Session Information
Session Type: Abstract Submissions
Session Time: 5:30PM-7:00PM
Background/Purpose: Pediatric rheumatology patients are at high risk for the development of pulmonary disease. Lung disease in these patients can go unnoticed for long periods of time, and carry significant morbidity and mortality. The importance of screening and monitoring for pulmonary manifestations in these patients is clear; however, many screening methods may be costly and difficult to administer. Pulse oximetry has been shown to be a useful screening tool for the ambulatory monitoring of COPD and certain types of interstitial lung disease. Despite this, pulse oximetry is rarely used as a routine measurement in the clinic setting. We therefore designed a pilot study to determine feasibility of in-clinic pulse oximetry to help determine when there is need for more in depth screening.
Methods: Baseline measurements of oxygen saturation (O2 sat) recordings were collected for all patients attending clinic at our institution. Measures were then implemented to improve these rates, including speaking with clinic nurses, clear signage, and working with information technology to include O2 sat in the vitals section in the electronic medical record system. This study was exempt from full review, and approved by the institutional IRB.
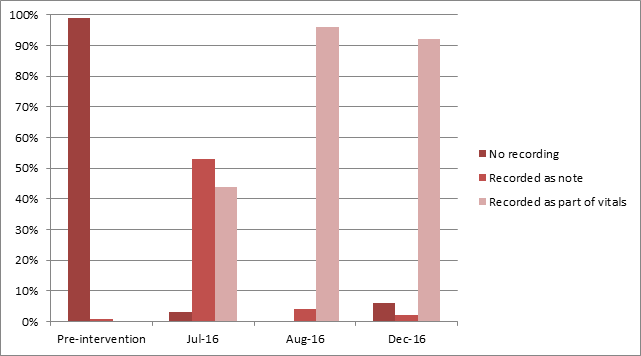
Results: As seen in figure 1, recordings of O2 sat increased from 1% to 94% during this period. Over the study period, O2 sat was also increasingly recorded as part of vital signs, where it could be easily accessed. As part of the intervention, one patient was found with abnormal pulse oximetry leading to further evaluation.
Conclusion: This study reveals that initiatives to increase O2 sat recordings in a clinic setting are effective and easily achieved. Research is ongoing about the best methods to screen for pulmonary disease in these patients who are at high risk.[i]The utility of post exercise and spirometry will be evaluated as ambulatory screening tools. Further research is needed to determine the efficacy of longitudinal O2 sat recordings as a screening tool for lung disease in pediatric rheumatology patients.
Figure 1. Oxygen Saturation Recordings
[i] Gabor Kovacs et al., “Use of ECG and Other Simple Non-Invasive Tools to Assess Pulmonary Hypertension,” PloS One 11, no. 12 (2016): e0168706, doi:10.1371/journal.pone.0168706; Suparaporn Wangkaew et al., “Correlation of Delta High-Resolution Computed Tomography (HRCT) Score with Delta Clinical Variables in Early Systemic Sclerosis (SSc) Patients,” Quantitative Imaging in Medicine and Surgery 6, no. 4 (August 2016): 381–90, doi:10.21037/qims.2016.08.08; Benjamin E. Schreiber et al., “Improving the Detection of Pulmonary Hypertension in Systemic Sclerosis Using Pulmonary Function Tests,” Arthritis and Rheumatism 63, no. 11 (November 2011): 3531–39, doi:10.1002/art.30535.
To cite this abstract in AMA style:
Trachtman R, Adams A, Pan N, Taber S, Onel K. Oxygen Saturation Recordings in Pediatric Rheumatology Patients At Risk For Lung Disease [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 4). https://acrabstracts.org/abstract/oxygen-saturation-recordings-in-pediatric-rheumatology-patients-at-risk-for-lung-disease/. Accessed .« Back to 2017 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/oxygen-saturation-recordings-in-pediatric-rheumatology-patients-at-risk-for-lung-disease/