Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose:
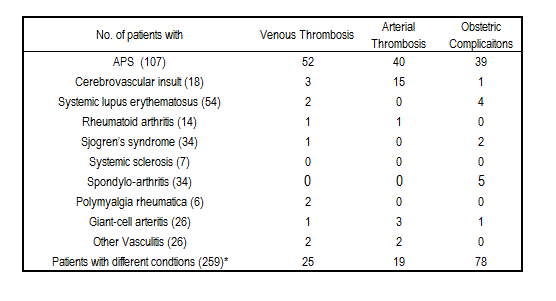
Patients with autoimmune disorders are at risk for thrombotic events and antiphospholipid antibodies (aPL) are one of known markers of increased thrombotic risk. The aims of our cross-sectional retrospective study were a) to evaluate association of different risk factors with thrombosis and b) to calculate the risk score of individual patients for experiencing thrombosis on a large cohort of unselected patients with autoimmune diseases, treated at our secondary/tertiary medical center.Methods: Lupus anticoagulant (LA)1, IgG, IgM, and IgA isotypes of anti-cardiolipin antibodies (aCL)1, anti-β2glycoprotein I (anti-β2GPI)1 and anti-phosphatidylserine/prothrombin antibodies (aPS/PT)1 were determined in sera of 585 consecutive patients with inflammatory rheumatic diseases and different conditions (Table 1) between January 1 and November 30, 2014. Medical records were analyzed, looking at patient age, gender, body mass index (BMI), thrombocytopenia, arterial hypertension, hyperlipidemia, diabetes, smoking, history of thrombotic or obstetric complications and current therapy including oral contraception. Table 1: Patients’ clinical characteristics
*Raynaud’s phenomenon, migraine, depression, fibromyalgia, ischemic lesions.
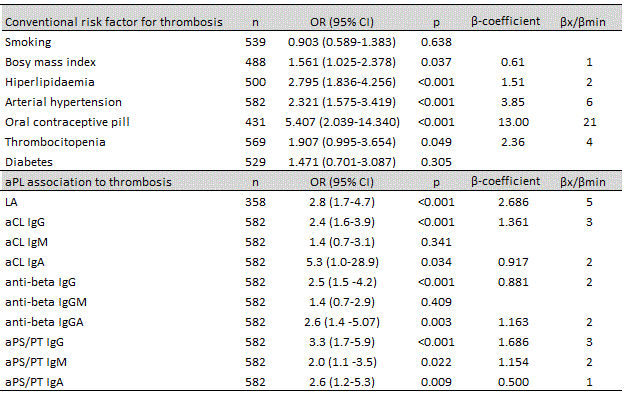
Results: A univariate logistic regression revealed that BMI, hiperlipidemia, arterial hypertension, use of oral contraceptive pill and thrombocytopenia were significantly associated with thrombosis (Table 2). Among tested aPL only IgM isotype of aCL and anti-β2GPI showed no association to thrombosis. A thrombotic risk score calculation (TRS) was constructed by assigning to each of the 13 variables showing significant correlation to thrombosis, a number of points proportional to its β-regression coefficient divided by the value of the lowest β-coefficient (βx/βmin). TRS values were significantly higher in patients with thrombosis than non-thrombotic patients (median (IQR) 2 (0-7) ) vs. 8 (2-13), p<0.001), showing area under ROC curve of 0.703. Table 2: Association of risk factors to thrombosis
Conclusion: Our results show that, in addition to various conventional risk factors, aPS/PT (all isotypes), aCL (IgG and IgA) and anti-β2GPI (IgG and IgA) associate with thrombotic risk in patients with autoimmune diseases. Calculation of a TRS accounting for significant conventional risk factors and aPL, better assesses thrombotic risk in different patients with autoimmune diseases compared to evaluating individual or just conventional factors alone.
1. Zigon et al, Thrombosis, Atherosclerosis and Atherothrombosis – New Insights and Experimental Protocols, Chapter 6, InTech 2015
To cite this abstract in AMA style:
Žigon P, Podovšovnik A, Ambrozic A, Tomsic M, Hocevar A, Gaspersic N, Rotar Z, Praprotnik S, Sodin Semrl S, Čučnik S. Association of Conventional Risk Factors and Antiphospholipid Antibodies to Thrombosis in Patients with Autoimmune Diseases: Lessons Learned from a Year-Long Systematic Assessment [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/association-of-conventional-risk-factors-and-antiphospholipid-antibodies-to-thrombosis-in-patients-with-autoimmune-diseases-lessons-learned-from-a-year-long-systematic-assessment/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/association-of-conventional-risk-factors-and-antiphospholipid-antibodies-to-thrombosis-in-patients-with-autoimmune-diseases-lessons-learned-from-a-year-long-systematic-assessment/