Session Information
Date: Sunday, November 8, 2020
Title: SLE – Diagnosis, Manifestations, & Outcomes Poster II: Comorbidities
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Data about incidence, clinical characteristics and outcome of patients with Systemic Lupus Erythematosus (SLE) with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) disease is scarce. We aimed to describe the infection rate, clinical characteristics and course of COVID-19 in patients with SLE.
Methods: An observational and descriptive study was conducted, which included patients with SLE from our Rheumatology Department. Clinical data and diagnosis of suspected or confirmed COVID-19 infection were extracted from electronic health records. We registered information about the clinical course of COVID-19 and performed a survey about the impact of the pandemic on the behavior and treatment of our patients.
Results: We included 251 patients with SLE, meeting the SLICC or 2019 ACR/EULAR criteria. 93,2% were women, with a mean age of 48,59 ± 13,25 years. 33 patients (13,1%) were diagnosed with suspected or confirmed COVID-19. Eight patients were confirmed by positive RT-PCR assay in nasopharyngeal swabs or by positive serology tests, while 25 patients were considered suspected cases with compatible clinical findings according to the general practitioner but without microbiological confirmation. The most frequent COVID-19 symptoms were cough (78,8%), fever (51,5%) and diarrhea (36,4%). 3 patients had contact with other SARS-CoV-2 positive individuals. Six patients (18,2%) had high disease activity according to SLEDAI-2K prior to the pandemic. 18,2% had secondary antiphospholipid syndrome. Five subjects (15,2%) attended the emergency department and all of them required hospital admission. One patient was admitted to the intensive care unit. Nine patients (39,4%) received specific treatment for COVID-19. The most frequent antiviral drugs were hydroxychloroquine (24,2%) and azithromycin (21,2%). Three individuals received corticosteroids (9,1%) and one received anti-IL6 (3%). Two patients (6,1%) died due to COVID-19, who were receiving rituximab and mycophenolate mofetil, respectively. We compared the characteristics of SLE patients with and without COVID-19 as shown in the table. The survey was responded by 27 patients. During the current COVID-19 pandemic, 63% lived with their families with a median of 3 people (IQR 2-4), while 18,5% lived alone. 74,1% did complete lockdown and 18,5% occasionally left home interacting with other people. 55,5% had telematic follow-up by our Rheumatology department. Regarding rheumatological therapy, 74,1% maintained their usual treatment, 7,4% discontinued biological therapy and 3,7% completely interrupted their current treatment. 63% defined their rheumatic disease as stable whereas 37% experienced more flares during the period under review.
Conclusion: Despite the limited number of patients in our series, there does not appear to be an increased frequency of SARS-CoV-2 in SLE patients. A higher proportion of patients with biological treatment and a history of asthma was found among those who presented suspicious symptoms of COVID-19. This pandemic has had a major impact on the behavior and treatment of our patients; therefore, we emphasize the importance of encouraging patients to maintain current treatment and reinforce preventive measures.
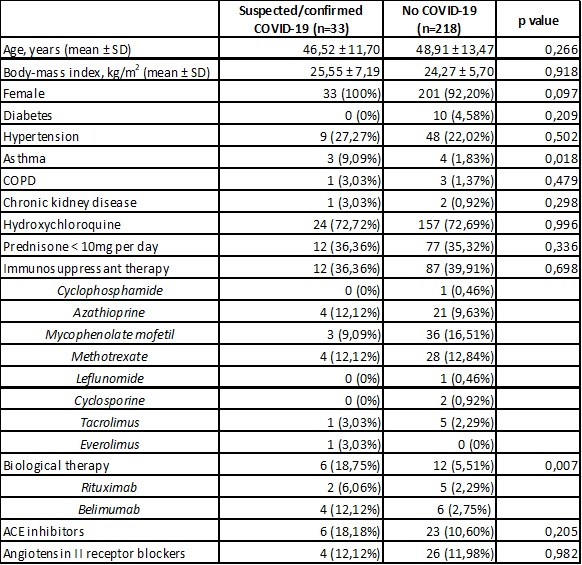 Baseline and clinical characteristics of SLE patients with and without COVID-19.
Baseline and clinical characteristics of SLE patients with and without COVID-19.
To cite this abstract in AMA style:
Briones-Figueroa A, García-Villanueva M, Andreu Suárez �, Tortosa-Cabañas M, Corral-Bote A, Garrote-Corral S, Bachiller-Corral J, Vázquez M. Clinical Characteristics and Impact of the COVID-19 Pandemic in Systemic Lupus Erythematosus Patients in a Spanish Tertiary Hospital [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/clinical-characteristics-and-impact-of-the-covid-19-pandemic-in-systemic-lupus-erythematosus-patients-in-a-spanish-tertiary-hospital/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/clinical-characteristics-and-impact-of-the-covid-19-pandemic-in-systemic-lupus-erythematosus-patients-in-a-spanish-tertiary-hospital/
