Session Information
Date: Monday, November 11, 2019
Title: RA – Diagnosis, Manifestations, & Outcomes Poster II: Treatments, Outcomes, & Measures
Session Type: Poster Session (Monday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Synovial biopsy is often performed when other methods of evaluation prove non-diagnostic in the assessment of persistent joint synovitis, whether in the setting of undifferentiated inflammatory arthritis (UIA) or rheumatoid arthritis (RA). The utility of synovial biopsy is well established. Several methods are used to perform synovial biopsies, such as arthroscopic surgery, fluoroscopic-guided and blind needle synovial biopsies. In recent years, ultrasound (US) technology has progressed significantly with improved image resolution and increased feasibility of US-guided synovial needle biopsies (USGSB). In this study, we compare histopathological findings of USGSB to surgical synovial biopsies of the same joint in patients with persistent synovitis.
Methods: Between 2016-2019, 25 patients were referred to a single rheumatology practice at an academic medical center for persistent joint synovitis and underwent USGSB. Chart review was performed to identify those patients who had surgical biopsies performed on the same joint. For each patient, tissue samples were sent to pathology in formalin for standard histologic evaluation, methanol for anhydrous histologic evaluation (to allow crystal visualization), and a sterile container for cultures.
Results: Of 25 patients who underwent USGSB, 3 patients also underwent surgical biopsies in the same joint within 12 months of the original biopsy. The age of the patients ranged from 32-81 years old. The main demographic and clinical characteristics of the patients and biopsy sites are presented in Table 1.
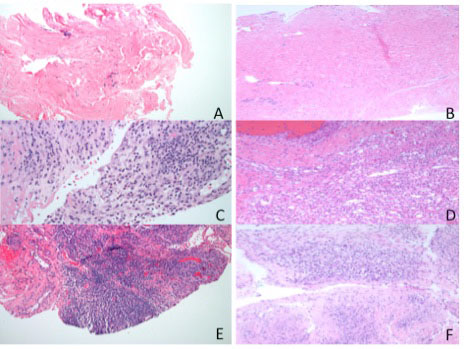
In patient (pt) 1, USGSB of the left 4th proximal interphalangeal (PIP) joint showed benign dense fibrous tissue, compatible with synovium, with similar findings found on a subsequent surgical arthroscopic biopsy, performed for persistent synovitis. Pt 2 was referred for chronic right knee monoarthritis 1 year after surgical arthroscopic synovial biopsy and meniscectomy, which showed hyperplastic synovium with acute and chronic inflammation; USGSB showed similar findings. Pt 3 had RF +, CCP + rheumatoid arthritis, previously failing multiple biologic and non-biologic DMARDs, and then developed persistent left wrist monoarthritis, suspicious for infection. USGSB showed benign synovial tissue and marked chronic lymphoplasmacytic inflammatory changes with scattered acute inflammatory cells compatible with active rheumatoid arthritis. Subsequent therapeutic left wrist surgical synovectomy identified the same pathology as was found with USGSB.
Conclusion: This study demonstrated that USGSB led to similar pathological results as those obtained by more traditional surgical methods. The three patients underwent synovial biopsies of different joint locations including small, medium and large joints. The surgical biopsies did not produce new or additional information beyond that obtained from the USGSB. All patients tolerated the USGSB well without any complications.
When compared to surgical or fluoroscopic guided biopsies, the USGSB technique has advantages including lower cost, no radiation exposure, and local anesthesia. In addition, we found that USGSB had concordant pathologic findings with surgical biopsies.
To cite this abstract in AMA style:
Lim K, Ben-artzi A, Forbess L, Faber S, Ishimori M. Correlation of Ultrasound Guided Synovial Biopsies and Surgical Synovial Biopsies in Patients with Inflammatory Arthritis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/correlation-of-ultrasound-guided-synovial-biopsies-and-surgical-synovial-biopsies-in-patients-with-inflammatory-arthritis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/correlation-of-ultrasound-guided-synovial-biopsies-and-surgical-synovial-biopsies-in-patients-with-inflammatory-arthritis/