Session Information
Date: Tuesday, October 23, 2018
Title: Spondyloarthritis Including Psoriatic Arthritis – Clinical Poster III: Treatment
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
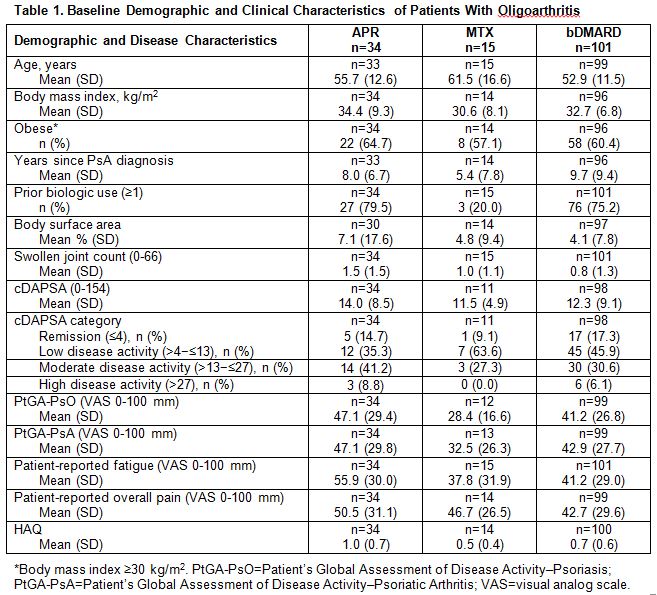
Background/Purpose: The effectiveness of therapies has rarely been studied in the subpopulation of patients with oligoarticular psoriatic arthritis (PsA). The objective of this study was to examine the baseline characteristics and 6-month clinical assessments of patients with PsA who had oligoarthritis (≤4 swollen joints) and initiated treatment with apremilast (APR) or methotrexate (MTX) monotherapy in the Corrona Psoriatic Arthritis/Spondyloarthritis (PsA/SpA) Registry, a prospective, US-based observational cohort study. Patients initiating biologic disease-modifying anti-rheumatic drug (bDMARD) monotherapy were also examined as a point of reference.
Methods: Patients ≥18 years of age with PsA and oligoarthritis in the registry who initiated monotherapy with APR, MTX, or a bDMARD and had a 6-month follow-up visit between June 2014 and March 2018 were included in the analysis. Descriptive statistics were calculated for patients’ clinical characteristics and disease assessments at treatment initiation and at the 6-month follow-up visit.
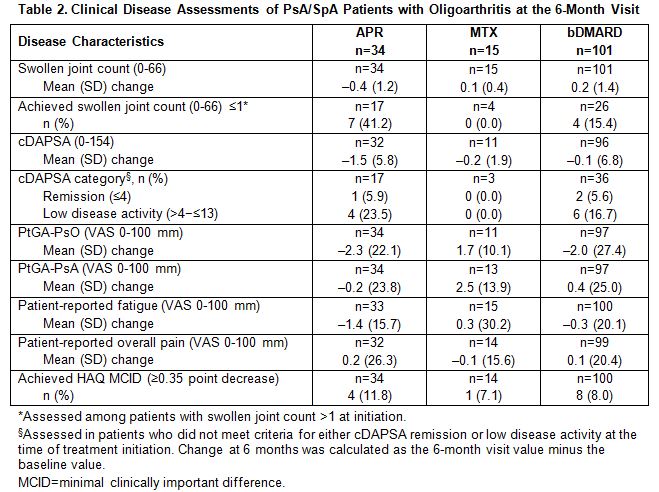
Results: The analysis included 150 patients initiating therapy (APR: n=34; MTX: n=15; bDMARD: n=101). Among APR and MTX initiators, 80% and 20% received at least 1 prior bDMARD, respectively (Table 1). APR was associated with higher levels of disease activity at baseline, including higher swollen joint count, Clinical Disease Activity for Psoriatic Arthritis (cDAPSA) (moderate and high: 50% [APR] vs. 27% [MTX]) and disease impairments represented by numerically higher scores of patient-reported outcome (PRO) measures, including the HAQ. Taken together, results suggest that APR initiators had more refractory oligoarthritis compared with MTX initiators. Clinical assessments at the 6-month follow-up indicate that patients who initiated APR experienced numerically higher improvements in disease activity and various PRO measures compared with MTX, as well as achievement of ≤1 swollen joint, HAQ minimal clinically important difference, and cDAPSA remission or low disease activity (Table 2). Of note, results associated with bDMARDs were more comparable to that of APR.
Conclusion: In this analysis of the Corrona PsA/SpA Registry, APR monotherapy was more often used in patients with refractory oligoarthritis compared with MTX monotherapy. Despite this, the APR group experienced numerically greater improvements in disease activity measures. Improvements observed with APR in patients with long-standing disease and refractory oligoarthritis were modest and comparable to that of bDMARDs.
To cite this abstract in AMA style:
Ogdie A, Liu M, Glynn M, Emeanuru K, Harrold LR, Richter S, Guerette B, Mease PJ. Descriptive Comparisons of the Impact of Apremilast and Methotrexate Monotherapy in Patients with Oligoarticular Psoriatic Arthritis in the Corrona Psoriatic Arthritis/Spondyloarthritis Registry [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/descriptive-comparisons-of-the-impact-of-apremilast-and-methotrexate-monotherapy-in-patients-with-oligoarticular-psoriatic-arthritis-in-the-corrona-psoriatic-arthritis-spondyloarthritis-registry/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/descriptive-comparisons-of-the-impact-of-apremilast-and-methotrexate-monotherapy-in-patients-with-oligoarticular-psoriatic-arthritis-in-the-corrona-psoriatic-arthritis-spondyloarthritis-registry/