Session Information
The 2020 Pediatric Rheumatology Symposium, originally scheduled for April 29 – May 2, was postponed due to COVID-19; therefore, abstracts were not presented as scheduled.
Date: Friday, May 1, 2020
Title: Poster Session 2
Session Type: ACR Abstract Session
Session Time: 5:00PM-6:00PM
Background/Purpose: Research has established that a large percentage of individuals diagnosed with childhood-onset systemic lupus erythematosus (cSLE) report cognitive dysfunction. Disease factors that can impact cognitive function in cSLE include inflammation, ischemia, and direct antibody effects on grey and white matter. Common cognitive domains affected include attention/executive functioning, memory, visual-spatial skills, language, and psychomotor speed. Identification of neurocognitive deficits by neuropsychological evaluation can help inform treatment recommendations and access to supports. A traditional full-day evaluation may not be practical nor an efficient use of resources for all patients with cSLE, whereas existing computerized screening measures take approximately 35-55 minutes to administer. Neurocognitive screening offers a practical method to quickly assess relevant cognitive domains and identify patients who may benefit from a comprehensive neuropsychological evaluation. The current study sought to explore feasibility of a neurocognitive screening protocol during a multidisciplinary cSLE clinic.
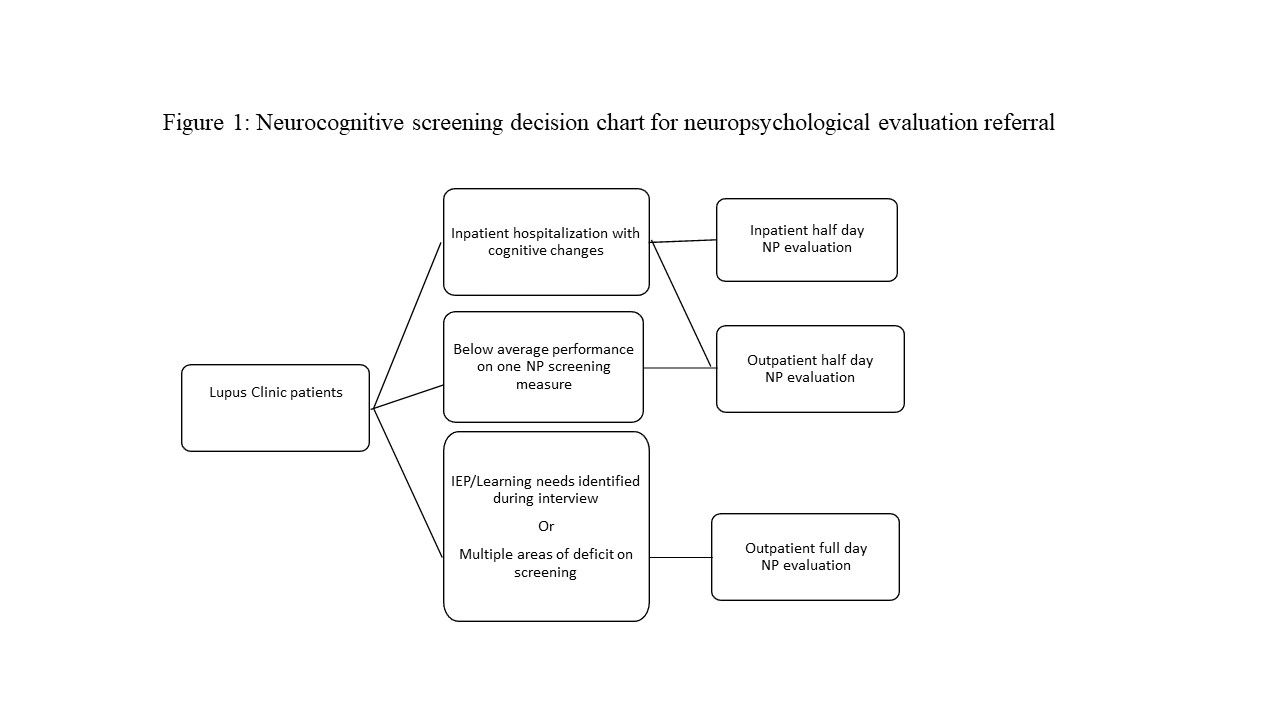
Methods: A brief neurocognitive screening battery was selected based on research findings and priorities of brief duration (10-15 minutes), usability for broad age range (≥8 years), and assessment of typically affected domains. Tools were administered by a neuropsychologist. A decision chart (see Figure 1) outlined the process for referring patients for half-day (3-hour) or full-day (6-hour) neuropsychological evaluation. Neurocognitive screening was routinely completed on consecutive patients in the context of a psychosocial consult visit during a multidisciplinary lupus clinic visit. Scaled and standard scores were transformed to z-scores to allow ease of comparison across subtests.
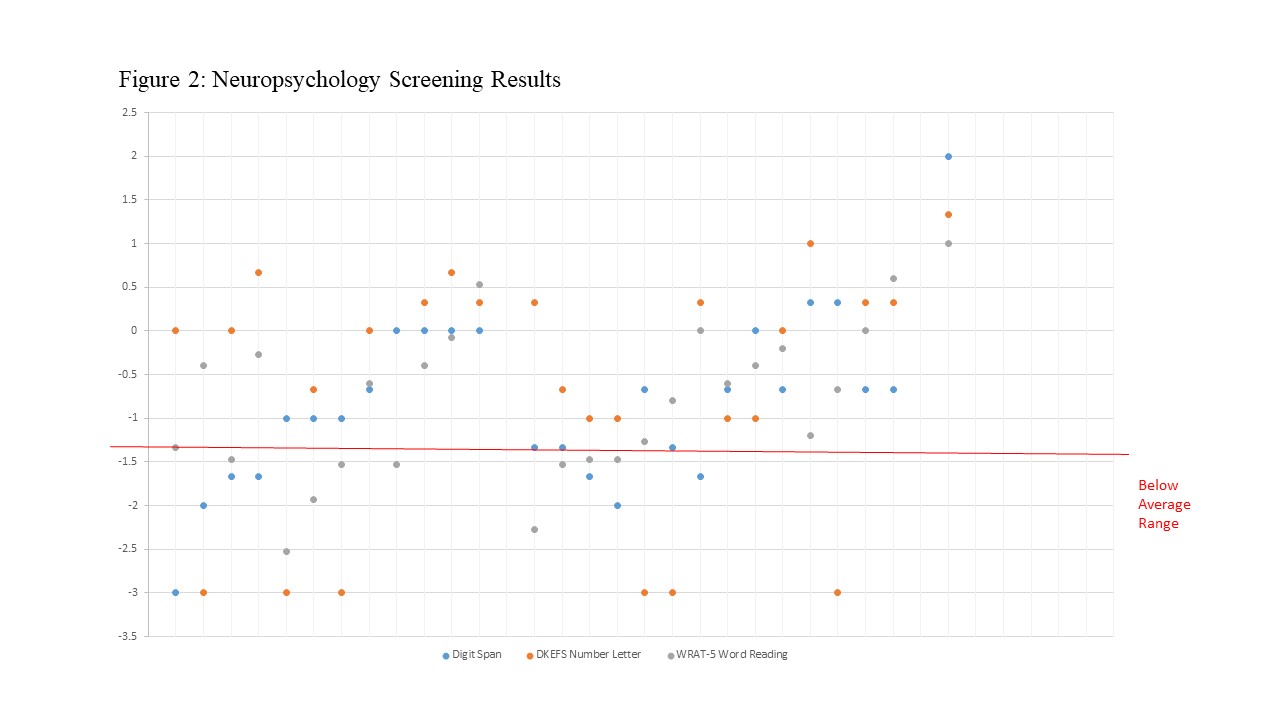
Results: Beginning in September 2018, 27 individuals diagnosed with cSLE (mean age 16.96 years; SD = 3.13) completed neurocognitive screening. Females comprised the majority of the sample (n = 22, 81.5%). The average time of consult visit with neurocognitive screening was 22.04 minutes (SD = 5.61). On screening measures, almost 50% of individuals performed at least one domain in the below average range, while approximately 25% of individuals performed in the below average range for greater than two neurocognitive domains. Eleven individuals (18.5%) were referred for a neuropsychological evaluation. Two families declined referrals as results were felt to be due to other psychosocial factors (for example, anxiety, not feeling well on the day of the screening).
Conclusion: The current study indicates that brief neurocognitive screening is feasible within a multidisciplinary lupus clinic. Brief neurocognitive screening may help identify individuals who are at higher risk for cognitive challenges. Results of screening indicate that 25-50% of individuals with cSLE are performing below age expectations and may warrant referral for a comprehensive evaluation. Future examination of other medical and psychosocial factors linked to neurocognitive challenges in c-SLE may help increase the efficiency of neurocognitive screening within this population.
To cite this abstract in AMA style:
Wilson C, Leever A, Cass J, Sivaraman V, Ardoin S. Implementation of an Abbreviated Neuropsychology Screening Protocol for Patients Diagnosed with Childhood-onset Systemic Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 4). https://acrabstracts.org/abstract/implementation-of-an-abbreviated-neuropsychology-screening-protocol-for-patients-diagnosed-with-childhood-onset-systemic-lupus-erythematosus/. Accessed .« Back to 2020 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/implementation-of-an-abbreviated-neuropsychology-screening-protocol-for-patients-diagnosed-with-childhood-onset-systemic-lupus-erythematosus/