Session Information
The 2020 Pediatric Rheumatology Symposium, originally scheduled for April 29 – May 2, was postponed due to COVID-19; therefore, abstracts were not presented as scheduled.
Session Type: Poster Breakout Session
Session Time: 5:10PM-5:40PM
Background/Purpose: MRI examination is frequently used to determine the presence of sacroiliitis in patients suspected of having inflammatory arthritis. In children and adolescents, the vascular primary spongiosa of endochondral bone can be misinterpreted as marrow edema and it can be mistaken for evidence of active sacroiliitis. The hypothesis is that a changing but predictable pattern for marrow signal intensity adjacent to the sacroiliac joints is present from infancy through skeletal maturity. We describe MRI features of the sacroiliac joints in children who are not diagnosed with inflammatory arthritis.
Methods: Three hundred fourty-five children who underwent MRI examination of the sacrum, sacroiliac joints, or pelvis were identified in the electronic medical record database. Those with underlying disease that may potentially alter SI signal were excluded (history of associated injury, inflammatory arthritis or JIA, malignancy and treatment with chemotherapy and/or local radiotherapy, anemia or history of psoriasis, CRMO/SAPHO, inflammatory bowel disease or reactive arthritis). Measurements in millimeters of the distance from the joint surfaces bilaterally at the level of the S1, S2, and S3 levels for T1 marrow signal intensity (less than muscle) and T2 marrow signal intensity (greater than muscle) relative to muscle was recorded as well as measurements in millimeters of the distance from the joint surfaces bilaterally at the level of the S1, S2, and S3 levels for T1 and T2 marrow signal intensity equivalent to the primary spongiosa of the iliac crests. Continuous and categorical variables were compared using Student’s t test and Fisher’s test respectively as appropriate. P-value < 0.05 was considered statistically significant.
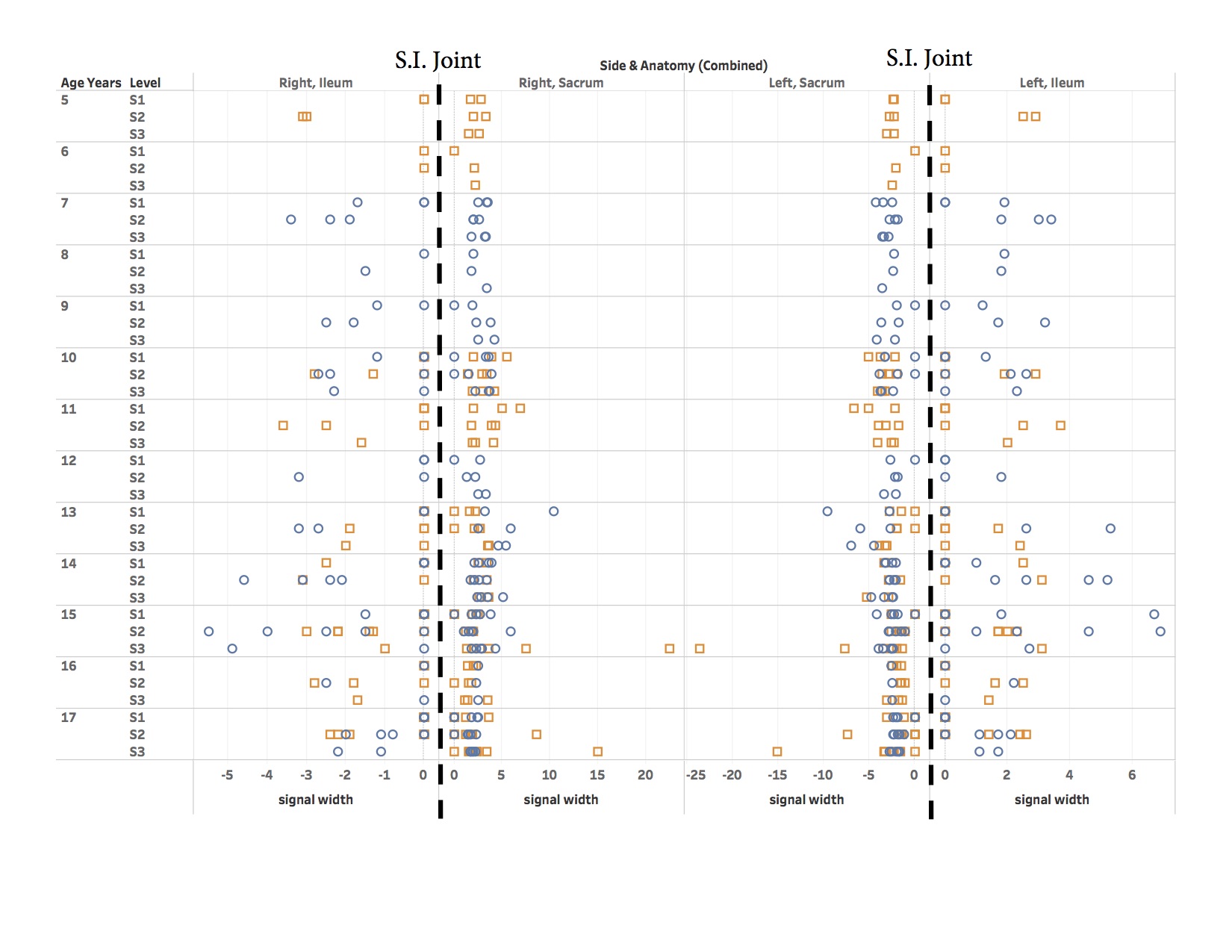
Results: Sixty children (31 females, 29 males) from 2 age groups-pre and peripubertal (8-13 years) versus close to skeletal maturity (14-18 years) met inclusion criteria and had technically adequate examinations to assess sacroiliac joint. Mean age was 13.5 years (SD: 3.64). There was symmetric increased of T2 signal intensity for both the iliac (mean +/- SD: 0.94 mm +/- 1.31 and 1.04 mm +/- 1.51, right and left iliac respectively) and sacral (mean +/- SD: 2.1 mm +/- 1.73 and 2.12 mm +/- 1.57 right and left sacral respectively) marrow adjacent to the sacroiliac joints at the level of the S1 and S2 segments with no difference in width of such marrow present when comparing pre and peripubertal subjects against subjects close to skeletal maturity. Males (48%) and females (52%) differed in only the width of increased T2 sacral marrow averages adjacent to the S2 level (mean +/- SD: 2.17 mm +/- 1.40 and 1.37 mm +/- 1.29, males and females respectively) (p = 0.024).
Conclusion: Healthy children and adolescents normally have increased T2 signal intensity within the sacral and iliac marrow adjacent to the sacroiliac joints, likely representing the vascular primary spongiosum. This is symmetric between sacral and iliac sides and uniform in width from prior to puberty until close to skeletal maturity. Knowledge of this normal pattern is beneficial in interpreting MRI examinations for the presence of sacroiliitis.
To cite this abstract in AMA style:
Borgia R, Woolnough L, Storey T. Normal MRI Appearance of Marrow Adjacent to the Sacroiliac Joints in Healthy Children During Development [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 4). https://acrabstracts.org/abstract/normal-mri-appearance-of-marrow-adjacent-to-the-sacroiliac-joints-in-healthy-children-during-development/. Accessed .« Back to 2020 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/normal-mri-appearance-of-marrow-adjacent-to-the-sacroiliac-joints-in-healthy-children-during-development/