Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: The use of swollen (SJC) and tender joint counts (TJC) for rheumatoid arthritis (RA) disease activity and treatment effectiveness is well established. Patient reported outcomes (PRO) are important. However, it is unknown if patient scoring is as reliable as trained professionals.
Methods: PRO including SJC and TJC were assessed at baseline, 6 and 12 weeks by patients and clinicians. Data was collected using ePRO (electronic) and pPRO (paper) The Least Squares Method (LSM), Pearson correlation (Rs.) and weighted Kappa scores were used to assess inter-rater reliability and agreement of responses between the patient, nurse and physician for changes in TJC and SJC from 0 to 12 weeks treatment.
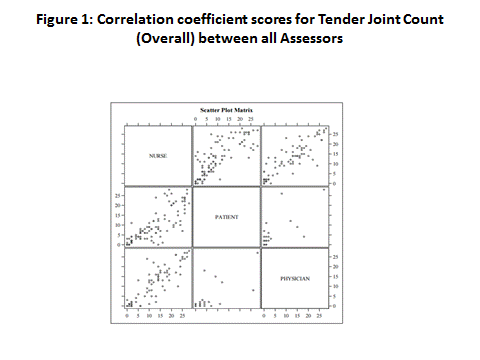
Results: Total 341 evaluable individual assessment episodes comprising 157 Nurse, 106 Patient and 78 Physician joint count episodes in 52 patients with RA of mean duration 11.7 (SD 10.97) years and mean age 55 (SD 14.3, 77% female) enrolled in the study. At baseline, matched joint count episodes were available for 104 Patient – Nurse, 72 Physician – Nurse and 21 Patient – Physician pairs. Correlation of TJC scores per assessor pairs were Rs. 0.83; p<0.001(Patient-Nurse), Rs 0.85; p<0.001(Physician-Nurse) & Rs. 0.59; p=0.005(Physician-Patient) (Table 1). The inter-rater reliability (agreement) of the Patient-Nurse pairs had a weighted Kappa of 0.59 (0.53, 0.68) (Figure 1). Correlation of SJC scores per assessor pairs were Rs. 0.69; p<0.001(Patient-Nurse), Rs 0.66; p<0.001(Physician-Nurse) & Rs. 0.42; p=0.058(Physician-Patient) (Table 1). The inter-rater reliability (agreement) of the Patient-Nurse pairs had a weighted Kappa of 0.48 (0.41, 0.55). The comparison suggests that the biggest discrepancy is from Physician assessments of improvement (interaction between assessor and time).
Conclusion: There is a moderate to high level of agreement between clinicians and patient TJC and SJC assessments that suggest it may be a useful option in assessing joints and response in RA. Further evaluation of activity tools ie DAS28, CDAI or SDAI utilising patient assessments may be worth exploring. Acknowledgements 1. UCB Australia for access to database, assistance with analysis and financial support. 2. Australian Rheumatologists contributing patients to the study. 
To cite this abstract in AMA style:
Inderjeeth C, Inderjeeth A, Raymond W. Concordance Between the Patient, Nurse and Physician Assessment of Clinical Outcomes in a Cohort of Rheumatoid Arthritis Patients Treated with Certolizumab Pegol [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/concordance-between-the-patient-nurse-and-physician-assessment-of-clinical-outcomes-in-a-cohort-of-rheumatoid-arthritis-patients-treated-with-certolizumab-pegol/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/concordance-between-the-patient-nurse-and-physician-assessment-of-clinical-outcomes-in-a-cohort-of-rheumatoid-arthritis-patients-treated-with-certolizumab-pegol/