Session Information
Date: Wednesday, October 24, 2018
Title: 6W007 ACR Abstract: Patient Outcomes, Preferences, & Attitudes II: PROs (2910–2915)
Session Type: ACR Concurrent Abstract Session
Session Time: 9:00AM-10:30AM
Background/Purpose:
Lupus patients may experience flares in disease activity that require rapid management. This study describes the experience, identification, and management of a flare from the patient perspective.
Methods:
An online survey was administered to persons with lupus who responded to outreach from the Lupus Foundation of America or the Research Now survey research service. Data collection included sociodemographic characteristics, flare profile, the Lupus Impact Tracker (LIT), and hospital admissions. The results were summarized with descriptive statistics.
Results:
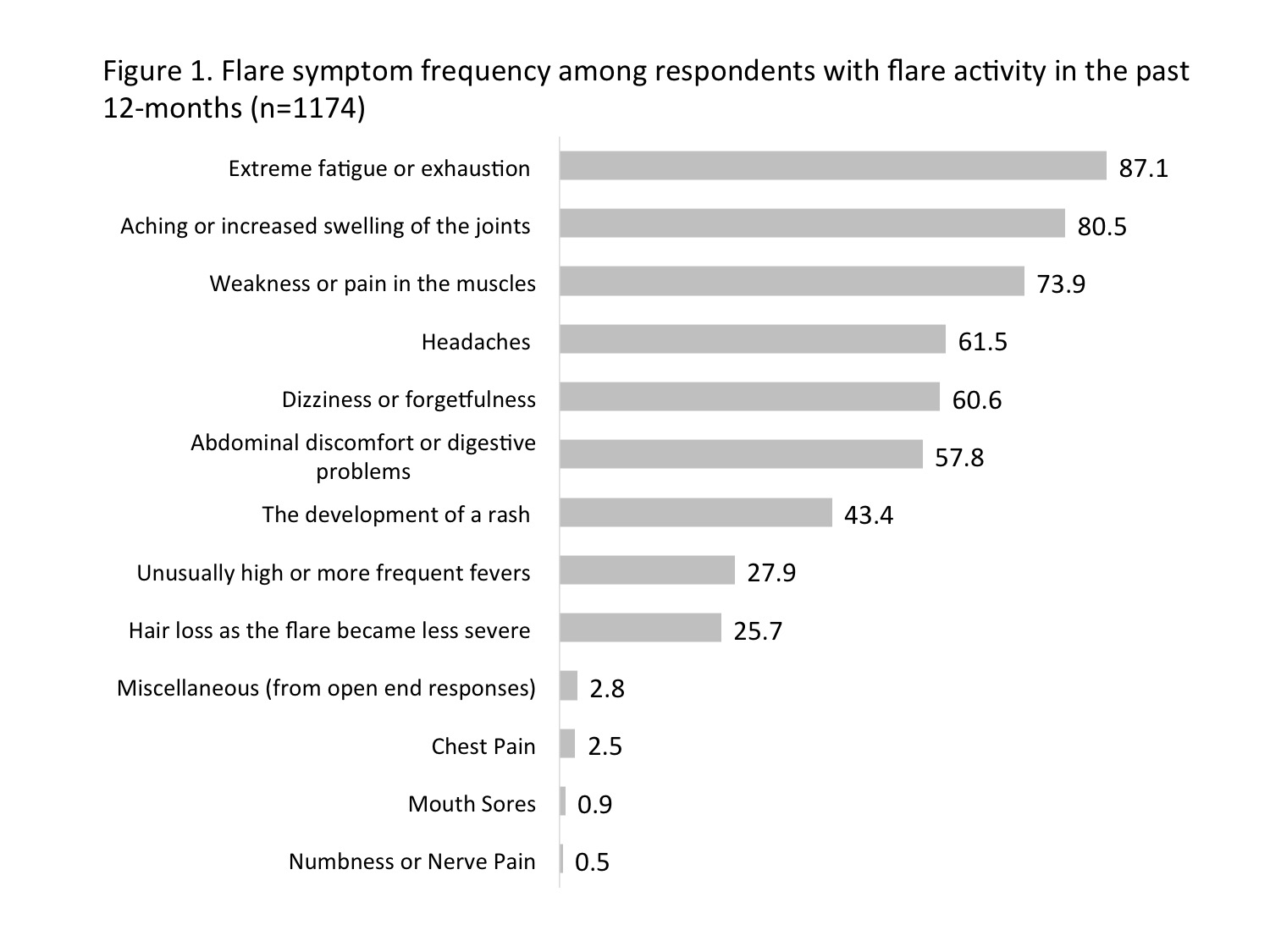
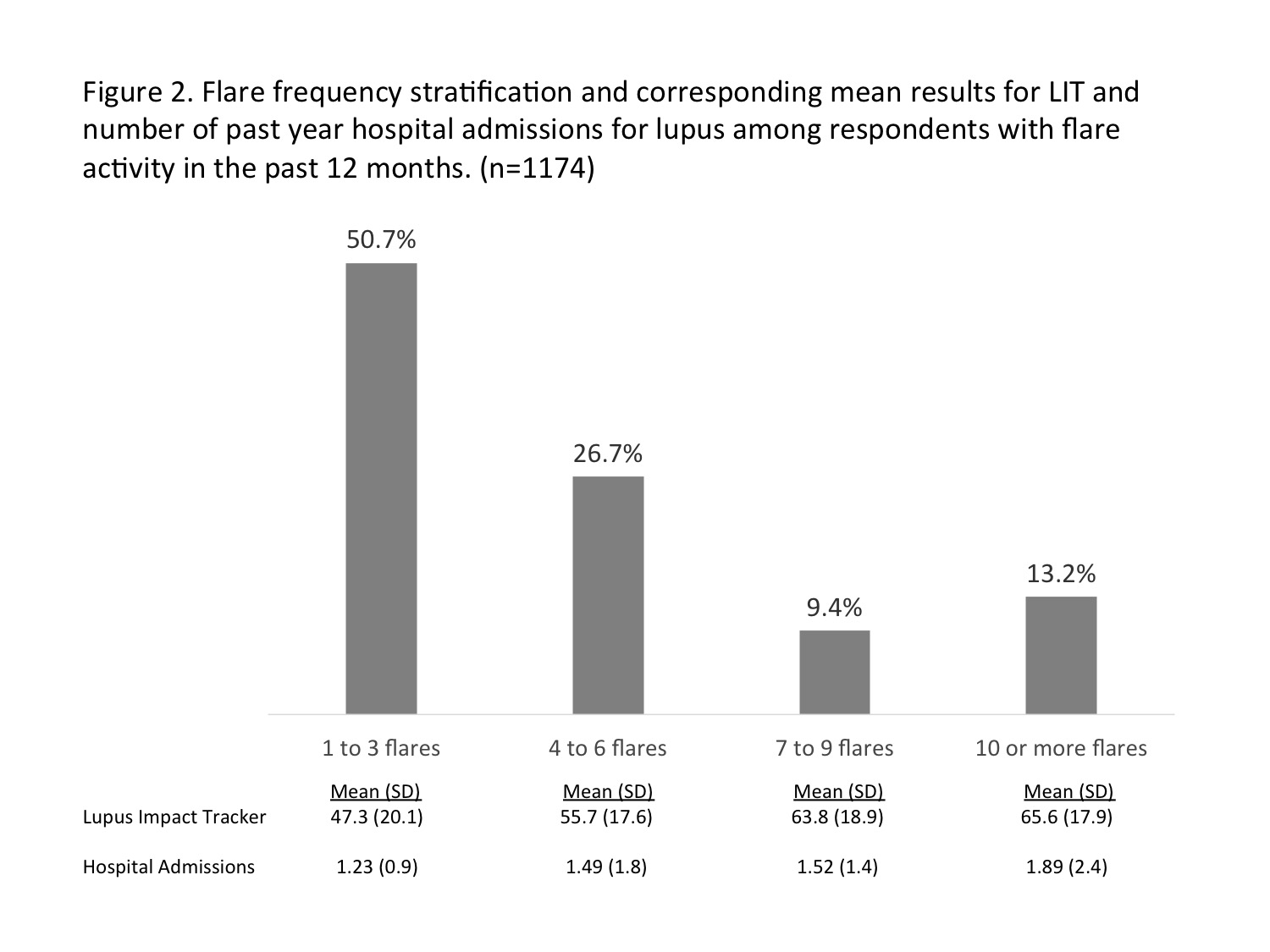
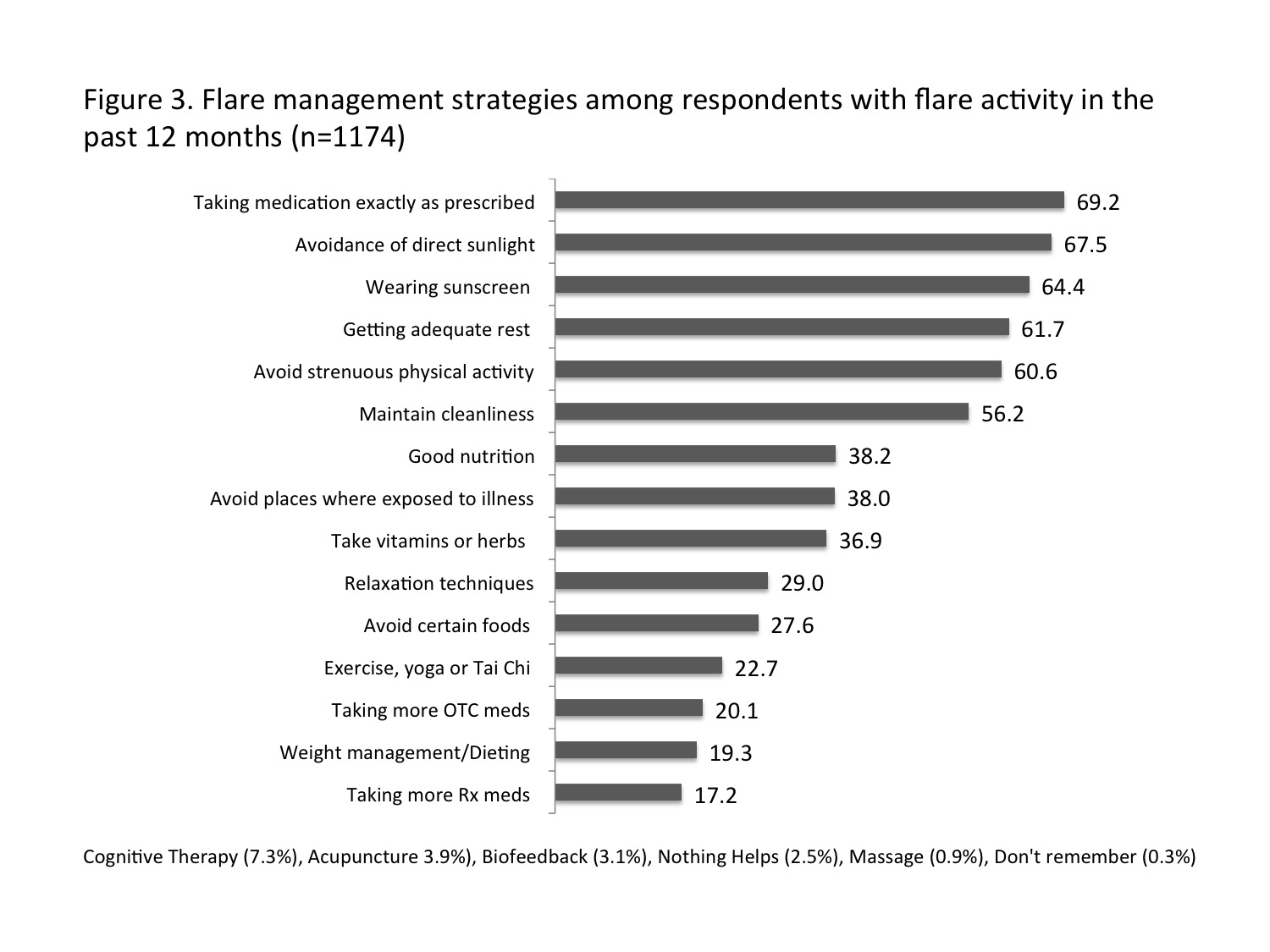
1503 individuals with self-reported lupus completed the survey from May to October 2017. 77% were Caucasian, 89% were female, mean age was 45 yrs, mean duration of illness was 12 yrs, and 19% reside rurally. 78% had flare activity in the past year. Of these, half reported 4 or more flares, and 66.9% perceived their flares as moderate to severe. The most common flare symptoms (Figure 1) were extreme fatigue/exhaustion (87%), aching/increased swelling of the joints (80%), and muscle weakness/pain (74%). Respondents who suffered more flares had worse LIT scores and more hospital admissions during the past year (Figure 2). Many respondents (48%) could not predict when a flare would occur but noted that flare triggers were events such as emotional stress, overdoing it, lack of rest, and sunlight exposure. 40.5% engaged the healthcare system, such as doctor, ER, or hospital, when suffering a flare. 54% self-treated flares, most frequently with over-the-counter products and prescription drugs kept on hand. For the most recent flare 34.8% delayed seeking care for 3 days or longer (24.3% of urban residents, 41.9% of rural); more than half did not receive care within 24 hours (46.1% of urban, 62.2% of rural). Figure 3 shows various tactics used to manage flares.
Conclusion:
Lupus flare burden is high, and flares often resulted in healthcare encounters and medication use. The most common flare symptoms may not be congruent with how clinicians define flares, leading to communication challenges. Patients appear to be receptive to self-treatment, presenting an opportunity to enhance their self-care skills. Findings provide insight into how clinicians and patients can work together to identify and manage flares more effectively.
To cite this abstract in AMA style:
Nelson W, Katz P, Daly RP, Topf L, Connolly-Strong E, Reed M. Lupus Flare Activity from the Patient Perspective [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/lupus-flare-activity-from-the-patient-perspective/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/lupus-flare-activity-from-the-patient-perspective/