Session Information
Session Type: Poster Session (Monday)
Session Time: 9:00AM-11:00AM
Background/Purpose: There have been few large, prospective cohort studies performed on morphea, or localized scleroderma. Most that exist focus exclusively on either pediatric or adult populations, or are retrospective. The objective of this study was to examine two combined prospective databases (Morphea in Adults and Children and National Registry for Childhood-Onset Scleroderma) in order to further characterize these patients and determine subtle features of disease.
Methods: We conducted a cross-sectional analysis using both traditional univariate statistics as well as a multivariate approach – a principal component analysis (PCA). All patients were scored using the Localized Scleroderma Cutaneous Assessment Tool, a validated outcome measure that includes disease activity (modified Localized Scleroderma Skin Severity Index (mLoSSI)) and damage (Localized Scleroderma Skin Damage Index (LoSDI)) components.
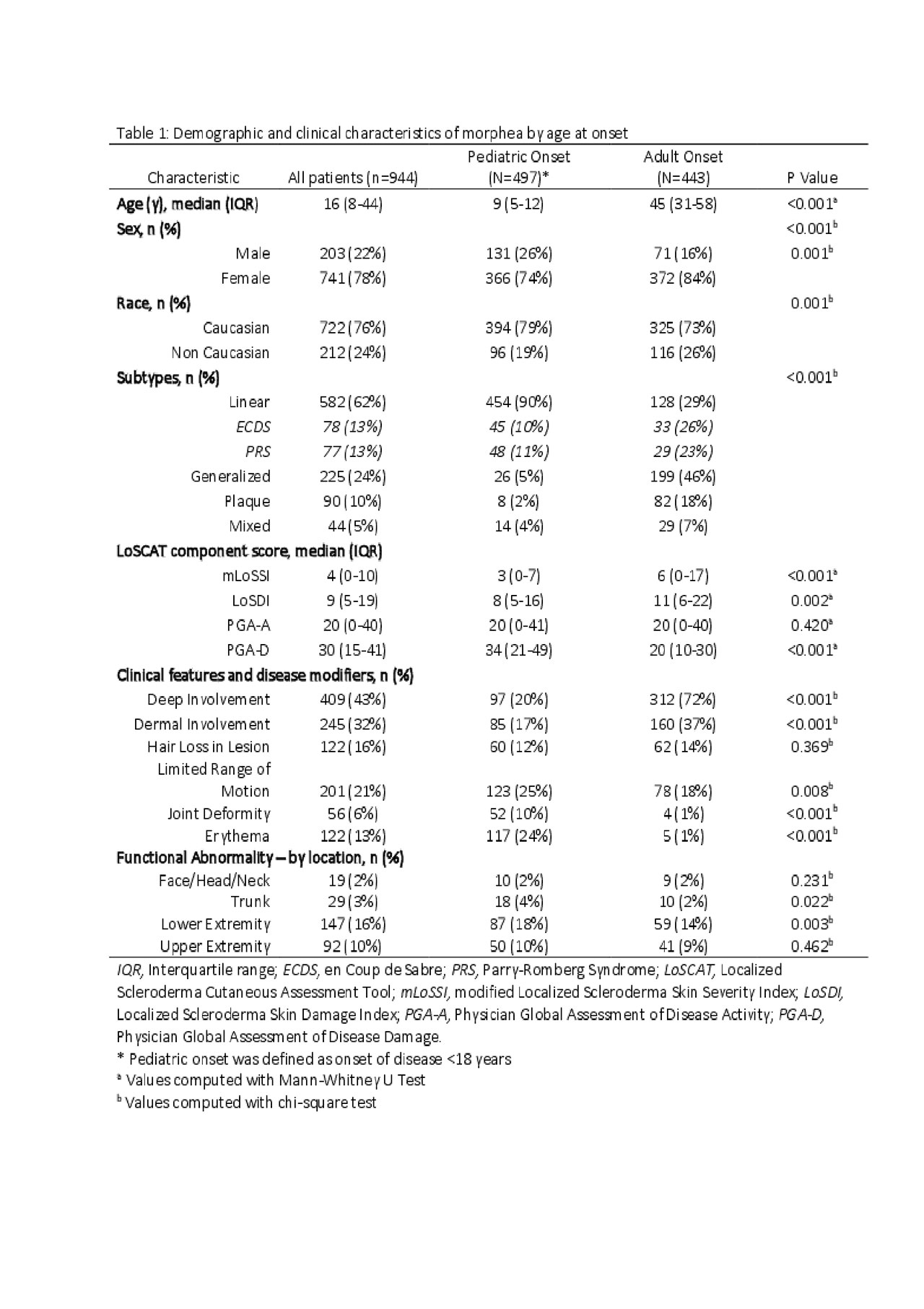
Results: Of the 944 participants, 497 (53%) had pediatric onset morphea, and 433 (47%) had adult onset morphea. [Table 1] Caucasian (76%), female (78%) and linear morphea (62%) patients compromised the majority of the cohort. Adult onset patients had significantly higher mLoSSI and LoSDI scores than pediatric onset disease (p < 0.001 and p = 0.002, respectively), but pediatric onset patients had a significantly higher PGA-D score (p < 0.001). Adult-onset patients were significantly more likely to have deep (72%, 312/443) and dermal (37%, 160/443) involvement (p < 0.001 for both), but children were significantly more likely to have erythema of lesions crossing the joint (24%, 117/497, p < 0.001), limited range of motion (LROM) (25%, 123/497, p = 0.) and joint deformity (10%, 52/497, p < 0.001). Children were also significantly more likely to have functional abnormalities in the trunk (4%, 18/497, p = 0.022) and lower extremity (18%, 87/497, p = 0.003).
Further analysis of the clinical and patient-reported symptoms by PCA determined 4 relevant latent phenotypes (F1-F3). [Table 2] F1 described patients who had LROM in their extremities with high damage scores, while F2 depicted patients with patient reported complaints related to fatigue, pain and depression. F3 described patients with deep dermal and underlying tissue involvement. F4 captures patients with highly active disease.
A PCA of the SKINDEX 30+3 quality of life questionnaire in adults revealed 4 significant factors (F1-F4). [Table 3] F1 represented questions regarding social isolation and overall self-consciousness, while F2 represented patients who exhibited pre-occupation with their skin condition and a higher proportion of emotions questions. F3 characterized patients who had functional impairment and F4 patients with mostly skin related symptoms.
Conclusion: In summary, our large, prospective cross-sectional study demonstrated several novel observations in addition to previously reported findings in morphea. These findings change practice by describing new subsets of morphea patients, including a group with characteristics of chronic pain syndrome and various cohorts with psychosocial impact. These results should be further explored to allow providers to provide more targeted management of these cohorts of morphea patients.
To cite this abstract in AMA style:
Prasad S, Schollaert K, Haley R, Torok K, Jacobe H. Further Characterizing Morphea Subsets Using a Multi-center, Prospective, Cross-sectional Analysis of Morphea in Adults and Children [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/further-characterizing-morphea-subsets-using-a-multi-center-prospective-cross-sectional-analysis-of-morphea-in-adults-and-children/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/further-characterizing-morphea-subsets-using-a-multi-center-prospective-cross-sectional-analysis-of-morphea-in-adults-and-children/