Session Information
Date: Monday, October 22, 2018
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose:
Patients with moderate-to-severe hip or knee arthritis often use opioids before undergoing total joint replacement (TJR). Preoperative opioid use may lead to persistent opioid use and poor clinical outcomes after TJR. We aimed to describe patterns of opioid use before TJR.
Methods:
Using Medicare (Parts A/B/D, 2010-2014) data, we conducted a cohort study among patients aged ≥65 who underwent incident total hip replacement (THR) or total knee replacement (TKR). Index date was the incident TJR date. Eligible patients were required to have continuous enrollment in Part A/B/D for at least 360 days before the index date. We excluded patients with: 1) no medical and/or pharmacy claims in the 360-days before the index date, and 2) both THR and TKR on the same date. Any opioid use was defined as having ≥1 opioid dispensing during the 12-month period; continuous opioid use was characterized as having ≥1 opioid dispensing in each of 12 months during the before the index date. We calculated mean morphine milligram equivalent (MME) per day and proportion of days covered (PDC) in each month. 50 MME is equivalent to 50 mg hydrocodone. We assessed variables potentially associated with opioid use, such as demographics, pain/fractures, other comorbidities, medication use, and healthcare use in 360 days prior to the surgery. A multivariable logistic regression model estimated the associations between patient characteristics and preoperative opioid use patterns.
Results:
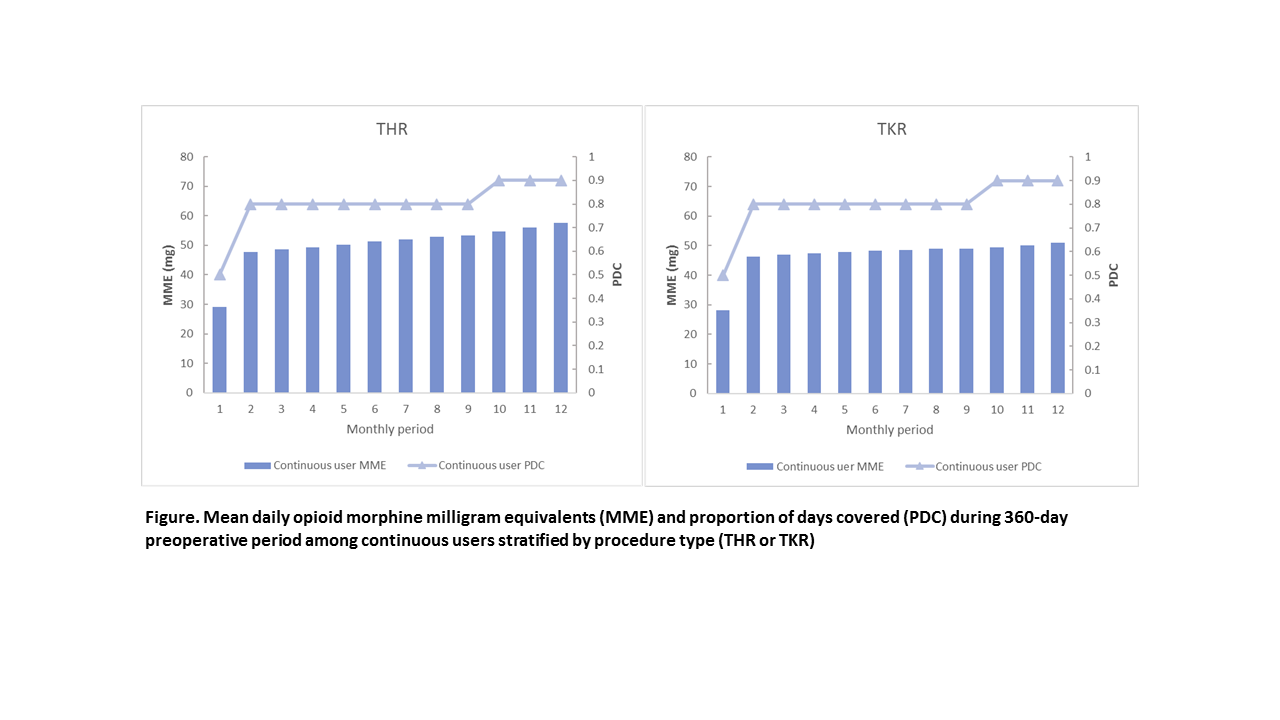
We identified a total of 473,781 patients who underwent TJR: 155,516 THR and 318,265 TKR. Mean (SD) age was 75 (7) years for THR and 74 (6) for TKR patients. 67.4% were female and 91.5% were White. Back pain was a common comorbidity in both THR (62%) and TKR (46.8) patients. 60.2% patients had any use of opioids before the surgery. Of those, 12.4% used opioids at least once a month continuously over the 12-month preoperative period. Hydrocodone was most commonly used agent, followed by tramadol and oxycodone. Among any users of opioids, MME per day and PDC both increased toward the TJR date. Continuous opioid users had over 90% PDC in the month before TJR and used higher MME dose of opioids per day (58mg in THR, 51mg in TKR) compared to any users (16mg in THR, 12mg in TKR) (p-values <0.0001) (Figure). Correlates of continuous opioid use included history of drug abuse (OR=5.19, 95% CI=3.96-6.84) and back pain (OR=2.32, 95% CI=2.24-2.40). African American patients had a 2-fold higher odds of using opioid continuously compared with White Americans (OR=2.14, 95% CI=2.01-2.28).
Conclusion:
Among patients in Medicare who underwent TJR, 60.2% had any use of opioids and 7.5% had continuous use of opioids in the year before the surgery. Use of opioids and MME increased gradually toward the index TJR date. History of drug abuse, back pain, and race African American were strongly associated with continuous use of opioids preoperatively.
To cite this abstract in AMA style:
Jin Y, Solomon D, Franklin PD, Lee YC, Lii J, Katz JN, Kim SC. Patterns of Opioid Use and Patient Characteristics before Total Hip and Knee Replacement [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/patterns-of-opioid-use-and-patient-characteristics-before-total-hip-and-knee-replacement/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/patterns-of-opioid-use-and-patient-characteristics-before-total-hip-and-knee-replacement/