores. Self-harm was almost four times more likely in patients with PolyA than healthy controls (table 2). Higher JADAS was associated with worse total competence scores, worse internalizing scores (mainly driven by anxiety/depression) and higher total problem scores (table 3). Most of these differences reached statistical significance (p< 0.01).
Conclusion: Our study shows patients with arthritis and more active disease have worse total competence scores and internalizing scores reported by parents, suggesting functional deterioration in activities, school and socialization and more internalized emotional disturbances.
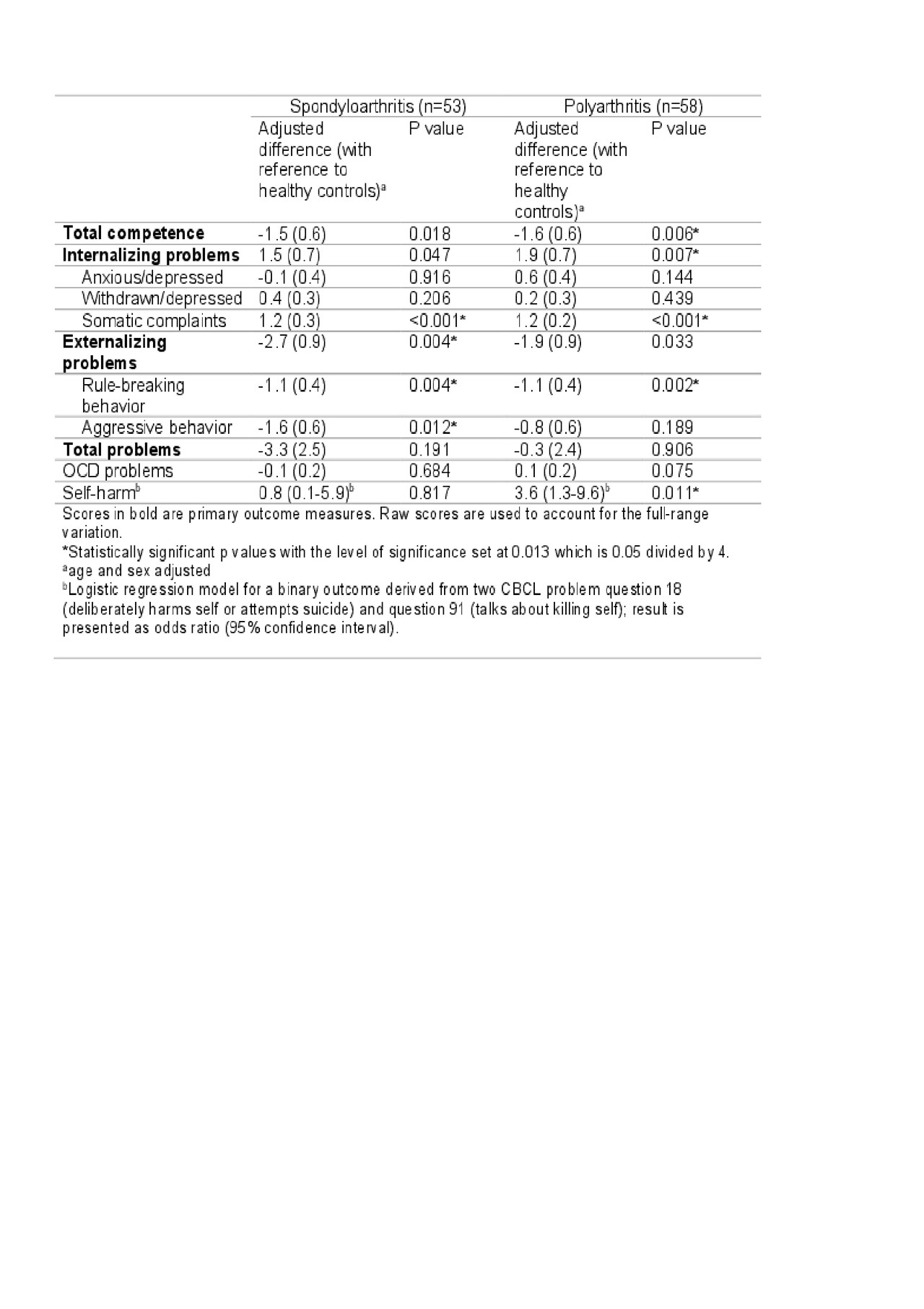
Table 2_comparison with control
To cite this abstract in AMA style:
McHugh A, Chan A, Herrera C, Thienemann M, Frankovich J. Profiling Behavioral and Psychological Symptoms in Children with Spondyloarthritis and Polyarthritis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/profiling-behavioral-and-psychological-symptoms-in-children-with-spondyloarthritis-and-polyarthritis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/profiling-behavioral-and-psychological-symptoms-in-children-with-spondyloarthritis-and-polyarthritis/