Session Information
Date: Sunday, November 10, 2019
Title: Measures Of Healthcare Quality Poster I: Testing, Screening, & Treating
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Research has shown potential retinal toxicity rates from HCQ as high as 7.5%. Research suggests toxicity is dose-related. In 2016, the American Academy of Ophthalmology (AAO) issued weight-based guidelines for HCQ dosing recommending that daily dose not exceed 5 mg/kg. Two years into the guideline’s release, we analyzed our institution’s HCQ prescribing habits and opinions on these guidelines.
Methods: We collected cross-sectional data from all prescribers in rheumatology and dermatology, from all patients with an active hydroxychloroquine prescription in a 20-month period (June 2017 – January 2019). We collected sex and the most current weight. We grouped and compared patients according to weight-based HCQ dose. Concurrently, we constructed and administered a multiple-choice survey to gauge understanding and perceived utility of these guidelines. Survey responses were compared using Fisher’s exact test with an assigned p-value < 0.05.
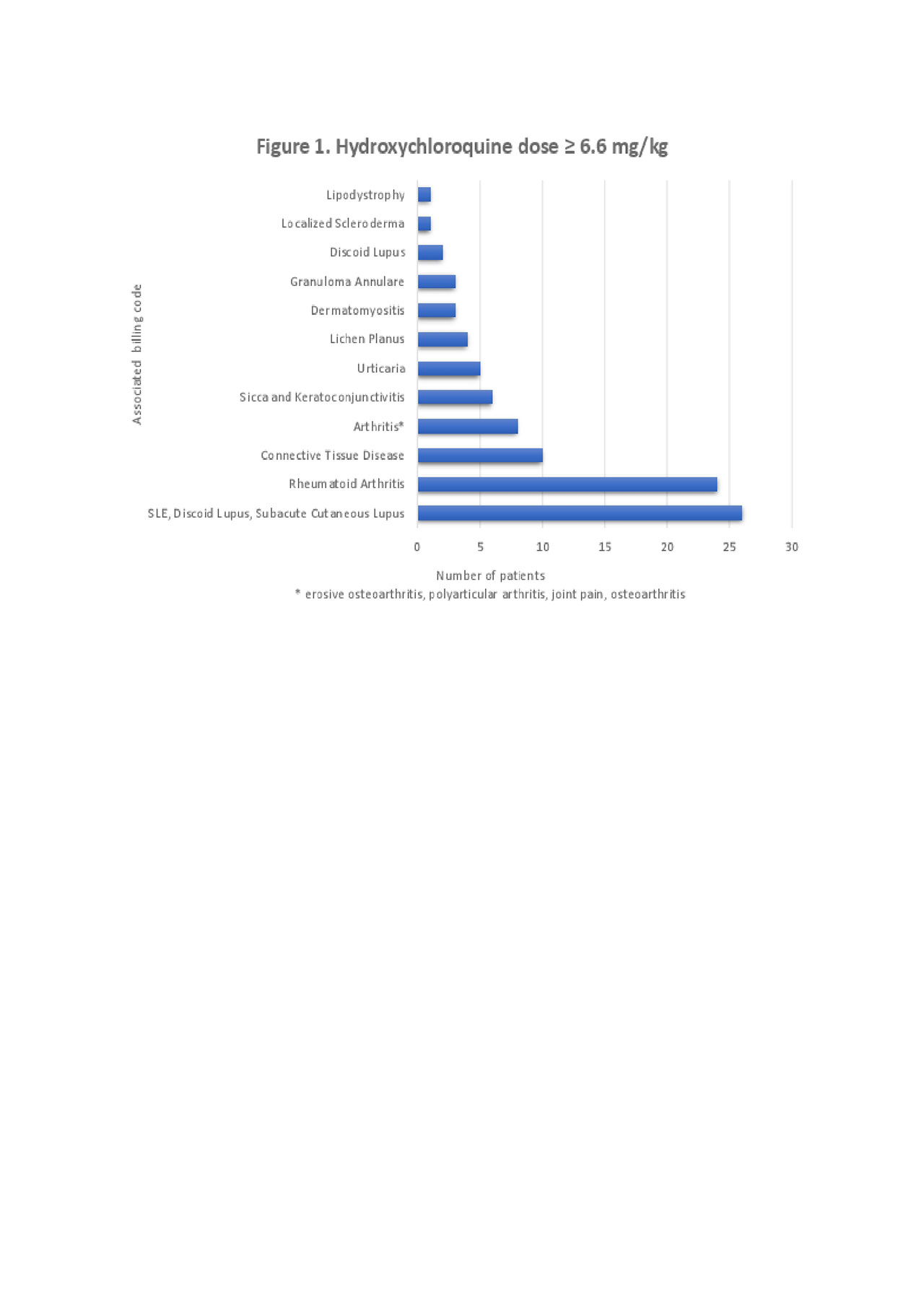
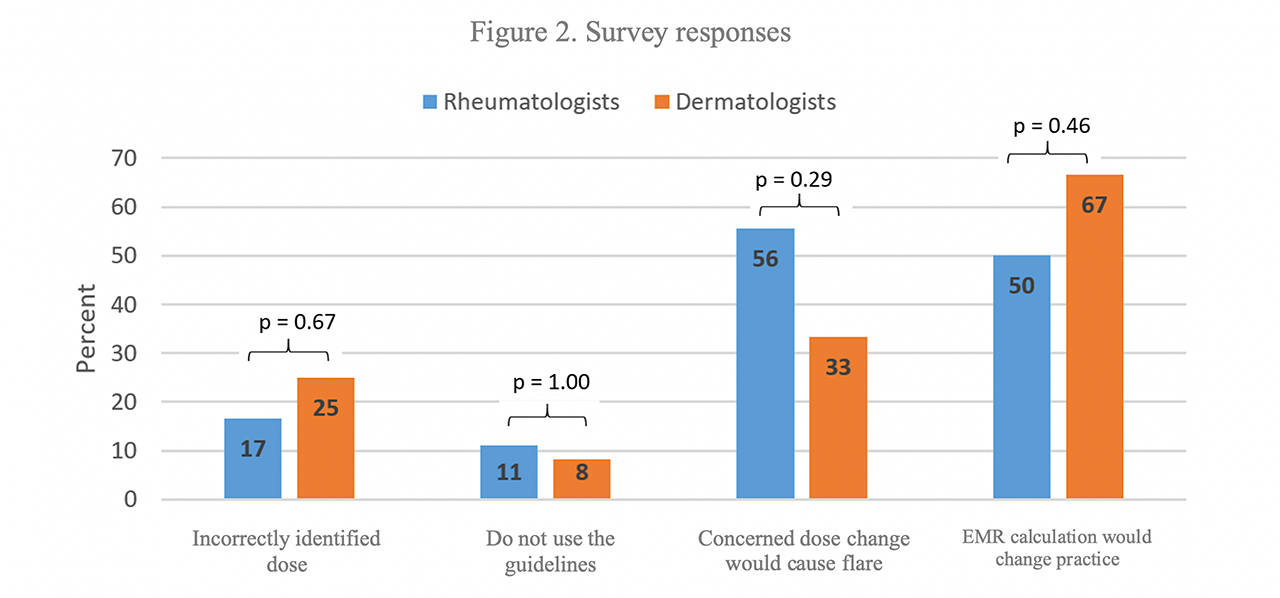
Results: We reviewed 1,128 rheumatology charts. 778 (69%) were prescribed ≤ 5 mg/kg. 80% were female. 277 (25%) were prescribed 5.1 – 6.5 mg/kg. 92% were female. 73 (6%) were prescribed ≥ 6.6 mg/kg. 96% were female. We reviewed 284 dermatology charts. 172 (61%) were prescribed ≤ 5 mg/kg. 71% were female. 77 (27%) were prescribed 5.1 – 6.5 mg/kg. 81% were female. 35 (12%) were prescribed ≥ 6.6 mg/kg. 94% were female (Table 1). In rheumatology patients with HCQ dose ≥ 6.6 mg/kg, use was most often for rheumatoid arthritis and systemic lupus erythematosus (SLE). In dermatology patients, indications for this higher dose included SLE, lichen planus, discoid lupus, dermatomyositis, and urticaria (Figure 1). We compiled 18 surveys from rheumatology and 12 surveys from dermatology. 3 (17%)/3 (25%) incorrectly identified the recommended weight-based dose. 2 (11%)/1 (8%) said they did not use these guidelines in their practice. 10 (56%)/4 (33%) were concerned that changing HCQ dose based on these guidelines would lead to disease flares. 9 (50%)/8 (67%) reported that if their electronic medical record (EMR) automatically calculated a weight-based dose that this would change their practice (Figure 2). There were no statistically significant differences in the survey responses between the subspecialties.
Conclusion: Despite prescribers’ declared familiarity with the 2016 recommendations regarding weight-based dosing of HCQ, and the belief that they are using these guidelines, HCQ doses often exceeded the recommended daily dose (33%). Survey data suggests that this discordance may be due to concern for causing disease flares. This could also suggest a gap between intended practice and actual practice that could be attributed to guideline misunderstanding or lack of knowledge of these guidelines. Findings are similar in rheumatology and dermatology settings. Smaller patients, and presumably therefore women, are more often prescribed a higher and potentially toxic weight-based dose. Further research should be a combined effort of rheumatology, dermatology and ophthalmology to explore tools, including EMR interventions, for bridging this gap between perceived guideline use and “real-world” implementation.
To cite this abstract in AMA style:
Overbury R, Pupaibool J, Hansen C, Clegg D, Lebiedz-Odrobina D. Hydroxychloroquine (HCQ) Prescribing Habits and Provider Opinion on Dosing Guidelines in the Rheumatology and Dermatology Practices of an Academic Institution [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/hydroxychloroquine-hcq-prescribing-habits-and-provider-opinion-on-dosing-guidelines-in-the-rheumatology-and-dermatology-practices-of-an-academic-institution/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/hydroxychloroquine-hcq-prescribing-habits-and-provider-opinion-on-dosing-guidelines-in-the-rheumatology-and-dermatology-practices-of-an-academic-institution/