Session Information
Date: Sunday, November 10, 2019
Title: 3S076: Patient Outcomes, Preferences, & Attitudes I: Patient Reported Outcomes (833–838)
Session Type: ACR Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose: There is growing interest in the implementation of patient-reported outcome measures (PROMs) in clinical rheumatology to promote patient-centered care and to meet the mandates of value-based health care initiatives. While studies suggest that patients support the routine measurement of patient-reported outcomes in clinical care, the views of rheumatologists are unknown. Understanding rheumatologists’ perspectives on the potential utility and challenges of using PROMs at the point of care is critical to the successful clinical implementation of PROMs. The objective of this study was to investigate rheumatologists’ views on the benefits of and barriers to utilizing PROMs in clinical care, with a specific focus on patients with systemic lupus erythematosus (SLE).
Methods: Structured interviews were conducted with academically affiliated clinical rheumatologists. Interviews were audio-recorded and transcribed verbatim. De-identified transcripts were uploaded into DedooseTM Version 8.2.14 web application for qualitative data analysis. Two authors (SK and AL) reviewed a subset of transcripts to construct a preliminary codebook which was iteratively updated to include emergent themes as additional transcripts were coded. The final codebook was applied using a comparison and consensus approach. Thematic analysis was used to identify the main benefits and barriers of the use of PROMs in clinical care.
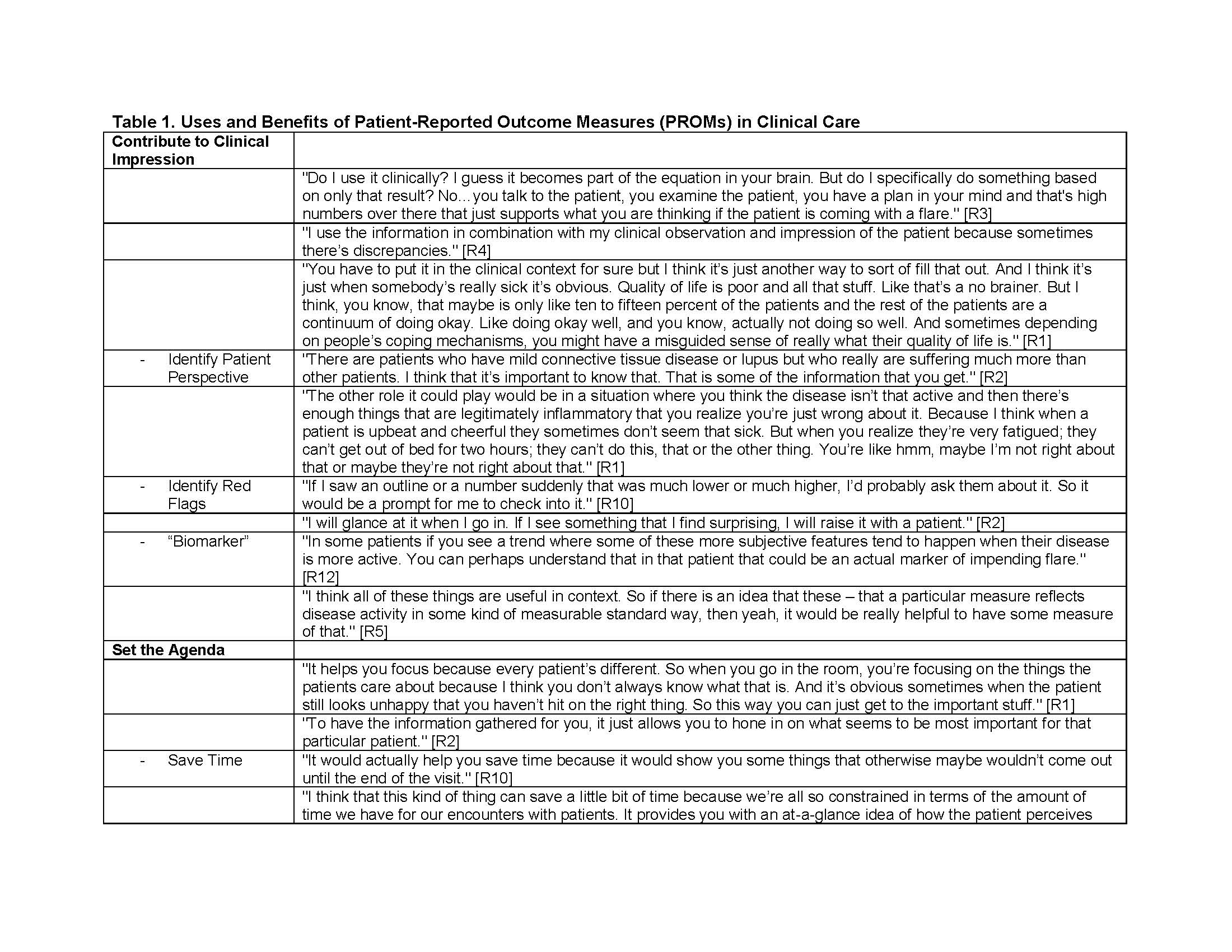
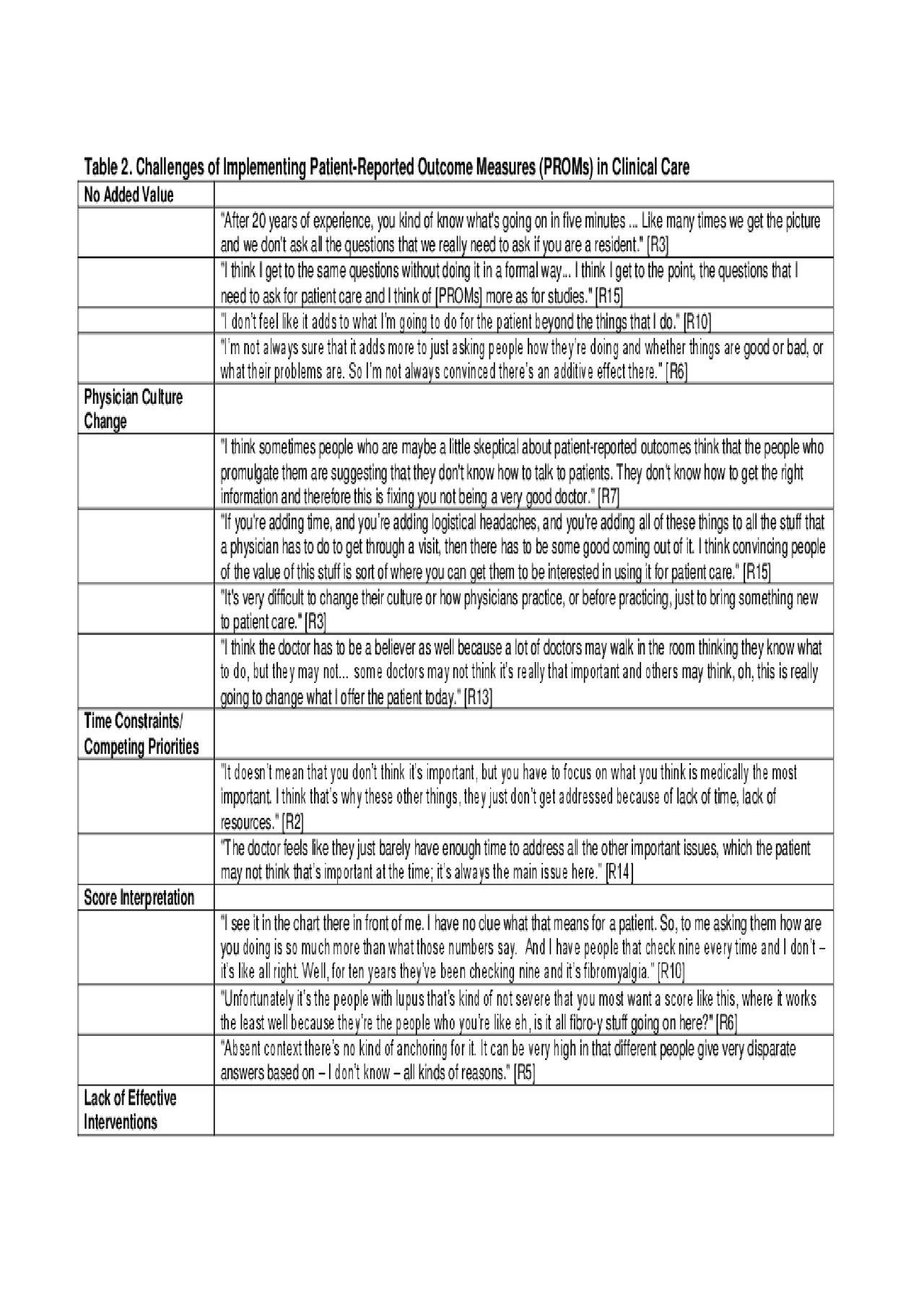
Results: Interviewees consisted of 15 attending rheumatologists affiliated with two academic medical centers in two states, and included 8 women (53%) and 7 men (47%). Subjects reported a median of 15 years in practice (range 5 to 43), with 53% reporting a specific interest in SLE. Rheumatologists identified several uses and benefits of implementing PROMs in clinical care (Table 1), including contributing to the clinical impression by providing the patient perspective, and promoting agenda setting by uncovering “the unspoken questions.” Interviewees noted PROMs could support treatment planning by enabling longitudinal tracking, identifying avenues for intervention, and providing a mechanism for asynchronous care and population management. They noted significant benefits of PROMs in building patient-physician relationships and facilitating patient engagement. However, they also identified several barriers to integrating PROMs in clinical care (Table 2), highlighting physician buy-in and culture change as significant challenges beyond logistical considerations. They further underscored the lack of effective interventions and resources for addressing the domains of most interest to patients.
Conclusion: Rheumatologists identified multiple mechanisms through which PROMs could augment the care of SLE, but also noted several obstacles to implementation in clinical settings, questioning the added value of PROMs and the limited availability of interventions to improve patient-centered outcomes. Programs seeking to successfully integrate PROMs to enhance patient-centered care and meet quality benchmarks must prioritize physician buy-in and training, and provide resources to address the outcomes that are measured.
To cite this abstract in AMA style:
Kasturi S, Wong J, Mandl L, McAlindon T, LeClair A. Implementing Patient-Reported Outcome Measures in Clinical Care: Rheumatologist Perspectives on Opportunities and Challenges [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/implementing-patient-reported-outcome-measures-in-clinical-care-rheumatologist-perspectives-on-opportunities-and-challenges/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/implementing-patient-reported-outcome-measures-in-clinical-care-rheumatologist-perspectives-on-opportunities-and-challenges/