Session Information
Date: Monday, October 22, 2018
Title: 4M086 ACR Abstract: RA–DX, Manifestations, & Outcomes II: DX & Prognosis I (1858–1863)
Session Type: ACR Concurrent Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose: Patients with RA have an increased risk of cardiovascular disease (CVD) accounting for over 50% of premature deaths in the RA population. EULAR recommends repeat assessment of CVD risk every 5 years or when major changes in DMARD therapies are instituted. Lipid screening should be performed to evaluate and mitigate CVD risk. Our objective was to estimate the 5-year lipid screening rate among Medicare beneficiaries with RA based on the specialties of their treating providers, including rheumatology, primary care providers (PCP) and cardiology.
Methods: We conducted a retrospective cohort study using 2011-2015 Medicare claims data (5% representative sample) that included fee-for-service beneficiaries with RA who were continuously enrolled in Parts A and B for 5 years and had at least 1 outpatient visit during continuous enrollment. Lipid screening including non-fasting total cholesterol and high-density lipoprotein (HDL) was ascertained using CPT codes. We estimated the proportion of beneficiaries receiving at least one lipid screening during the 5 years, using logistic regression, based on the specialties of their treating providers. We stratified the analysis by those with and without preexisting CVD or CVD-risk conditions (e.g., hyperlipidemia, hypertension, and diabetes mellitus).
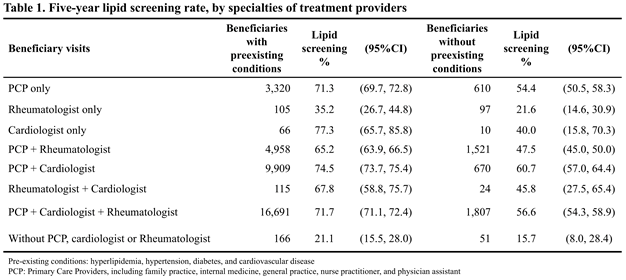
Results: Among 40,120 beneficiaries with RA, 35,330 (88%) had preexisting CVD or CVD-risk conditions. RA patients without preexisting conditions had a 5-year lipid screening rate of 52.8% (95%CI: 51.4, 54.2), while those with preexisting conditions had a screening rate of 71.2% (95%CI: 70.8, 71.7). RA patients without preexisting conditions who only saw a rheumatologist had a lower 5-year lipid screening rate (21.6%, 95%CI: 14.6, 30.9), compared to patients who saw a PCP only (54.4%, 95%CI: 50.5, 58.3) or a cardiologist only (40.0%, 95%CI: 15.8, 70.3). RA patients with preexisting conditions who only saw a rheumatologist had a screening rate of 35.2% (95%CI: 26.7, 44.8), whereas patients who only saw a PCP or cardiologist had screening rates of 71.3% (95%CI: 69.7, 72.8) and 77.3% (95%CI: 65.7, 85.8), respectively. Screening rate estimates for combinations of physician specialties suggest that beneficiaries seen by a PCP and/or a cardiologist have higher rates of lipid screening, with little influence from rheumatology care (Table 1).
Conclusion: Five-year lipid screening rates among Medicare beneficiaries with RA did not meet EULAR recommendations, particularly among those without preexisting CVD or CVD-risk conditions. Patients that were seen by only a rheumatologist had the lowest rate of screening, when compared to patients seen by a PCP or a cardiologist. Rheumatologists need to devise screening implementation strategies to improve comprehensive coordinated CVD preventative care.
To cite this abstract in AMA style:
Kumar N, Lo-Ciganic WH, Zhou L, Ashbeck EL, Kwoh CK. Lipid Screening in Medicare Beneficiaries with Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/lipid-screening-in-medicare-beneficiaries-with-rheumatoid-arthritis/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/lipid-screening-in-medicare-beneficiaries-with-rheumatoid-arthritis/