Session Information
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Inflammatory joint diseases (IJD) such as psoriatic arthritis (PsA) have an increased risk of cardiovascular disease (CVD) since inflammation plays a pivotal role in the pathogenesis of coronary artery disease (CAD), heart failure (HF) and atrial fibrillation (Afib)1. Ischemic heart disease and HF are the main causes of the increased and premature mortality among patients with IJD2.
Additionally, patients with PsA have a prevalence of hyperuricemia (HUC) of 32%, 3 times greater as compared with the general population, which may be related to increased cell turnover as well as the release of pro-inflammatory cytokines and tumor necrosis factor3.
Prolonged exposure to high levels of uric acid (UA) has been shown to result in oxidative stress causing endothelial dysfunction, ionic channel changes, atrial and ventricular remodeling4. There is experimental evidence indicating that uric acid stimulates renin-angiotensin-aldosterone system (RAAS), and it is associated with an increase in cardiac tissue xanthine oxidase activity, all of which induce cardiomyocyte hypertrophy, myocardial oxidative stress, interstitial fibrosis and impaired diastolic relaxation5.
Methods: This is a retrospective cohort study using the 2016 National Inpatient Sample (NIS) of adults diagnosed with PsA based on ICD-10 codes, to detect the prevalence of cardiovascular (CV) conditions such as CAD, Afib, and HF with preserved ejection fraction (HFpEF) in patients with concomitant HUC or gout versus age matched controls. Chi square was used for point prevalence and multivariate linear regression adjustment was used for age, gender, race, CAD, diabetes mellitus, HTN, hyperlipidemia (HLD), smoking, chronic kidney disease (CKD) and Charlson comorbidity index to obtain prevalence odds ratio (POR). We used STATA-15 for statistical analysis.
Results: We identified 37,315 patients with PsA, of whom 2,165 had concomitant HUC or gout (5.80%). Mean age was 61 years, 57% were females. Our results showed that PsA with concomitant HUC or gout compared to PsA without HUC or gout was associated with a higher rate of Afib (17.8% vs 6.1%, p < 0.001), CAD (35.1% vs 19.4%, p < 0.001) and HFpEF (7.2% vs 3.1%, p < 0.001). Furthermore, patients with PsA and HUC/gout appeared to have more risk of developing Afib (POR 1.79; 95%-CI 1.31-2.45; p < 0.001) and HFpEF (POR 1.56; 95%-CI 1.08-2.26; p=0.018), compared to patients with normal uric acid after multivariate-adjustment for risk factors. No statistical difference in CAD was identified between the two groups (POR 1.21; 95%-CI 0.94-1.55; p=0.131) after multivariate linear regression adjustment for confounders.
Conclusion: This study showed that HUC is independently associated with CVD, mainly with Afib and HFpEF in patients with PsA. It remains to be seen if a treat-to-target approach with normalization of UA in patients with PsA will result in improved CV outcomes. We believe that our findings merit further investigation and that this study adds weight to the hypothesis of UA as a potential risk factor for CVD. Prospective studies are needed to establish the role of serum uric acid level as a biomarker or predictor for CVD, including CAD, Afib and HFpEF in patients with PsA.
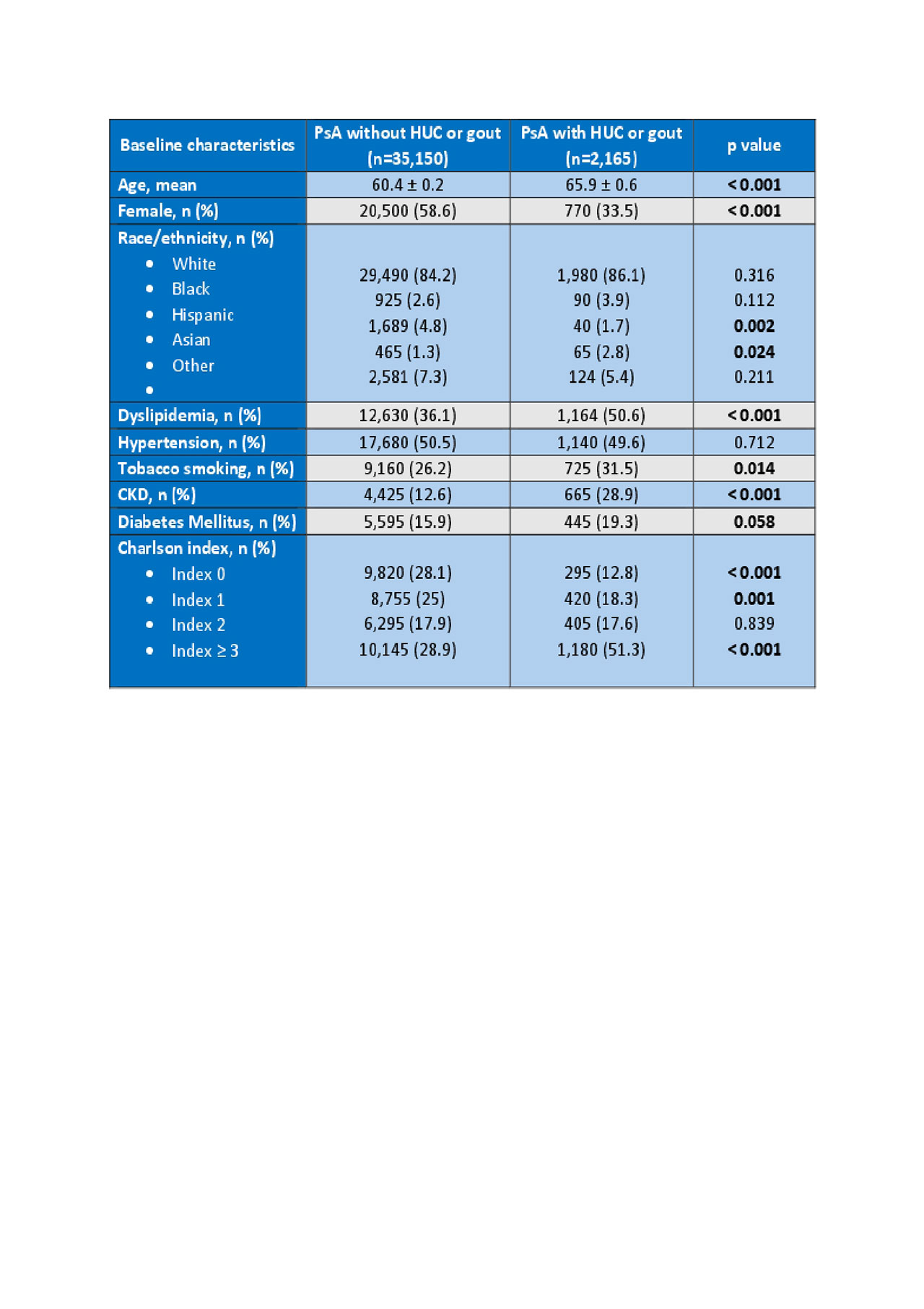
Table 1 Baseline characteristics
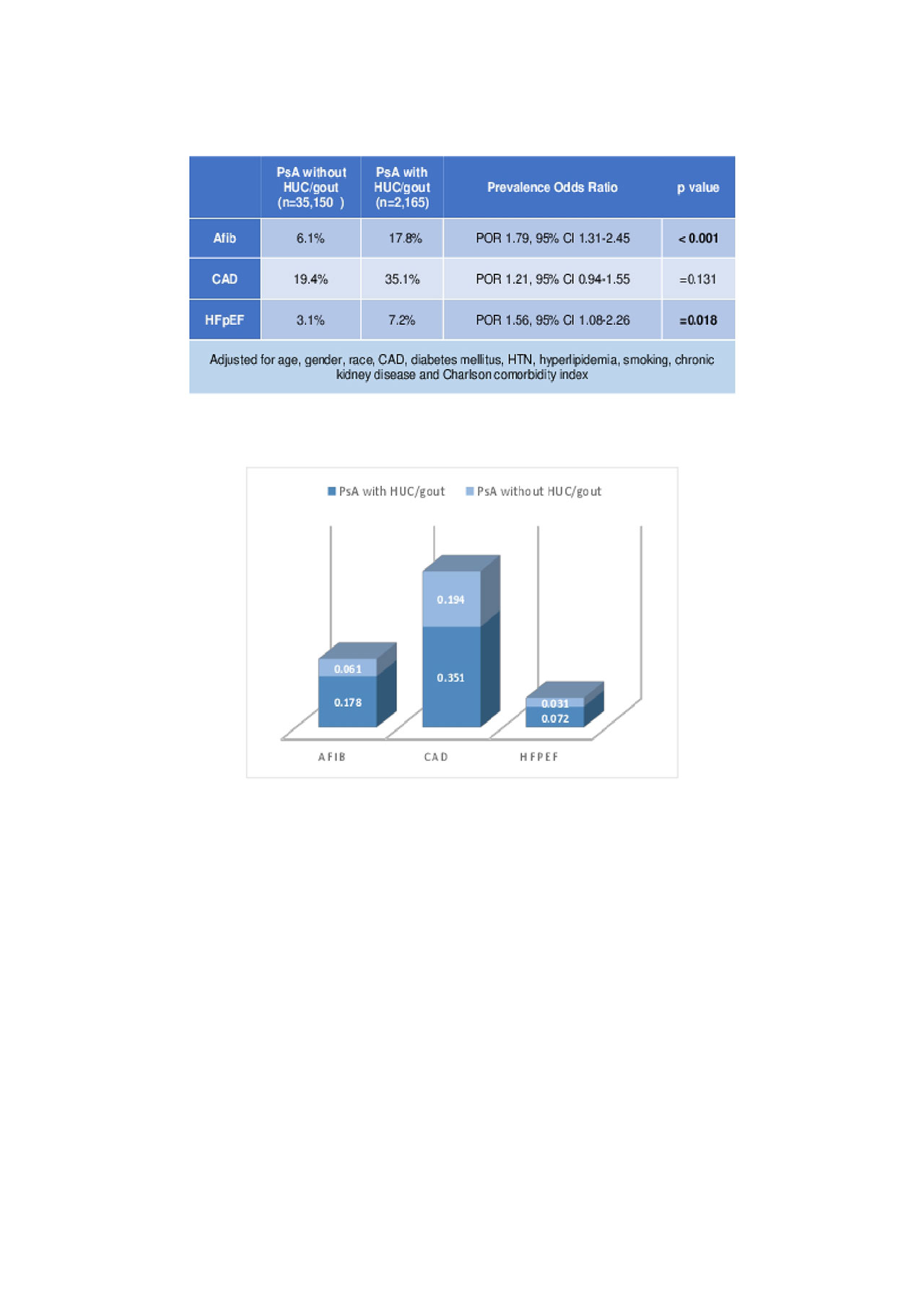
Table 2 Prevalence of Afib, CAD and HFpEF in PsA with and without HUC
To cite this abstract in AMA style:
Arevalo A, Haddadin F, Contreras G, Murray S, Luo Y, Ali Y. Cardiovascular Impact of Hyperuricemia in Patients with Psoriatic Arthritis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/cardiovascular-impact-of-hyperuricemia-in-patients-with-psoriatic-arthritis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/cardiovascular-impact-of-hyperuricemia-in-patients-with-psoriatic-arthritis/
