Session Information
Date: Tuesday, November 12, 2019
Title: Osteoporosis & Metabolic Bone Disease – Basic & Clinical Science Poster
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Bone mineral density (BMD) is used for the diagnosis of osteoporosis, predicting future fracture risk, and monitoring osteoporosis treatment. Osteoporosis is defined as BMD of at least 2.5 standard deviations below the young adult mean (YAM) (T-score ≦2.5) according to World Health Organization (WHO) criteria or a BMD of 70% or lower of YAM (YAM% ≦70) according to the Japanese Society for Bone and Mineral Research (JSBMR) criteria in Japan. As is often the case, T-score or YAM% values of different skeletal sites are discordant. This means that making a diagnosis of osteoporosis may depend on measured sites. BMD of the spine and hip is usually measured for the diagnosis of osteoporosis; however, that of the distal radius is not always measured. The purpose of the present study was to clarify correlations of BMD among the three skeletal sites and evaluate whether measuring BMD of the distal radius is essential. In addition, BMD of the three skeletal sites based on patients’ age was investigated.
Methods: Two hundred and one patients between the ages of 52 and 93 with postmenopausal osteoporosis were enrolled.
BMD of the spine, hip, and distal radius was measured using dual energy X-ray absorptiometry (DXA) (Prodigy, GE Healthcare UK Ltd.). The cut-off values for the diagnosis of osteoporosis according to JSBMR criteria were used. Analyses of correlations between BMD of two skeletal sites (i.e., hip and distal radius, spine and distal radius, and hip and spine) were assessed using the t-test.
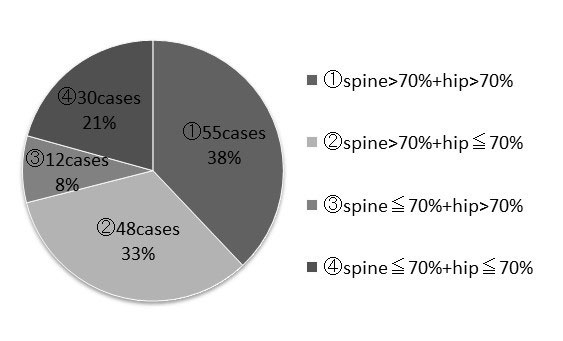
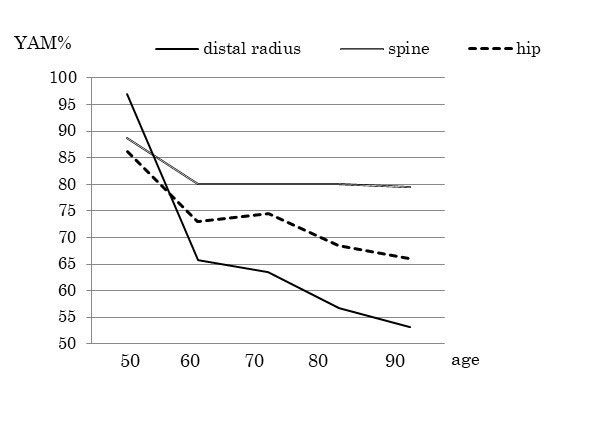
Results: YAM% of the distal radius was 61.7%, being lower than that of the spine, 80.4%, and hip, 71.9% (p >0.001) (Table 1). Correlation coefficients of BMD between the hip and distal radius, spine and distal radius, and hip and spine were 0.475965, 0.406596, and 0.415697, respectively. Among the 145 patients diagnosed as osteoporotic at the distal radius, 55 were not osteoporotic at either the spine or hip, 48 (33%) were osteoporotic at the hip but not spine, 12 (8%) were osteoporotic at the spine but not hip, and 30 (21%) were osteoporotic at both the spine and hip (Table 2). Among the 56 patients without osteoporosis at the distal radius, only one patient (1.8%) was osteoporotic at the spine and 12 (21%) were osteoporotic at the hip. YAM% of the three skeletal sites according to the patients’ age is shown in Table 3.
Conclusion: BMD of the distal radius is significantly lower than those of the spine and hip. Sontag reported that the radius was frequently recognized as the site of initial osteoporotic fractures among women with osteoporosis. This report might support the present study and suggest the possible susceptibility of the radius to osteoporosis as the initial site compared with the spine and hip, especially in early osteoporotic generations. Among 145 patients diagnosed with osteoporosis at the distal radius, 55 (38%) were not osteoporotic at either the spine or hip. This means that a diagnosis of osteoporosis might not be made for some patients if only BMD of the spine and hip and not the distal radius is measured. Therefore, measuring BMD of the distal radius in addition to that of both the spine and hip is highly recommended to avoid underestimating the actual value of BMD for the diagnosis of osteoporosis, especially in early osteoporotic generations.
To cite this abstract in AMA style:
NAKASEKO K. Bone Mineral Density of the Spine, Hip, and Distal Radius in Patients with Postmenopausal Osteoporosis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/bone-mineral-density-of-the-spine-hip-and-distal-radius-in-patients-with-postmenopausal-osteoporosis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/bone-mineral-density-of-the-spine-hip-and-distal-radius-in-patients-with-postmenopausal-osteoporosis/