Session Information
Session Type: ACR Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Transition from pediatric to adult care is seen as a vulnerable time for youth with chronic diseases. In patients with rheumatic disease, studies show high rates of loss to follow up and increased disease activity in young adults compared to adolescents. However, there are no mortality data on young adults with rheumatic diseases. In this study, we sought to assess whether transitional age is a risk factor for inpatient mortality.
Methods: We analyzed the 2012-2014 National Inpatient Sample database, a representative sample of all discharges in the United States produced by the Agency for Healthcare Research and Quality (AHRQ). Individuals with rheumatic diseases were identified by International Statistical Classification of Disease – 9 (ICD-9) codes at time of discharge. Youth were divided by age into three age groups: pre-transitional age (11-17), transitional age (18-24) and post transitional (25-31). We fitted univariable and multivariable logistic regression models to assess whether transitional age was a risk factor for inpatient mortality. We also assessed whether sex, underlying disease, socioeconomic status, insurance type, and psychiatric comorbidity were risk factors for inpatient death. Due to NIS restrictions on reporting data cells with fewer than 10 outcomes, specific diagnoses were combined to form the following categories: inflammatory arthritis, systemic lupus erythematosus (SLE), systemic sclerosis (SS), connective tissue diseases other than SLE or SS, systemic vasculitis, and periodic fever syndromes.
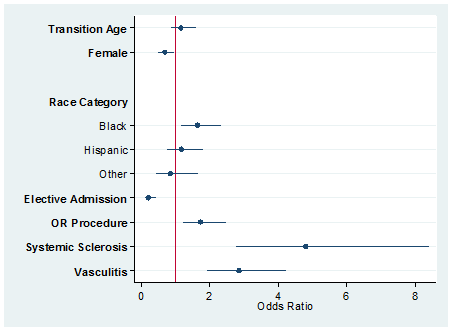
Results: There were 21,488,293 individual hospital discharges in the NIS data sets from 2012-2014. Of these, 30,269 met our inclusion criteria of diagnosis and age. There were 195 inpatient deaths (0.7%). The Odds ratio for inpatient death of an individual in the transitional age range was 1.18 compared to the pre transitional and post-transitional age ranges in the multivariable model (p=0.3). Black race (OR=1.4, p=0.06), male sex (1.75, p<0.001), and a diagnosis of systemic sclerosis (OR= 4.81, p<0.001) or vasculitis (OR= 2.85 p<0.001) were the greatest risk factors of inpatient mortality.
Conclusion: Transitional age was not a risk factor for inpatient mortality in this study. We did identify other risk factors for inpatient mortality other than age. Further studies are required to assess if there is an increased risk of mortality in outpatients of the transitional age group.
Figure 1: Parsimonious multivariable logistic regression model including all covariates significant at the p=0.05 level. Transition age was forced into the model despite being non-significant. White Race was the referent racial category.
To cite this abstract in AMA style:
Jensen PT, Koh K, Cash R, Ardoin SP, Hyder A. Inpatient Mortality in Transition-Aged Youth with Rheumatic Disease: An Analysis of the National Inpatient Sample [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/inpatient-mortality-in-transition-aged-youth-with-rheumatic-disease-an-analysis-of-the-national-inpatient-sample/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/inpatient-mortality-in-transition-aged-youth-with-rheumatic-disease-an-analysis-of-the-national-inpatient-sample/