Session Information
Title: Systemic Sclerosis, Fibrosing Syndromes, and Raynaud’s - Clinical Aspects and Therapeutics II
Session Type: Abstract Submissions (ACR)
Background/Purpose: Recentry, development of potent effective newer drugs for pulmonary arterial hypertension (PAH) have resulted in improving survival of the patients. However, the prognosis of patients with PAH associated with SSc remains still poor compared with that of patients without SSc. To explore the characteristics relevant to the poor survival of patients with PAH associated with SSc, we analyzed serum levels of brain natriuretic peptide (BNP).
Methods: We analyzed 2786 measurements of serum levels of BNP (pg/ml) obtained from 83 patient with PAH associated with CTDs, including 41 patients with SSc, and 42 patients with CTDs other than SSc (16 patients with SLE, 20 patients with MCTD and 6 patients with other CTDs), who had been diagnosed as PAH based on right heart catheterization test and followed between April 2001 and March 2013 in our hospital. For statistical analysis, we converted serum levels of BNP into logarithmic values based on the distribution. Comparison of serum levels of BNP between PAH with SSc and that with non-SSc CTDs was carried out using mixed effects model in which we set presence or absence of SSc, WHO-functional class (WHO-FC) as fixed effects, and patient as a random effect. Comparison of hemodynamics between PAH with SSc and that with non-SSc CTDs was similarly carried out.
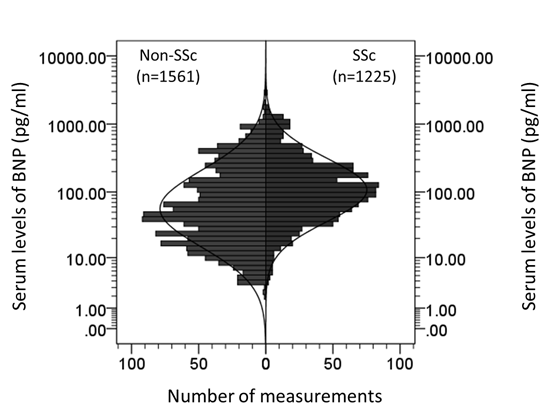
Results: Significant deviation of the distribution of serum levels of BNP was observed between SSc and non-SSc CTDs (Figure). Thus, median (IQR) of serum level of BNP in SSc and non-SSc CTDs were 104.6 (52.5, 214) pg/ml, and 48.9 (19.9, 149.4) pg/ml, respectively. Mixed effects model showed that serum levels of BNP of each WHO-FC in SSc were significantly higher than those in non-SSc CTDs (Table). On right hart catheterization examinations, pulmonary capillary wedge pressure in SSc was significantly higher than that in non-SSc CTDs (8 (5.6, 11.0) mmHg, 6.3(5, 8) [median (IQR)], respectively; p=0.04), although there were no significant differences in mean pulmonary artery pressure, cardiac output, or pulmonary vascular resistance between both group.
Conclusion: Our results demonstrate that left ventricular dysfunction coexists with PAH associated with SSc, accounting for poor survival of PAH associated with SSc. Thus, special attention to this complication would be required in the management of patients with PAH associated with SSc using PAH-specific drugs.
Disclosure:
S. Tanaka,
None;
Y. Arinuma,
None;
T. Wada,
None;
T. Nagai,
None;
J. Okada,
None;
S. Hirohata,
None.
« Back to 2013 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/left-ventricular-dysfunction-reflected-by-higher-serum-brain-natriuretic-peptide-accounts-for-poorer-prognosis-of-pulmonary-arterial-hypertension-associated-with-systemic-sclerosis/