Session Information
Session Type: Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Osteoporosis is characterized by decreased bone tissue microarchitecture. This leads to reduced bone density and quality and is a significant contributor to morbidity, mortality, and resources. Current guidelines recommend serial BMD measurement with a DXA scan every 1 to 3 years and the latest position paper from International Society for Clinical Densitometry explicitly states the use of the same or cross-calibrated DXA scanners. Interpreting follow-up DXA scan results from different scanners that are not cross-calibrated may lead to erroneous clinical decisions. This retrospective study aims to determine the proportion of patients who had follow-up DXA scans done on different scanners that have not been cross-calibrated and to determine potential risk factors that may contribute to this type of error.
Methods: Service code X128 was used to extract DXA scan records from the Physician Claim Database (PCD) between 1 April 2009 and 31 December 2018, inclusively. Patients at least 18 years of age with at least 2 DXA scans completed during this period were included. Variables for each patient and DXA scan were obtained from the Pharmacy Information Network and PCD using pre-defined pharmaceutical, ICD-9, and ICD-10 codes.
The imaging facility identifier codes of all follow-up scans were compared to that of the immediately preceding scan. A follow-up scan was considered to have a scanner error (SE) if it was performed on different scanner that was not cross-calibrated. Logistic regression model with repeated measurements was used to calculate odds ratios for variables leading to SE.
Results: At least 2 DXA scans were done by 264,866 patients for a total of 470,641 follow-up DXA scans. Of the follow-up DXA scans, 116,401 (25%) were done on a different scanner. With consideration of cross-calibrations done between these different scanners, 88,922 (19%) had a SE. Overall, 97,813 patients (37%) had at least one follow-up DXA scan done at a different facility. With cross-calibration considered, 75,928 (29%) of all patients experienced at least one SE.
Factors associated with SE include increasing time between consecutive DXA scans (OR 1.2502, CI 1.2435-1.2569), rheumatoid arthritis (OR 1.1830, CI 1.1277-1.2410), and fragility fractures (OR 1.0564, CI 1.0339-1.0794). Factors associated with less SE include use of osteoporosis medication (OR 0.8922, CI 0.8753-0.9095), increasing follow-up scan year (OR 0.9762, CI 0.7260-0.9798), and older age at time of last DXA scan (OR 0.9942, CI 0.9933-0.9950). Female sex did not significantly affect SE (OR 0.9725, CI 0.9433-1.0026). The imaging facility groups at which follow-up DXA scans were performed was also associated with differing risk of patients experiencing SE.
Conclusion: Proper management of osteoporosis requires interpretation of comparable DXA scans. This study found that a large proportion of follow-up DXA scans were of minimal clinical utility due to use of different DXA scanners that were not cross-calibrated. Using such results pose significant risk to patients and economic cost to the healthcare system. Interventions are needed to decrease this type of DXA scan error.
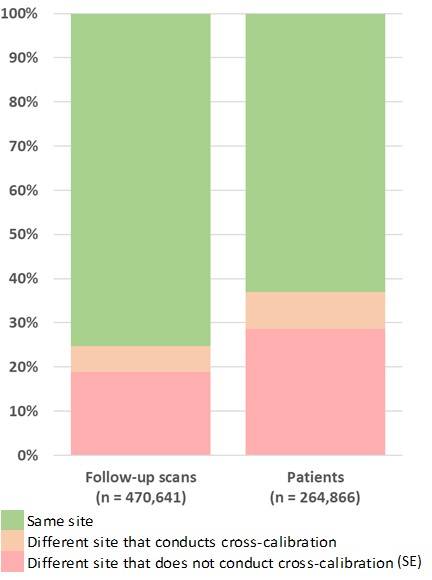 Percentage of follow-up DXA scans and patients
Percentage of follow-up DXA scans and patients
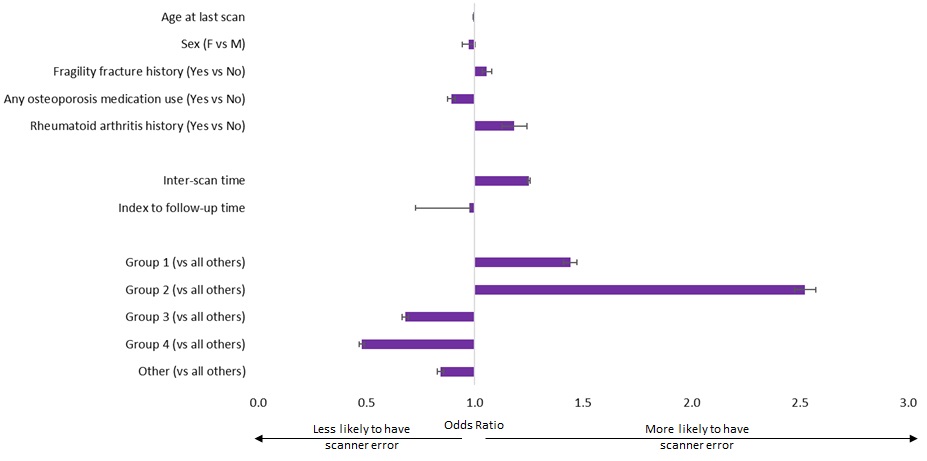 Factors associated with scanner error
Factors associated with scanner error
To cite this abstract in AMA style:
Lee K, Al Jumaily K, Lin M, Siminoski K, Ye C. Incidence of Follow-Up Dual-Energy X-Ray Absorptiometry Scanner Error: A Contributor to Precision Error [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/incidence-of-follow-up-dual-energy-x-ray-absorptiometry-scanner-error-a-contributor-to-precision-error/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/incidence-of-follow-up-dual-energy-x-ray-absorptiometry-scanner-error-a-contributor-to-precision-error/

