Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Little is known about the incidence of late-onset relapse in systemic vasculitis. This study examined the incidence of relapse < 2 years and ≥ 2 years after diagnosis in 6 different types of systemic vasculitis.
Methods: Data from patients in the Vasculitis Clinical Research Consortium Longitudinal Study, a prospective, multicenter North American cohort, were included if they had no relapse between the date of diagnosis and enrollment into the cohort. 6 vasculitides were studied: granulomatosis with polyangiitis (GPA), eosinophilic granulomatosis with polyangiitis (EGPA), microscopic polyangiitis (MPA), giant cell arteritis (GCA), Takayasu’s arteritis (TAK), and polyarteritis nodosa (PAN). For GPA, EGPA, and MPA, the outcome of relapse was defined as new or worsening Birmingham Vasculitis Activity Score > 0; for GCA, TAK, and PAN, relapse was defined by physician global assessment > 0. Kaplan-Meier curves of the incidence of relapse over time and incidence rates < 2 years and ≥ 2 years from diagnosis were compared within each type of vasculitis. Use of immunosuppressive medications at time of relapse was examined.
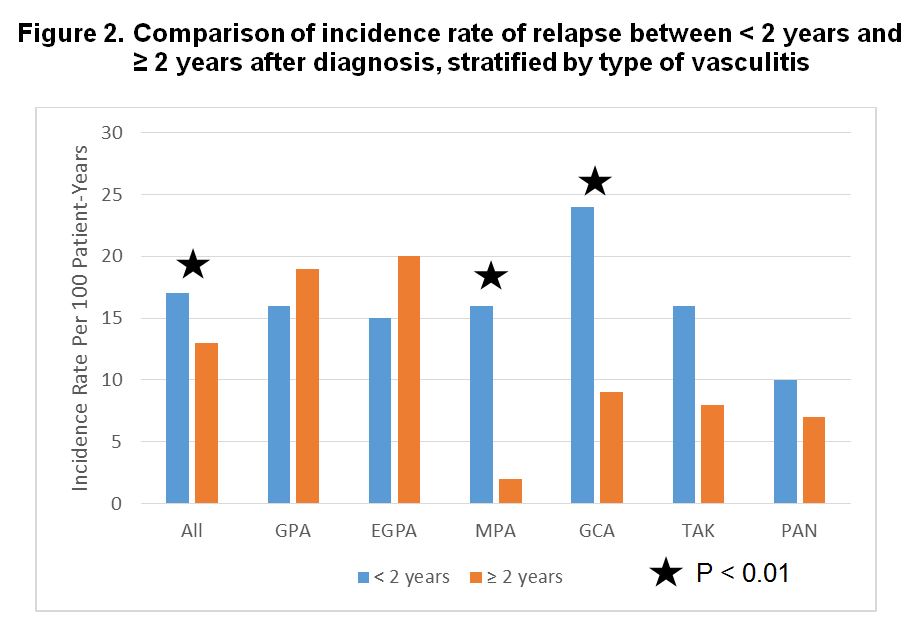
Results: There were 743 patients included in this study: 261 GPA, 95 EGPA, 57 MPA, 212 GCA, 70 TAK, and 48 PAN. The Kaplan-Meier curves for relapse-free survival are shown in Figure 1. A significant decrease in the incidence rate of relapse over time was seen in MPA and GCA but not in the other types of vasculitis (Figure 2). Among those who relapsed, the proportion on non-glucocorticoid immunosuppressive therapy at the time of relapse was not significantly different between the 2 time periods except for PAN. Compared to patients who relapsed within 2 years of their diagnosis, patients with GPA, GCA, and TAK who relapsed after 2 years were less likely to be on prednisone at the time of relapse.
Conclusion: In MPA and GCA, the incidence of relapse significantly decreases after 2 years among those who maintain remission for at least 2 years after diagnosis. However, there are no significant differences in the incidence of relapse after 2 years in GPA, EGPA, TAK, and PAN. Use of maintenance immunosuppressive therapy at time of relapse is not significantly different between those who relapse within or after 2 years, suggesting medications alone cannot account for late-onset relapses. These data indicate that continued close monitoring years after diagnosis is required in patients with systemic vasculitis. 
To cite this abstract in AMA style:
Rhee RL, Dehghan N, Sreih AG, Cuthbertson D, Carette S, Hoffman GS, Khalidi NA, Koening CL, Krischer J, Langford CA, McAlear CA, Monach PA, Moreland LW, Pagnoux C, Seo P, Specks U, Ytterberg SR, Merkel PA. Late-Onset Relapse in Patients with Systemic Vasculitis [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/late-onset-relapse-in-patients-with-systemic-vasculitis/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/late-onset-relapse-in-patients-with-systemic-vasculitis/
