Session Information
Date: Monday, November 9, 2015
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose:
Renal disease in scleroderma (SSc), including
scleroderma renal crisis (SRC), remains a major clinical challenge. Previous
studies showed up to 50% of SSc patients have renal
involvement. We sought to gain insight into the pathogenesis of SSc kidney disease by examining markers of disease in
serum, urine and renal biopsy specimens.
Methods:
We collected urine and serum from 80 SSc patients,
with or without renal involvement, for comparison with patients with kidney
disease of other causes (n=10) and healthy controls (n=12). We performed
multiplex analysis of candidate markers of disease activity or severity in SSc and renal injury: MCP-1, MCP-3, IL-6, IL-18, TNFalpha, and VEGF. In a further experiment we examined
biopsies of patients with SRC using immunostaining
for MCP-1.
Results:
40 SSC patients were in the subgroup with renal involvement (“SSc-CKD”) defined by eGFR,
urinalysis or a history of SRC. Serum MCP-1 was increased in SSc compared with controls, with SSc-CKD
significantly lower than SSc without renal
involvement. Mean serum MCP-1 was 132 pg/ml (95% CI
105-162) for SSc with normal renal function compared
with 65 pg/ml in SSc-CKD
(49-81, p<0.001 for this comparison). MCP-1 was not increased in renal
disease of other causes (mean 47 pg/ml, 23-85)
compared with controls (mean 53 pg/ml, 25-85,
p=0.848). Conversely, urine MCP-1:creatinine ratio was
higher in SSc-CKD (mean 64, 32-111) than in SSc with normal renal function (mean 23, 18-28, p=0.046).
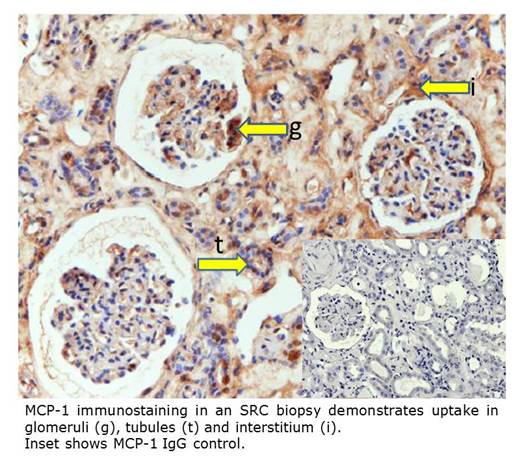
20 SRC cases
confirmed on histology were stained with IgG antibodies for MCP-1 (see figure).
Expression was highest in the tubules, interstitium and vasculature. The number
of typical “onion skin” arterial lesions seen was positively correlated with
the level of MCP-1 expression in the vasculature overall (p=0.048).
Conclusion:
This is the first study to measure MCP-1 in the urine of SSc
patients. Elevated urine MCP-1 in SSc with renal
involvement was corroborated by immunohistochemistry demonstrating marked expression
of the chemokine in the kidneys of affected patients. The identification of
urine MCP-1 as a marker for local expression in the kidney may help define
organ-specific effects of this chemokine, which has previously been reported to
be increased in serum in association with pulmonary complications. Our findings
support further investigation of urine concentrations of MCP-1 as a marker or
mediator of renal disease in SSc.
To cite this abstract in AMA style:
Stern E, Hong C, Ong VH, Burns A, Unwin R, Denton CP. Monocyte Chemoattractant Protein-1 (MCP-1, CCL2) Is a Potential Local Marker of Renal Involvement in Scleroderma [abstract]. Arthritis Rheumatol. 2015; 67 (suppl 10). https://acrabstracts.org/abstract/monocyte-chemoattractant-protein-1-mcp-1-ccl2-is-a-potential-local-marker-of-renal-involvement-in-scleroderma/. Accessed .« Back to 2015 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/monocyte-chemoattractant-protein-1-mcp-1-ccl2-is-a-potential-local-marker-of-renal-involvement-in-scleroderma/