Session Information
Date: Monday, November 14, 2016
Title: Systemic Lupus Erythematosus – Clinical Aspects and Treatment III: Novel and Current Therapies
Session Type: ACR Concurrent Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose:
Non-adherence to treatment, a major cause of continued lupus activity and flares, may be difficult to recognize. In this international prospective study, we evaluated adherence to hydroxychloroquine (HCQ) in systemic lupus erythematosus (SLE) patients with flares (ClinicalTrials.gov: NCT01509989).
Methods:
This study included 305 SLE patients (who all met the SLICC criteria) from 19 centers in 10 countries, all of whom had been prescribed HCQ for at least 2 months and were having a disease flare according to the SELENA-SLEDAI Flare Index. Adherence to HCQ was assessed by (1) blood concentrations of HCQ and its main metabolite desethylchloroquine ([HCQ] <200ng/ml and/or undetectable [DCQ] defining severe non-adherence by dosage), (2) self-questionnaires (MASRI<80% and/or Morisky<6 defining non-adherence by questionnaires), and (3) physician’s assessments (on a VAS 0-100).
Results:
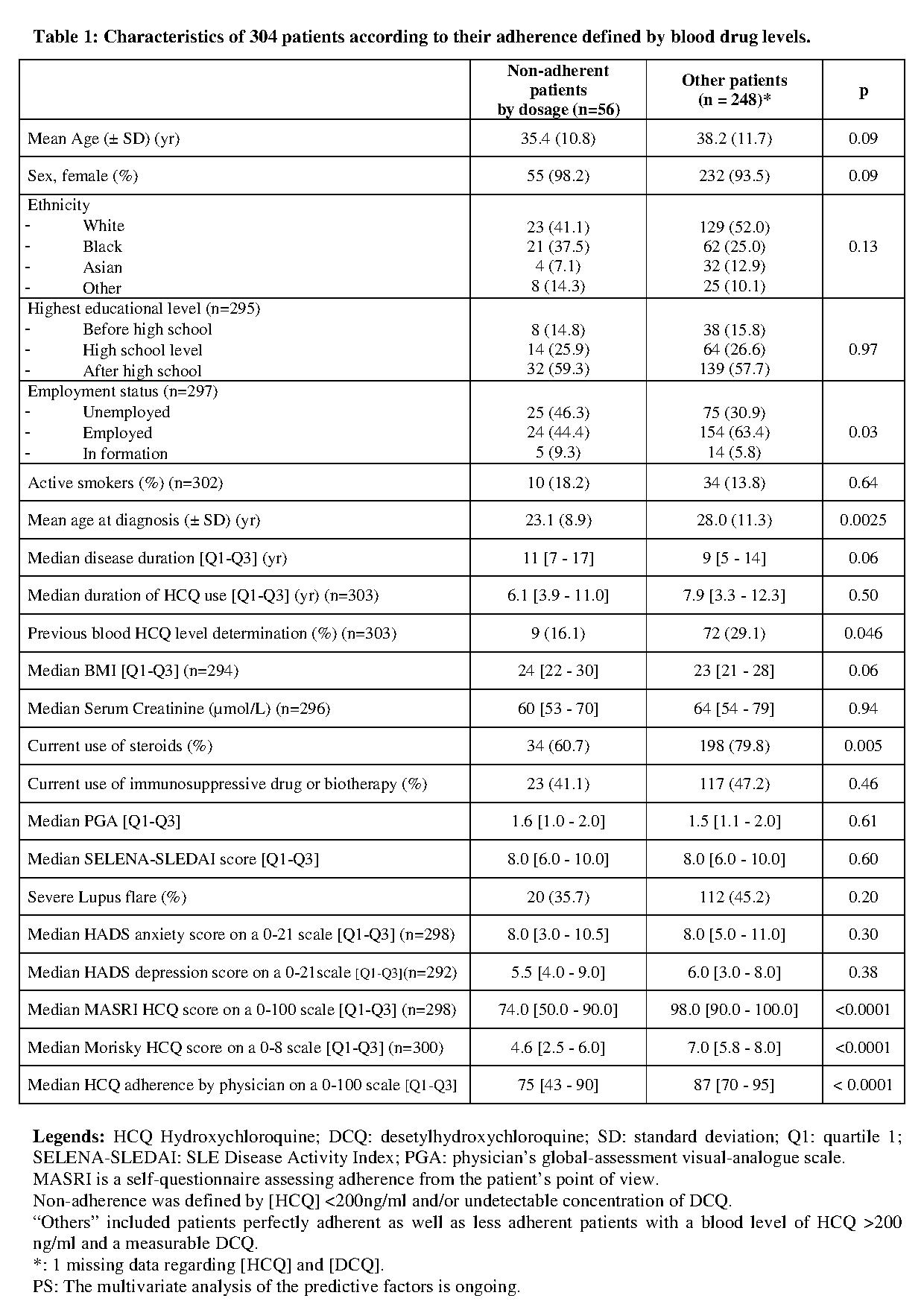
305 patients (288 women; mean age 38±12ys) met the inclusion criteria. Fifty-six patients (18.4%) were severely non-adherent by dosage (1 missing data point): 44 patients (14.5%) had [HCQ] <200ng/ml and 12 additional patients (3.9%) had an undetectable concentration of DCQ indicating a very recent resumption of treatment. Comparison between non adherent and adherent patients is summarized in table 1. These 56 non-adherent patients by dosage were younger at SLE diagnosis (28±11 vs 23±9; p=0.0025), more likely to be unemployed (46.3% vs 30.9%; p=0.03), and less likely treated with steroids (60.7% vs 79.8%; p=0.0050), whereas their exposure to immunosuppressive drugs was not different. Drug level assessment at inclusion was most often their first drug measurement (84% vs 71%, p=0.046). Their anxiety and depression scores (on the HADS questionnaire) were not different from those of the other patients. Even if their median MASRI and Morisky scores were statistically significantly lower, 24 non adherent patients (43%) would still have been defined as adherent by at least one questionnaire. Moreover, even if the median [Q1-Q3] physician’s adherence rating was statistically significantly lower in these 56 patients (75 [43-90] vs 87 [70-95], p<0.0001), their expert physicians considered that 42 patients (75%) took at least half of their treatment and even that 24 (43%) took at least 80% of their treatment.
Among the 305 patients, 121 (39.9%) were non adherent by self-questionnaires. The total non-adherence (dosage + self-questionnaires) was 47%, with only 7% of the patients being classified as non-adherent by both methods.
Conclusion:
These data show that blood HCQ and DCQ measurements objectively identify significant non-adherence in nearly 20% of SLE patients who are flaring. Non-adherence can be missed by the physician and underreported by the patient strongly suggesting the usefulness of blood assays in this setting and the value of using different methods to increase the likelihood of diagnose of non adherence.
To cite this abstract in AMA style:
Costedoat-Chalumeau N, Houssiau FA, Izmirly PM, Le Guern V, Navarra SV, Jolly M, RUIZ-IRASTORZA G, Hachulla E, Agmon-Levin N, Shoenfeld Y, Dall'Ara F, Buyon JP, Deligny C, Cervera R, Lazaro E, Bezanahary H, Baron G, Leroux G, Morel N, Viallard JF, Pineau C, Galicier L, van Vollenhoven R, Tincani A, Nguyen H, Gondran G, Zahr N, Pouchot J, Piette JC, Petri M, Isenberg DA. Predictive Factors of Adherence to Treatment in an International Prospective Study of Blood Hydroxychloroquine Levels in SLE Patients with Flares [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/predictive-factors-of-adherence-to-treatment-in-an-international-prospective-study-of-blood-hydroxychloroquine-levels-in-sle-patients-with-flares/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/predictive-factors-of-adherence-to-treatment-in-an-international-prospective-study-of-blood-hydroxychloroquine-levels-in-sle-patients-with-flares/