Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Exploring HLA-DRB1 Risk Alleles in Non-Hispanic African American Children with Juvenile Idiopathic Arthritis and Chronic Anterior Uveitis
Background/Purpose:
HLA-DRB1*08, 11 and 13 are risk alleles associated with juvenile idiopathic arthritis (JIA). Carriage of DRB1*11 and *13 may increase the risk for uveitis in Non-Hispanic White children with oligoarticular and polyarticular rheumatoid factor (RF) negative JIA. HLA-B8, in linkage disequilibrium with DRB1*03, was reported in African American children with uveitis. Few studies investigate the role of HLA-DRB1 alleles in Non-Hispanic African American (NH AA) children with JIA or uveitis because they are rare conditions. Our aim is to explore the association of HLA-DRB1 alleles in NH AA children with JIA and chronic anterior uveitis (CAU).
Methods:
High-resolution HLA-DRB1 genotyping was performed to determine the frequency of HLA-DRB1*03, 08,11 and 13 alleles in our cohort of NH AA children with JIA and/or uveitis. Frequencies were compared among JIA and CAU (JIA-associated uveitis and idiopathic chronic anterior uveitis) groups using Chi-square tests and Exact tests. In addition, we compared the frequency of these alleles in our cohorts to 3734 AA healthy controls from the National Marrow Donor Program (NMDP) using two-sided Z-tests for proportions.
Results:
There were 58 NH AA children (43 JIA, 6 JIA-associated uveitis, and 9 idiopathic chronic anterior uveitis) who were mainly female (66%). Of those with JIA, 22 (45%) had extended or persistent oligoarticular JIA, and 27 (55%) had polyarticular RF negative JIA. Antinuclear antibody was positive in 17 (40%) JIA children and 3 (50%) JIA-associated uveitis (JIA-U) children.
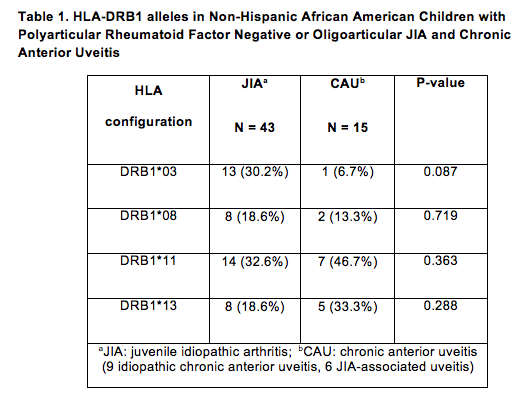
Comparing children with JIA and CAU, there was a borderline significant difference in DRB1*03 (30.2% vs. 6.7%, p = 0.087) (Table 1).
Compared to AA controls, NH AA children with JIA alone had increased DRB1*03 (30.2% vs. 13.6%, p = 0.001), DRB1*08 (18.6% vs. 3.3%), and DRB1*11 (32.6% vs. 13.4%, p < 0.001). NH AA children with CAU (JIA-U and idiopathic chronic anterior uveitis) also had increased DRB1*08 (13.3% vs. 3.3%, p = 0.029) and DRB1*11 (46.7% vs. 13.4%, p < 0.001), which may be associated with the JIA diagnosis (Table 2).
Conclusion:
Carriage of HLA-DRB1*08 and 11 may increase the risk for JIA and uveitis in NH AA children. Carriage of DRB1*03 may also increase the risk for JIA in this cohort. Further studies including larger sample sizes of NH AA children should be conducted to investigate the role of HLA-DRB1 in children with JIA and uveitis.
To cite this abstract in AMA style:
Chan LHK, McCracken C, Jenkins K, Yeh S, Patel P, Prahalad S, Angeles-Han S. Exploring HLA-DRB1 Risk Alleles in Non-Hispanic African American Children with Juvenile Idiopathic Arthritis and Chronic Anterior Uveitis [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/exploring-hla-drb1-risk-alleles-in-non-hispanic-african-american-children-with-juvenile-idiopathic-arthritis-and-chronic-anterior-uveitis/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/exploring-hla-drb1-risk-alleles-in-non-hispanic-african-american-children-with-juvenile-idiopathic-arthritis-and-chronic-anterior-uveitis/