Session Information
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: The predominance of myeloperoxidase-antineutrophil cytoplasmic antibody (ANCA) and interstitial lung disease (ILD) have been reported as characteristics of Japanese patients with ANCA-associated vasculitis (AAV) recently. A previous report using cluster analysis showed that the importance of ANCA type and renal involvement in Western countries. Because of the considerable differences in demographic and clinical characteristics, other relevant clusters may be identified in Japanese patients.
Methods: Using the dataset of two nationwide cohort studies for AAV, we performed multiple correspondence and cluster analysis. Model 1 included ANCA type, items of Birmingham Vasculitis Activity Score (BVAS), and ILD, and Model 2 included serum creatinine and C-reactive protein (CRP) levels additionally. Clustering was performed for finding homogeneous clusters, and clinical characteristics and clinical outcomes were compared among determined clusters. Multivariable regression analysis was conducted to explore factors related to CRP levels among BVAS items and ILD.
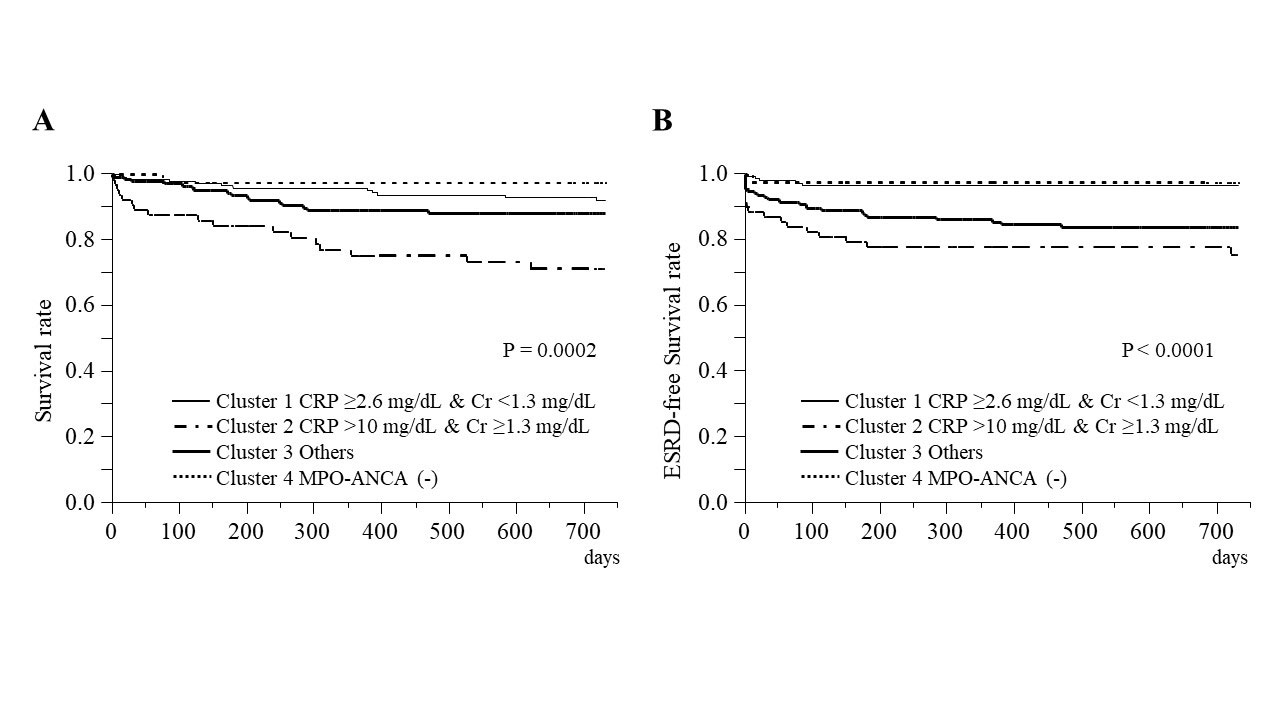
Results: After excluding patients with eosinophilic granulomatosis with polyangiitis or missing of proteinase 3 (PR3)-ANCA test, 427 patients were enrolled. Seven and four clusters were determined in Model 1 and Model 2, respectively. In seven clusters of Model 1, ANCA negative (n=8) and PR3-ANCA positive (n=41) group emerged as distinct two clusters. Other myeloperoxidase-ANCA positive five clusters were characterized by ear, nose and throat (n=47), cutaneous (n=36), renal symptoms (n=256), the absence of renal symptoms (n=33), and others (n=6). Four clusters of Model 2 were characterized either by MPO-ANCA negativity (n=42, cluster 4), high CRP ( >10mg/dL) and increase of creatinine (creatinine ≥1.3 mg/dL) levels (n=71, cluster 2), increase of CRP (≥2.6 mg/dL) without increase of creatinine (< 1.3 mg/dL) levels (n=157, cluster 1), and others (n=157, cluster 3). Overall survival, renal survival, and relapse rates were significantly different across the four clusters of Model 2 (log-rank test; P=0.0002, P< 0.0001 and P=0.0051, respectively, Figure). Multivariable regression analysis revealed that fever (β coefficient [95% confidence interval], 2.1 [1.5–2.6]), myalgia (2.5 [2.0–3.1]), massive hemoptysis/alveolar hemorrhage (1.3 [0.43–2.2]) and mononeuritis multiplex (1.2 [0.47–2.0]) were independently associated with CRP level.
Conclusion: Cluster analysis indicated the association of the distinct clinical and laboratory characteristics with outcomes in Japanese patients with AAV. Prognostic values of improvements in CRP and serum creatinine levels by treatments should be evaluated in future research.
-A- Overall survival rates and -B- ESRD-free survival rates.
Analysis performed using a log-rank test.
ESRD, end-stage renal disease; Cr, creatinine; CRP, C-reactive protein; MPO-ANCA, myeloperoxidase-antineutrophil cytoplasmic antibody.
To cite this abstract in AMA style:
Watanabe H, Sada K, Harigai M, Makino H. Cluster Analysis for Classification of Japanese Antineutrophil Cytoplasmic Antibody-associated Vasculitis: Subgroup Analysis of Nationwide Cohort Studies [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/cluster-analysis-for-classification-of-japanese-antineutrophil-cytoplasmic-antibody-associated-vasculitis-subgroup-analysis-of-nationwide-cohort-studies/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/cluster-analysis-for-classification-of-japanese-antineutrophil-cytoplasmic-antibody-associated-vasculitis-subgroup-analysis-of-nationwide-cohort-studies/