Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose : Some rheumatoid arthritis (RA) patients (pts) may experience flares in their disease even after reaching stable low disease activity (sLDA), but the consequences of even temporary elevations in disease activity are poorly understood. The purpose of this analysis was to explore the rates of flares after reaching sLDA in pts treated to target with either methotrexate (MTX) monotherapy or adalimumab combination therapy (ADA+MTX).
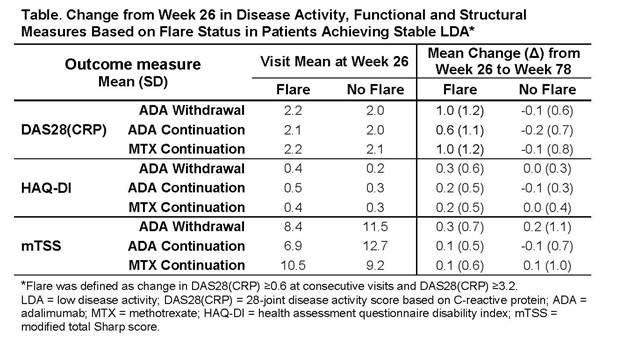
Results : In pts achieving sLDA at the end of P1, flare rates in P2 differed based on initial treatment assignment (ADA Continuation: 11.7% [11/94]; MTX Continuation: 22.4% [22/98]). Interestingly, flare rates in pts randomized to withdraw ADA in P2 (ADA Withdrawal: 25% [22/88]) were numerically similar to the MTX Continuation group. The mean time to flare was 193, 191, and 177 days in the ADA Withdrawal, ADA Continuation, and MTX Continuation groups, respectively. During P2, the mean DAS28(CRP) scores were predictably higher in pts who flared compared with those who did not across treatment groups. In pts experiencing flares in P2, disease activity and functional measures worsened from wk 26 to wk 78 as compared with pts without flares (Table). Of the individual DAS28(CRP) components, pt global assessment of disease activity (PtGA) showed the greatest worsening. There were small differences in radiographic progression between pts experiencing flares compared with pts without flares.
Conclusion : In early RA pts achieving sLDA, flares were generally infrequent; however, they were more prevalent in pts receiving PBO+MTX compared with ADA+MTX. Flares were numerically associated with higher disease activity, functional deterioration, and higher PtGA, underscoring its impact on health-related quality of life and the importance of preventing flares as a therapeutic outcome.
Reference:
1. Smolen JS, et al., Lancet, 2014; 383:321-32.
To cite this abstract in AMA style:
Kavanaugh A, van Vollenhoven RF, Sunkureddi P, Zhang Y, Suboticki JL, Smolen JS. Disease Flares Among Early Rheumatoid Arthritis Patients Treated with Continued Methotrexate Either Alone or in Combination with Adalimumab (Humira) [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/disease-flares-among-early-rheumatoid-arthritis-patients-treated-with-continued-methotrexate-either-alone-or-in-combination-with-adalimumab-humira/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/disease-flares-among-early-rheumatoid-arthritis-patients-treated-with-continued-methotrexate-either-alone-or-in-combination-with-adalimumab-humira/