Session Information
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Recently, the use of hematologic indexes as markers of systemic inflammation has been reported in oncological, cardiovascular and rheumatic diseases. Only 2 studies evaluated their role in polymyalgia rheumatica (PMR).
Our objective was to primarily compare the levels of neutrophil- (NLR), monocyte- (MLR), eosinophil- (ELR), basophil- (BLR) and platelet to lymphocyte ratio (PLR) in PMR and control patients without inflammatory conditions and, secondarily, to evaluate their use as prognostic markers in PMR.
Methods: This retrospective case control study included 63 patients with PMR and 101 patients without inflammatory conditions who attended our Hospital. Clinical data and blood cell counts at diagnosis (prior to start treatment) were obtained from medical records and laboratory reports.
We compared the indexes of both groups at diagnosis by a Student’s t test and sequentially performed a subgroup analysis in PMR patients in order to determinate the utility of the indexes to evaluate prognosis, relapses and recurrences. We also analyzed the use of methotrexate as a marker of more severe disease. A correlation with inflammatory markers using Student’s t test and Pearson correlation coefficient was performed
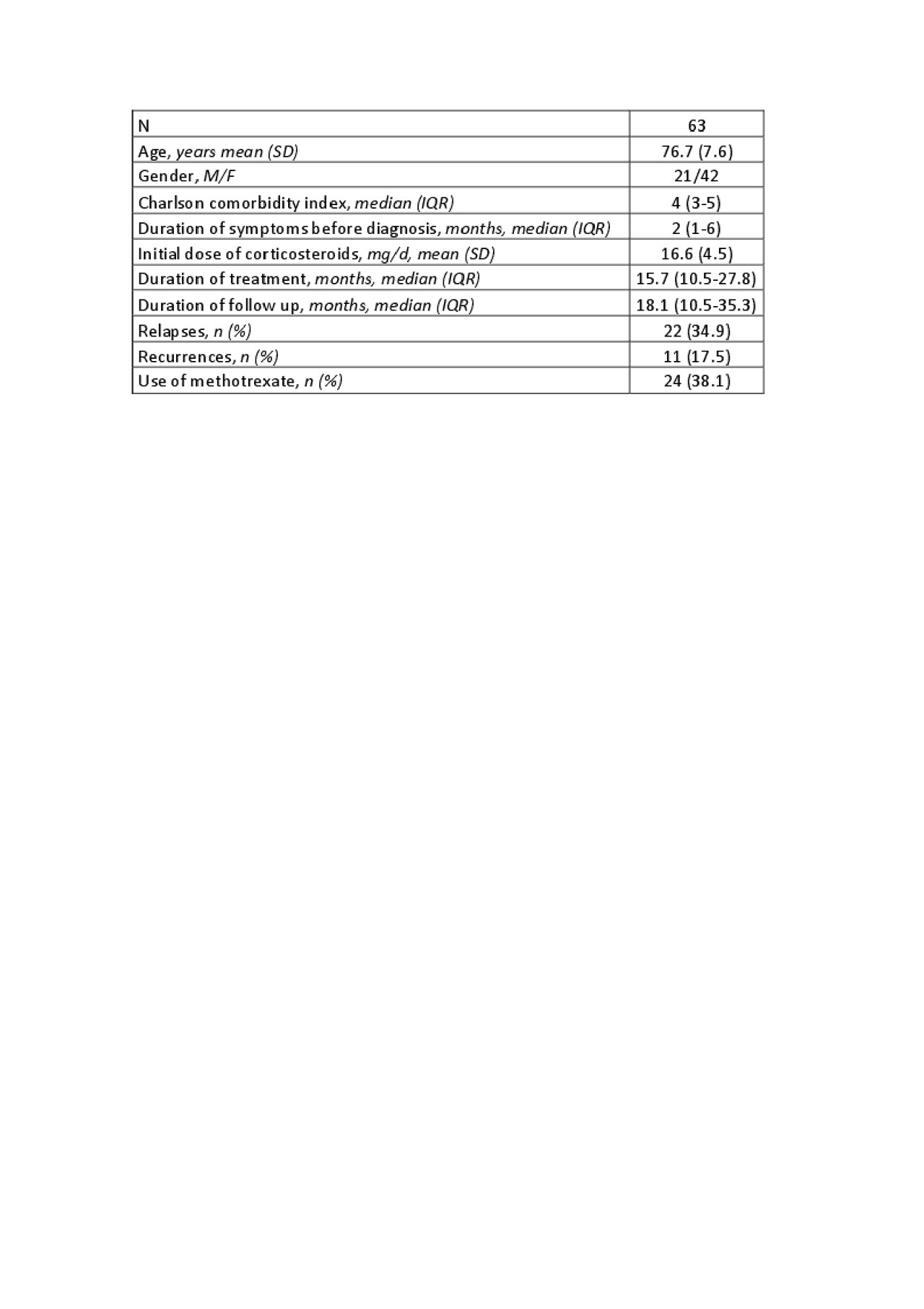
Results: Age, gender and laboratory data of PMR and control patients are shown in Table 1. The control group included patients with osteoarthritis (78,2%), fibromyalgia (9.9%) and others soft tissue non inflammatory conditions (11.9%). NLR and MLR levels were significantly higher in PMR patients than controls (NLR 2.77 vs 1.99, p < 0.001 and MLR 0.37 vs 0.27, p < 0.001). All the other indexes did not differ between populations. Clinical characteristics of PMR patients are shown in Table 2. The median time of follow up of PMR patients was 24.1 months (IQR 10.5-35.3). When evaluating this subgroup of patients, neither NLR nor MLR were associated with relapses, recurrences or need of methotrexate during follow up. Results shown in table 3. No correlation was found between both indexes and the duration of symptoms before diagnosis and duration of glucocorticoid treatment. The median erythrocyte sedimentation rate (ESR) was 41.5 mm/hr (19 – 62) and C reactive protein (CRP) level was 2.48 mg/L (0.54 – 3.38) at diagnosis. We found a poor correlation between NLR and MLR and ESR and CRP levels. Fourteen PMR patients (22.2%) had normal values of ESR and CRP. However, the treating physician considered the diagnosis on a clinical basis and started treatment accordingly. When comparing NLR and MLR levels, there were no differences between this group and control patients; on the other hand, a significant difference was found with PMR patients who presented with high levels of acute phase reactants.
Conclusion: NLR and MLR levels were significantly higher in PMR patients than controls. Baseline indexes did not correlate adequately with acute phase reactants and they were not able to predict a poor outcome in PMR.
To cite this abstract in AMA style:
de la Torre M, Pisoni C. Are Hematologic Indexes Helpful in the Diagnosis and Prognosis of Polymyalgia Rheumatica? [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/are-hematologic-indexes-helpful-in-the-diagnosis-and-prognosis-of-polymyalgia-rheumatica/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/are-hematologic-indexes-helpful-in-the-diagnosis-and-prognosis-of-polymyalgia-rheumatica/