Session Information
Date: Sunday, November 5, 2017
Title: Fibromyalgia, Soft Tissue Disorders, Regional and Specific Clinical Pain Syndromes Poster I
Session Type: ACR Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Patients with fibromyalgia may feel depressed. But is it a clinical depression, suggesting the need for SSRI, SNRI, or other medication, or is it frustration related to the presence of the symptoms of the disease?
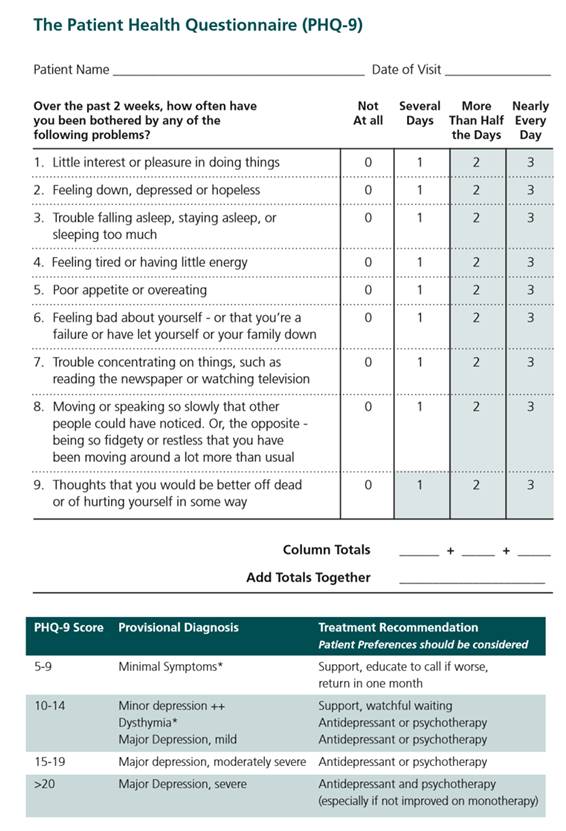
Methods: 115 fibromyalgia syndrome (FMS) patients, meeting the 2010 ACR criteria for the diagnosis, completed a questionnaire in a rheumatology office practice asking whether they were depressed and also whether they felt frustrated. The 62 FMS patients who responded yes to having depression also filled out a Patient Health Questionnaire-9 (PHQ-9) for depression. The PHQ-9 asked the following questions: little interest in doing things; feeling down/depressed; trouble with sleep; feeling tired/low energy; poor appetite; feeling bad about oneself; poor concentration; moving and speaking slowly or excessively fidgety; and thoughts of hurting oneself. Patients were asked to rate these questions based on how they felt over the last two weeks, as follows: 0 for not at all, 1 for several days, 2 for "more than half the days and 3 for nearly every day. A score of 5-9 minimal symptoms, 10-14 minor depression, 15-19 major depression, moderate; and >20 major depression, severe.
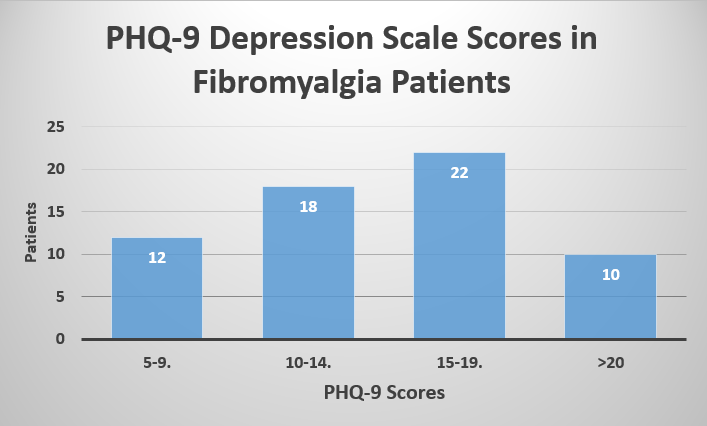
Results: 96 FMS patients responded yes to the question “are you frustrated?” When asked, “Are you depressed?”, 62 FMS patients answered yes. Scores of the PHQ-9 in the 62 FMS patients feeling depressed were as follows: 12 (19.3%) that scored in the 5-9 range (“minimal symptoms”), 18 (29.2%) that scored in the 10-14 range (“minor depression”), 22 (35.4%) that scored in the 15-19 range (Major depression, moderate), and 10 (16.1%) that scored in the >20 range (Major depression, severe).
Conclusion: Of 115 patients with fibromyalgia, 62 reported depression. Using the PHQ-9 depression questionnaire 22 of these patients had a moderate major depression and 10 severe major depression. The great majority of patients with fibromyalgia express frustration but don’t meet the criteria for depression, based on the PHQ-9 questionnaire. Psychotherapy, including ventilation of the patient’s symptoms in the rheumatologist’s office, and continued in a psychologist’s or psychiatrist’s office, can be important. Separating depression, with the possibility of prescribing antidepressant medications, and frustration can be clinically and therapeutically important.
To cite this abstract in AMA style:
Katz RS, Polyak JL. Depression Versus Frustration [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/depression-versus-frustration/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/depression-versus-frustration/