Session Information
Date: Tuesday, November 12, 2019
Title: Miscellanous Rheumatic & Inflammatory Disease Poster III: Autoimmune Conditions and Therapies
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Frailty, a state of decreased homeostatic reserve, is well studied in the elderly and is independently associated with increased morbidity and mortality. Many systemic rheumatic diseases are increased in the elderly and can similarly be associated with poor outcomes. To our knowledge, there are no systematic reviews evaluating frailty in inflammatory rheumatic conditions. Thus, we performed a systematic review to evaluate the prevalence of frailty and the association of frailty with health-related outcomes in patients with systemic rheumatic disease.
Methods: A search of Ovid MEDLINE, Ovid Embase, the Cochrane Library, the Cumulative Index to Nursing and Allied Health Literature, AgeLine, and Scopus was conducted from database inception to January 2019 to identify original research articles and abstracts about frailty and inflammatory rheumatic conditions. Studies addressing frailty, using all definitions, and any inflammatory rheumatic disease were eligible. Data extracted included study design, patient characteristics, frailty instruments, and health-related outcomes. Risk of bias was assessed using the Newcastle-Ottawa scale for cohort and cross-sectional studies and the Cochrane Risk of Bias Tool for randomized controlled trials (RCTs). Two investigators reviewed each study. Disagreements were resolved by a third reviewer. The study was registered prospectively in PROSPERO and conducted according to Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines.
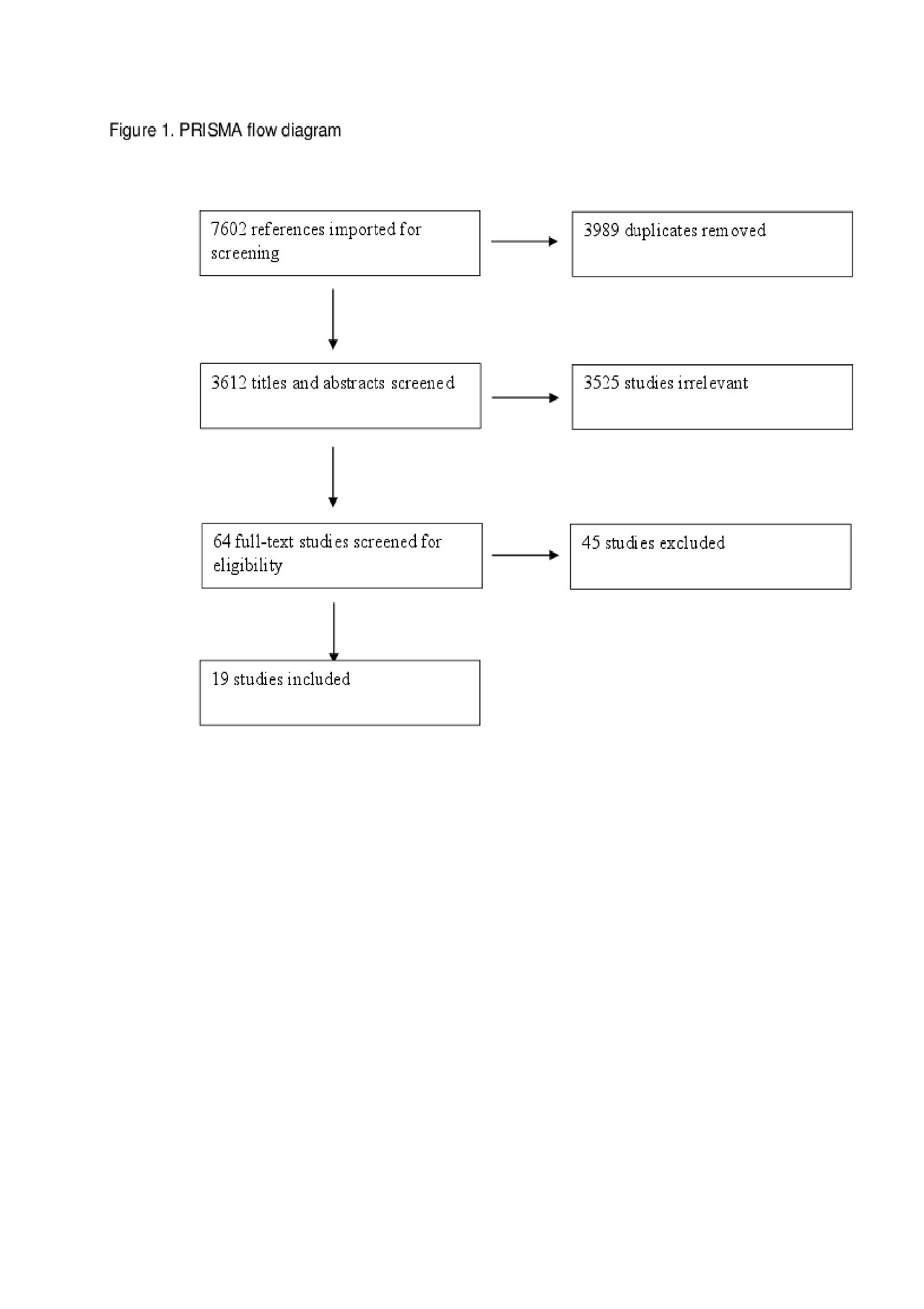
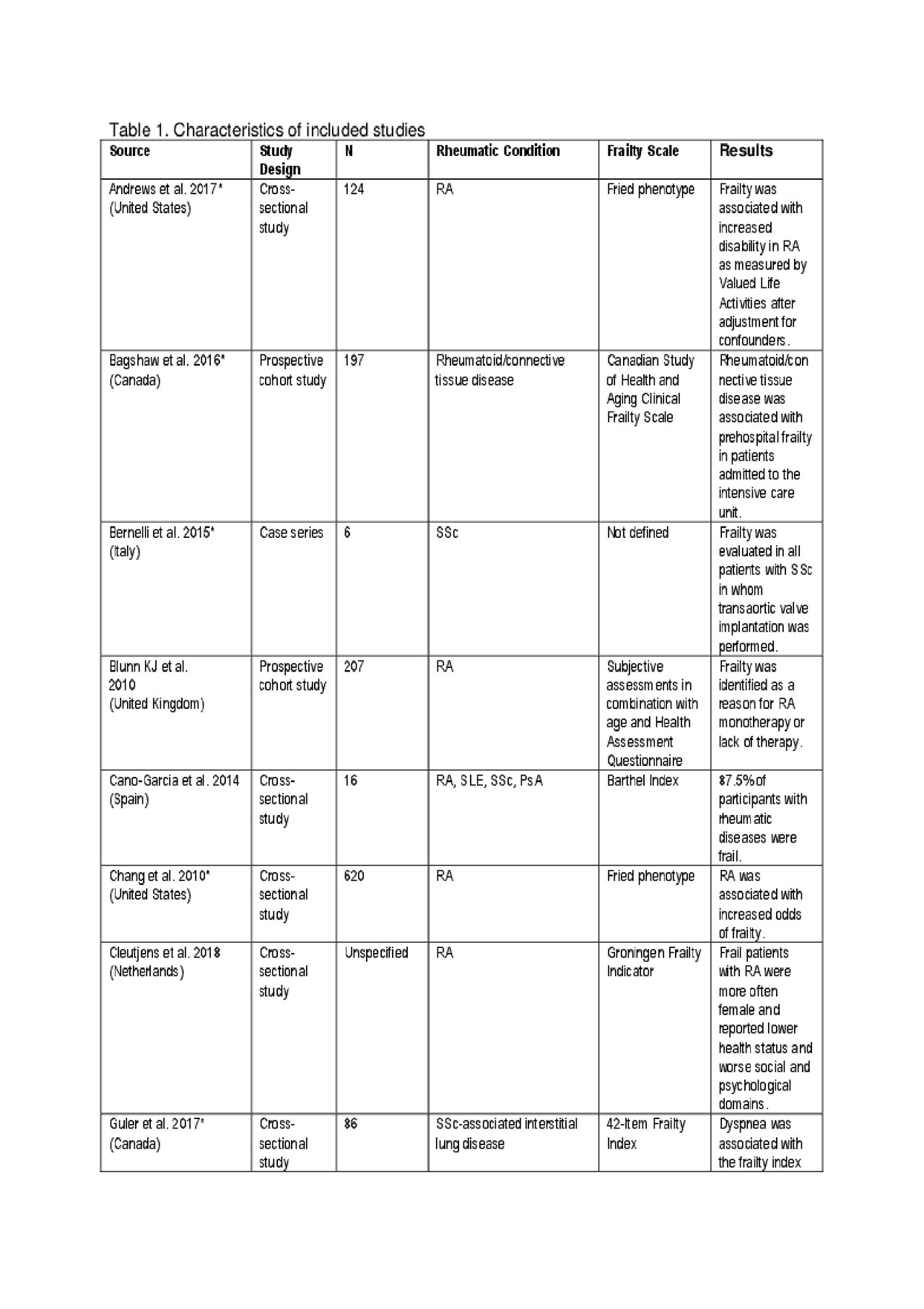
Results: Of 7602 abstracts identified, 64 full-text abstracts and articles were available for review, and 19 were included (Figure 1). These included 1 RCT, 9 prospective cohort studies, 7 cross-sectional studies, 1 retrospective cohort study, and 1 case series. Eleven studies included participants with RA, 4 studies included participants with SSc, 2 studies included participants with SLE, 3 studies included participants with vasculitis, 1 study included participants with PsA, and 2 studies included participants with non-specific “connective tissue disease.” Given study heterogeneity, meta-analysis was not conducted. Risk of bias varied across studies. Frailty was prevalent in multiple systemic rheumatic diseases and associated with poor clinical outcomes, including increased disability and mortality (Table 1).
Conclusion: To our knowledge, this is the first systematic review exploring the relationship between frailty and systemic rheumatic diseases. Frailty is prevalent in multiple systemic rheumatic diseases and is often associated with poor clinical outcomes. Further study is needed to determine risk factors for frailty in systemic rheumatic disease, including risks for progressing from pre-frail to frail. Using standardized frailty instruments will facilitate comparisons between diseases and patient populations.
To cite this abstract in AMA style:
Lieber S, Schmucker A, Mandl L. Frailty in Systemic Rheumatic Diseases: A Systematic Review [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/frailty-in-systemic-rheumatic-diseases-a-systematic-review/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/frailty-in-systemic-rheumatic-diseases-a-systematic-review/