Session Information
Session Type: Abstract Session
Session Time: 3:00PM-3:50PM
Background/Purpose: According to APS classification criteria1, clinical manifestations of antiphospholipid syndrome (APS) consist in thrombotic and obstetric events, including severe preeclampsia (PE). Because little is known on this topic, our aim was to describe severe PE in a cohort of APS patients and to report the thrombotic and obstetrical outcomes in these patients.
Methods: Retrospective study of female patients referred to 5 French Internal Medicine departments and 1 Italian Rheumatology Unit with a severe PE according to standard definition1, that occurred before 34 WG between 2000 and 2018 in patients with APS2. In case of more than one episode of severe PE in one given patient, we defined the index pregnancy as the first episode. We considered that women had been treated during pregnancy if they were prescribed low-dose aspirin (LDA) and/or low-molecular-weight heparin (LMWH) before the diagnosis of severe PE.
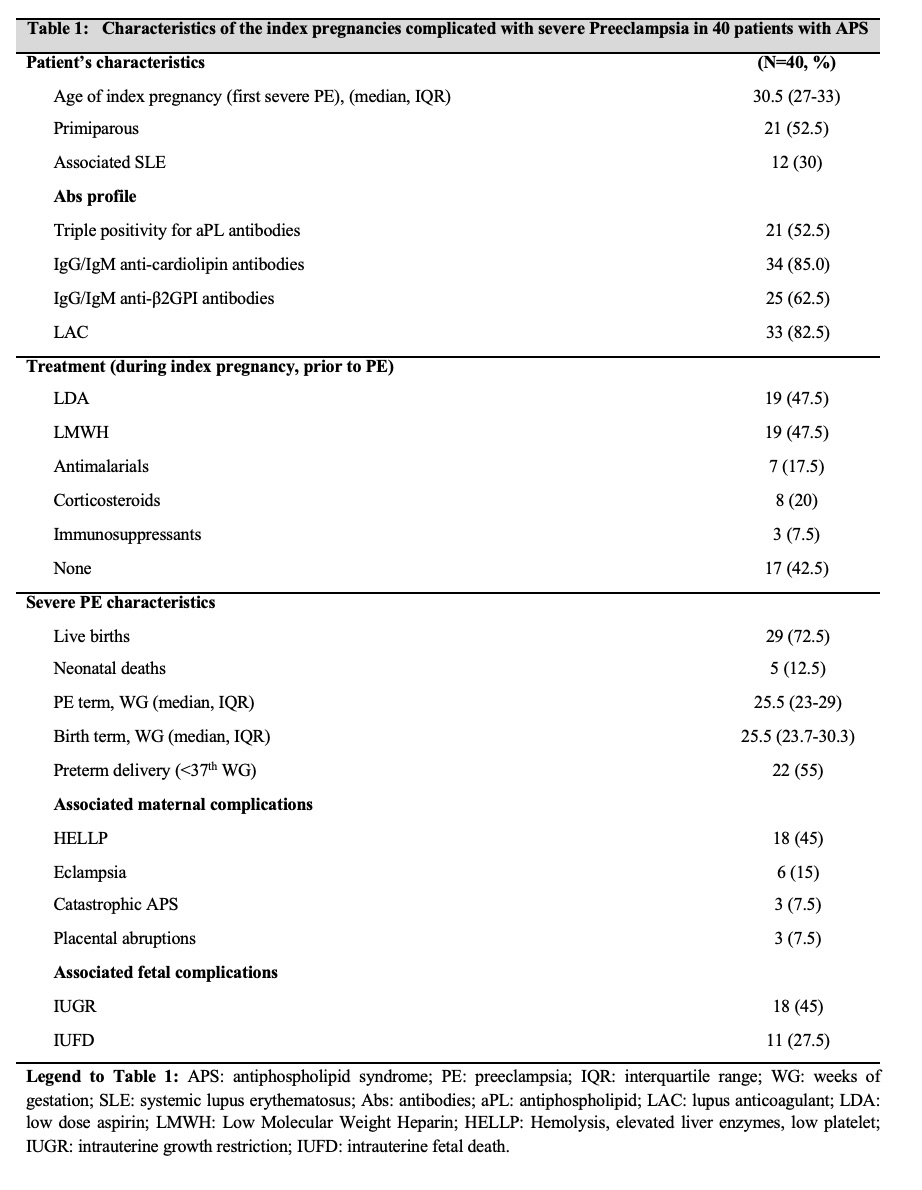
Results: The study included 40 women with APS, with a median follow-up after the index pregnancy with PE of 3 years. 12 (30%) had an associated SLE. 33 women (82.5%) had a positive LAC and 21 women (52.5%) had triple positivity anti-phospholipid (aPL) positivity.
- During the index pregnancy, PE occurred at a median term of 25.5 WG. 29 pregnancies (72.5%) led to a live birth but 5 severely premature neonates died (i.e. a total of 24 pregnancies resulted to a living child). Data on PE are described Table 1.
- Thrombotic criteria: 16 women (40%) had at least one thrombotic event. Their first thrombosis occurred before (n=14) or after the index pregnancy (n=2). Thromboses were venous (n=6), arterial (n=12), and/or micro-thrombotic (n=5). Four patients experienced a catastrophic APS (CAPS), 3 of them simultaneously with PE.
- Obstetrical criteria: when considering all their pregnancy (n=122), 17 patients (42.5%) had at least one intra-uterine fetal death (IUFD), and 19 women (47.5%) had at least one HELLP syndrome. None of the 40 patients presented 3 or more consecutive miscarriages.
Conclusion: During the 40 index pregnancies, severe PE occurred early in the pregnancy with a high rate of in utero (n=11) or neonatal (n=5) mortality of the offspring.
APS was characterized by a strong autoimmune anti-phospholipid serology and SLE was frequent (30%).
Among these 40 APS patients with severe PE, almost half also experienced at least one thrombosis, a HELLP syndrome and/or an IUFD. However, no overlap with the «three consecutive miscarriages” classification criterion was found in our cohort suggesting that the underlying physiopathology of these 2 obstetrical phenotypes are completely different.
References:
- Diagnosis and Management of preeclampsia and eclampsia. International Journal of Gynecology &Obestetrics 2002;77:67-75.
- Miyakis S, et al. International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome (APS). J Thromb Haemost 2006;4:295e 306
To cite this abstract in AMA style:
Larosa M, Morel N, Belhocine M, Ruffatti A, Martin Silva N, Paule R, Mouthon L, Dreyfus M, Piette J, Souchaud-Debouverie O, Deneux-Tharaux C, Tsatsaris V, Pannier Metzger E, Guettrot-Imbert G, Le Guern V, Doria A, Costedoat-Chalumeau N. Obstetrical Outcome and Thromboses in a Multicentric Cohort of Antiphospholipid Syndrome (APS) Patients with Severe Preeclampsia: An Analysis of APS Classification Criteria [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/obstetrical-outcome-and-thromboses-in-a-multicentric-cohort-of-antiphospholipid-syndrome-aps-patients-with-severe-preeclampsia-an-analysis-of-aps-classification-criteria/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/obstetrical-outcome-and-thromboses-in-a-multicentric-cohort-of-antiphospholipid-syndrome-aps-patients-with-severe-preeclampsia-an-analysis-of-aps-classification-criteria/