Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: With the availability of multiple biologic agents, each with different modes of action, use of real world registries provide the manner in which to examine comparative effectiveness in the absence of head-to-head clinical trials inform physicians how they might be used for the treatment of rheumatoid arthritis
Methods: Arthritis Registry Monitoring Database (ARMD) has been collecting prospective patient data since 2005 in all patients seen in routine care. Each patient in this setting (with any diagnosis) completes a 2-sided, 1-page MDHAQ (multidimensional health assessment questionnaire) at every visit while waiting to see the physician in the infrastructure of clinical care. The MDHAQ includes scales for physical function, pain, patient global estimate (PATGL), fatigue, and a self-report RADAI painful joint count. Usage of the biologic medication abatacept as well as its route of administration along with self-reported disease activity and clinic measures were abstracted. Time to first response defined as an improvement in RAPID3 of at least 3.6 was calculated; change from abatacept initiation to first response for self-reported disease activity and clinic measures was estimated by administration route. For those individuals with no response, time to last follow-up was calculated.
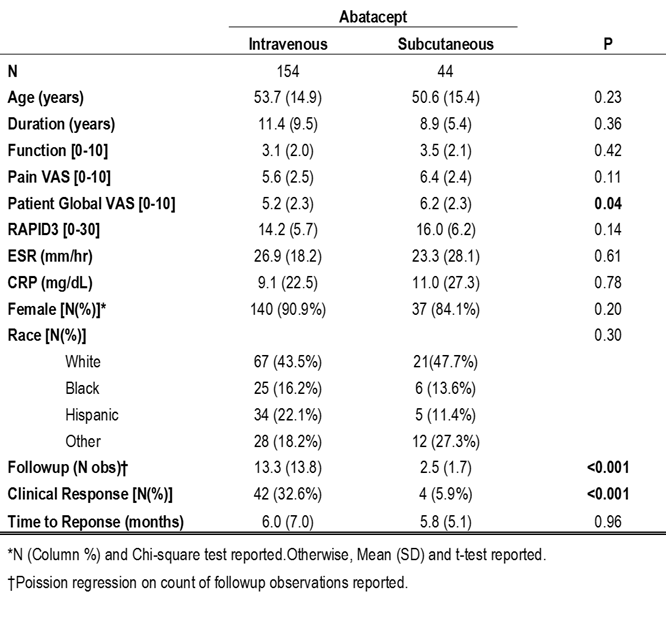
Results: 2168 encounters were reviewed for this analysis. 198 subjects were abstracted with an average of 10.9 followup encounters. The average age of the cohort was 53.0 years (±15.0), average duration 10.9 years (±9.0), 177 (89%) were female, and average baseline RAPID3 was 14.5 (±5.8). 154 subjects were given abatacept intravenously (IV), while 44 were administered abatacept subcutaneously (SC). PATGL was slightly higher in the SC group compared to IV, but the overall RAPID3 was not different; no other differences between demographics or baseline clinical features were observed (Table). However, the SC group had significantly less followup encounters compared to IV (SC 2.5±1.7 versus IV 13.3±13.8, poisson regression P<0.001). Despite the followup disparity, the average time for abatacept subjects to achieve clinical response was approximately six months regardless of administration route (SC 5.8±5.05 versus IV 6.0±7.0).
Conclusion: Our data suggest that there are no major differences in efficacy of the different administration routes of abatacept in time to response when treating RA patients. Further investigation into previous treatment history to determine refractory status and its impact on abatacept efficacy in warranted. Table. Demographic and Clinical Features at Abatacept Initiation as well as Followup Outcomes by Route of Administration
To cite this abstract in AMA style:
Swearingen CJ, Poon J, Bernstein H, Yazici Y. Comparison of Intravenous Versus Subcutaneous Abatacept for the Treatment of Rheumatoid Arthritis in a Routine Clinical Care Setting: A Preliminary, Time to Response Analysis [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/comparison-of-intravenous-versus-subcutaneous-abatacept-for-the-treatment-of-rheumatoid-arthritis-in-a-routine-clinical-care-setting-a-preliminary-time-to-response-analysis/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/comparison-of-intravenous-versus-subcutaneous-abatacept-for-the-treatment-of-rheumatoid-arthritis-in-a-routine-clinical-care-setting-a-preliminary-time-to-response-analysis/