Session Information
Date: Tuesday, October 23, 2018
Title: Osteoporosis and Metabolic Bone Disease – Basic and Clinical Science Poster
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose:
There is controversy about the intervals of retesting bone mineral density (BMD) in patients treated for osteoporosis. The objective of this study is to investigate proper intervals of BMD measurement during treatment of osteoporosis in patients with rheumatoid arthritis (RA).
Methods:
We retrospectively studied 297 patients (271 women and 26 men) with RA who were treated for osteoporosis with mean age of 65.7 ± 8.8 years and the mean duration of treatment for osteoporosis of 8.2 ± 3.9 years. BMD had been measured every year for five years. Annual changes of BMD and T-score at lumbar spine (L1-L4), femoral neck and total hip were evaluated. Treatment failure was defined as an occurrence of two or more fractures, or a reduction in BMD more than the least significant change (LSC) despite adequate treatment. The values of the LSC were 5.3% in lumbar spine, 6.9% in femoral neck, and 5.0% in total hip in the 95% confidence interval.
Results:
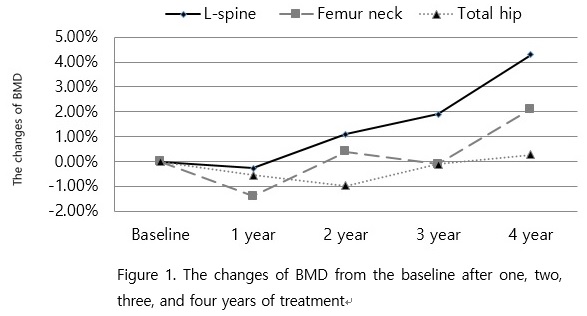
48 (16.2%) patients stopped treatment for osteoporosis due to improvement of T-score. They had an average treatment duration of 4.3 ± 0.5 years before discontinuation. 227 (76.4%) patients were consistently treated with osteoporosis. 18 (6.1%) patients discontinued treatment due to improvement of T-score and then re-started treatment again with deterioration of T-score on follow-up of BMD test. The number of patients with osteoporotic fracture was 80 (30.3%), and among them 57 (19.2%) patients had sustained fractures before starting treatment and 23 (7.7%) patients had incident fractures during treatment for osteoporosis. Annual changes of BMD were -0.28%, 1.24%, 0.84%, and 2.46% at lumbar spine after the first year to the fourth year of treatment compared to the results of previous year respectively, -1.39%, 1.77%, – 0.51%, and 1.78% at femoral neck and -0.56%, -0.49%, 0.97%, and 0.24% at total hip respectively. The changes of BMD from the baseline after one, two, three, and four years of treatment were -0.28%, 1.14%, 1.90%, and 4.31% at lumbar spine, -1.39%, 0.41%, -0.10%, and 2.10% at femoral neck and -0.56%, -0.97%, -0.10%, and 0.28% at total hip respectively (Figure 1). The treatment failure after one year of treatment to the four year compared to the baseline were 11.4%, 7.4%, 5.8% and 3.1% at lumbar spine, 14.7%, 10.1%, 8.4%, and 4.7% at femoral neck and, 13.9%, 12.7%, 9.1%, and 6.3% at total hip respectively.
Conclusion:
Despite treatment for osteoporosis, patients with RA did not show significant improvement of BMD by one year. Considering these results, the reasonable interval of BMD measurement would be at least four years during the anti-osteoporotic treatment because the treatment failure is continuously decreasing. Moreover, many patients with RA need continuous treatment for osteoporosis regardless of BMD due to high incidence of fracture.
To cite this abstract in AMA style:
Lee SY, Kwon SR, Lim MJ, Jung KH, Park W. Intervals of Bone Mineral Density Measurement during Treatment for Osteoporosis in Patients with Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/intervals-of-bone-mineral-density-measurement-during-treatment-for-osteoporosis-in-patients-with-rheumatoid-arthritis/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/intervals-of-bone-mineral-density-measurement-during-treatment-for-osteoporosis-in-patients-with-rheumatoid-arthritis/