Session Information
Date: Tuesday, November 7, 2017
Title: Health Services Research I: Cost Drivers in Rheumatic Disease
Session Type: ACR Concurrent Abstract Session
Session Time: 4:30PM-6:00PM
Background/Purpose: Rheumatoid arthritis (RA) is associated with high healthcare resource utilization, but knowledge about factors determining healthcare costs is limited. The aim was to identify healthcare cost drivers in RA.
Methods: RA patients attending Jyvaskyla Central Hospital (JCH) rheumatology unit, Finland, are as of 2007 prospectively enrolled in a structured digital database. We combined this clinical data with well-recorded administrative data on all primary and specialty healthcare in visits in Jyvaskyla area from fiscal year 2014. We excluded 46 outliers, defined as patients with annual costs exceeding the geometric mean by two standard deviations. For each patient, we considered the median of time dependent clinical variables: disease activity score (DAS28-3), health assessment questionnaire index (HAQ index, 0-3), and pain on visual analogue scale (VAS, 0-100). In patients with non-zero costs, factors affecting annual costs (€) were assessed with an age-stratified multivariate generalized linear model using Gamma distribution and a log link function. Variables were selected by statistical significance in univariate analyses. All multivariate analyses were adjusted for age in years or disease duration, and sex. To increase interpretability, we calculated marginal effects at the means of the independent variables. This displays how the annual costs are affected when a variable increases by one unit, while the other variables remain unchanged.
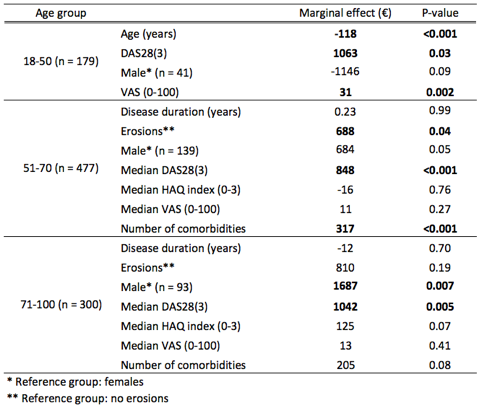
Results: Three age groups were analysed separately: 18-50 (n = 179), 51-70 (n = 477) and 71-100 (n = 300), with mean per-patient annual healthcare costs being 2,942€, 2,914€ and 4,026€, respectively. The main factor associated with healthcare costs across all age groups was disease activity: an increase in the long-term median level of DAS28(3) of an individual yielded up to a 848€ to 1,063€ increase in annual costs (Table 1). In terms of other clinical measures, strong evidence of an association was present for pain in those 18-50 (31€ per one point increase in VAS, p = 0.002) and for number of comorbidities in those 51-70 (317€ per comorbidity, p < 0.001).
Conclusion: A main cost driver in all age groups was disease activity.
Table 1. Multivariate generalized linear model for annual costs, stratified by age. The marginal effects were calculated at the means of the independent variables. For continuous variables, the marginal effect displays how the annual costs are affected when the variable increases by one unit, while the other variables remain unchanged. For dichotomous variables, the change represents comparison to the reference group.
To cite this abstract in AMA style:
Mars N, Kerola AM, Kauppi MJ, Pirinen M, Elonheimo O, Sokka-Isler T. Healthcare Cost Drivers in Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/healthcare-cost-drivers-in-rheumatoid-arthritis/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/healthcare-cost-drivers-in-rheumatoid-arthritis/