Session Information
Session Type: ACR Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Understanding a patient’s status before entering the exam room, or accurately tracking status between visits, is vital to creating more efficient ways to apply patient care. We studied which patient-derived dataset resulted in the most accurate diagnosis for common clinical scenarios encountered in rheumatoid arthritis (RA) management.
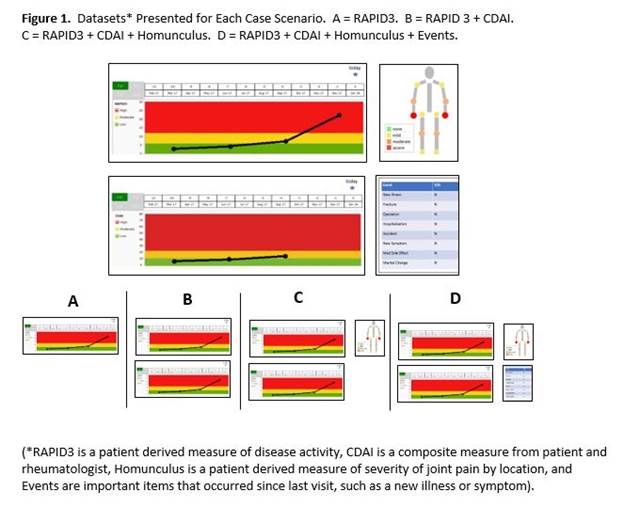
Methods: 3 clinical cases were created for 4 RA scenarios: Acute Flare–RA, Chronic Active–RA, Acute Flare–Not RA, and Chronic Active–Not RA. To see which data most accurately predicted the clinical scenario, 4 datasets were developed (Figure 1): Dataset A (RAPID3), B (RAPID3 + CDAI), C (RAPID3 + CDAI + Homunculus), and D (RAPID3 + CDAI + Homunculus + Events). CDAI included only values from previous office visits, so the dataset could be derived without physician input. 12 rheumatologists were given randomly assembled packets with 48 cases (3 cases x 4 scenarios x 4 datasets). For each case, the rheumatologist decided which of the 4 RA scenarios the dataset represented, as well as how confident they were in their decision (10-point Likert scale). Comparisons were tested using a Generalized Estimating Equation for logistic regression. Post-hoc comparisons were tested for each incremental amount of data.
Results: Across all scenarios (Table 1), there was an increase in percent correct as more clinical data was presented (p<0.0001). Post-hoc analysis showed improvement in % correct moving from dataset A to B (6.2% vs. 59.0%, p<0.0001) and B to C (59.0% vs. 86.1%, p<0.0001), but not C to D (86.1% vs. 89.6%, p=0.4575). Analysis of specific scenarios showed that dataset C was optimal for Acute Flare–RA and Acute Flare–Not RA. Dataset B was optimal for Chronic Active – RA and Chronic Active – Not RA. Level of confidence was high (8/10) and did not vary by dataset – indicating confidence in decision making regardless of the decision.
Conclusion: To our knowledge, this is the first study that shows the optimal data set to collect from patients between visits or before a visit to accurately diagnose the common clinical scenarios that affect patients with RA. The combination of RAPID3 (historical and current) + CDAI (historical) + pain Homunculus gave the greatest diagnostic accuracy across all clinical phenotypes. These results can inform the design of data collection systems that improve rheumatology efficiency, by empowering the rheumatologist before the visit, and driving return visits based on patient need rather than an arbitrary interval.
To cite this abstract in AMA style:
Newman E, Thomas E, Berger A, Kirchner HL. Optimizing the Dataset to Collect from Patients to Accurately Predict Their Status Prior to the Clinic Visit [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/optimizing-the-dataset-to-collect-from-patients-to-accurately-predict-their-status-prior-to-the-clinic-visit/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/optimizing-the-dataset-to-collect-from-patients-to-accurately-predict-their-status-prior-to-the-clinic-visit/