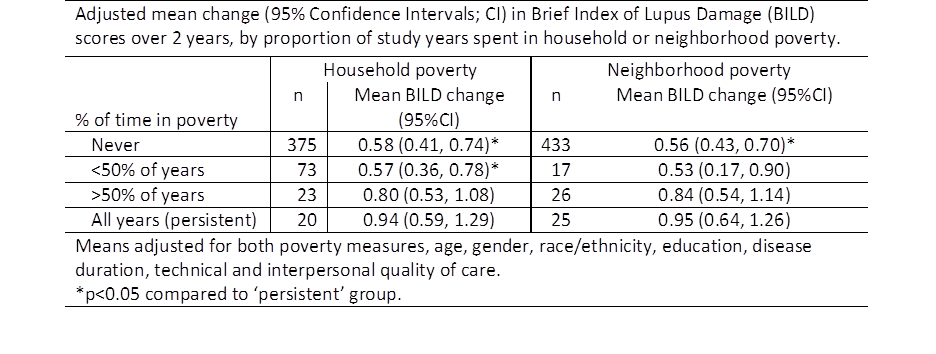Session Information
Date: Monday, November 9, 2015
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Title: Persistent
Individual and Neighborhood Poverty Are Independent Risk Factors for
Accumulated Lupus Damage
Background/Purpose: Previous
research in systemic lupus erythematosus (SLE) has shown that individual
poverty and living in an area of concentrated poverty are both associated with
poor health outcomes. The present study evaluates whether persistent poverty or
persistently living in a neighborhood with a high concentration of poverty is
associated with accumulated disease damage in SLE, in comparison to those who
are intermittently or never in those circumstances.
Methods: Data derive from the
UCSF Lupus Outcomes Study, a national cohort of persons with SLE interviewed
annually since 2003. Interview data were augmented through geocoding with data from participants’
census block group (600-3000 residents), the study definition of a neighborhood.
The survey includes measures of demographic characteristics, socioeconomic
status, technical and interpersonal quality of healthcare, and disease status.
Individual poverty status was calculated annually, defined as household income ≤125%
of the Federal poverty level (<FPL). Concentrated poverty was calculated for
each address, and defined as living in a census block group in which >30% of
households <FPL. Persistent individual and neighborhood poverty were defined
as being poor or in a poor neighborhood at each of the five or more interview
years. The Brief Index of Lupus Damage (BILD), a validated self-report
measure, was collected in 2012-13 and 2014-15. We modeled the 2 year change in
BILD as a function of the proportion of interviews in which participants’
incomes were <FPL, and the proportion in which they lived in concentrated
poverty, controlling for gender, age, racial/ethnic minority status, disease
duration, education, and two measures of quality of care (pass rate of ≥
85% on technical quality of care indicators vs. not and summary of ratings of
interactions with providers and health systems).
Results: Analysis included 501
participants with ≥ 5 interviews and complete data on all variables of
interest. Mean age was 54 ± 12 yrs., mean duration 20 ± 9 yrs., 35% were non-white,
25% had ≥ 1 year in individual poverty, and 14% lived in a concentrated
poverty neighborhood for ≥ 1 year. Mean BILD score at
baseline was 2.9 ±2.6 (range 0-18); mean 2-year change in BILD was 0.44 ± 0.75
(range 0-5). Persistence in both individual and neighborhood poverty were
associated with increased BILD scores. Results from the multivariable linear
regression model shown in table.
Conclusion: In this national
sample of individuals with SLE followed for up to 11 years, persistent
individual and neighborhood poverty were independently predictive of increased
accumulated lupus damage, even after adjustment for other characteristics known
to affect SLE outcomes. Persistent individual and neighborhood poverty are
strong markers for future accumulation of damage.
To cite this abstract in AMA style:
Trupin L, Rush S, Yazdany J, Yelin EH. Persistent Individual and Neighborhood Poverty Are Independent Risk Factors for Accumulated Lupus Damage [abstract]. Arthritis Rheumatol. 2015; 67 (suppl 10). https://acrabstracts.org/abstract/persistent-individual-and-neighborhood-poverty-are-independent-risk-factors-for-accumulated-lupus-damage/. Accessed .« Back to 2015 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/persistent-individual-and-neighborhood-poverty-are-independent-risk-factors-for-accumulated-lupus-damage/