Session Information
Session Type: ACR Concurrent Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose: Although significant advances have been made in treating inflammation in RA, little is known about central nervous system (CNS) pain pathways in inflammatory arthritis. Recognizing this gap in knowledge, the ACR Pain Management Task Force emphasized the need for quantitative, non-invasive biomarkers of pain and the application of these measures to the study of pain. Our objective was to use pulsed arterial spin labeling (pASL), a type of functional MRI, to evaluate the neural correlates of clinical pain in RA and to characterize changes in CNS pain pathways in response to DMARD treatment.
Methods: This pilot study included 2 stages: 1) a cross-sectional analysis of 15 RA patients with active disease compared to 16 age- and sex-matched controls, and 2) a prospective analysis of 10 RA patients followed for 12-weeks after starting DMARD treatment. To be included, RA patients had to have chronic pain with an average of at least 3/10 in intensity at the MCPs and be starting a DMARD for active disease. Controls could not have current pain or have a history of chronic pain conditions or systemic inflammatory disease. All subjects underwent 6-min pulsed arterial spin labeling scans (voxel size = 3.515*3.515*6.25 mm, number of slices = 16) to assess regional cerebral blood flow (rCBF) using a 3T Siemens MAGNETOM Skyra, with a 32-channel head coil. Scans were obtained under the following conditions: resting state and pressure at the left MCP joints. The experimental stimulus was applied using a blood pressure cuff inflated to achieve 40/100 pain in the patients and using the same pressure for the matched controls. RA patients were followed for 12-weeks after starting a DMARD and scanned again at the end of the treatment using the same parameters.
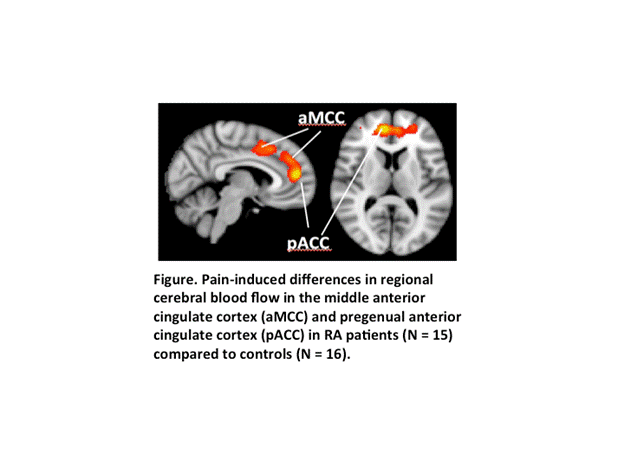
Results: The pressure stimulus was more painful in RA patients (median 50.0; interquartile range (IQR) 36.5-65.0) than in controls (median 3.5; IQR 0-11.3; p = 0.0001). Accordingly, a significant stimulus-induced increase in rCBF in the middle anterior and pregenual anterior cingulate cortices (aMCC/pgACC) was observed only in RA patients (Figure).The group x condition interaction trended for significance in a region-of-interest analysis (p = 0.065). After 12-weeks of treatment with a DMARD, normalized rCBF in the aMCC/pgACC decreased from a mean ± SD of 0.92 ± 0.08 to 0.87 ± 0.10 (one-sided p = 0.10), becoming similar to control values (0.87 ± 0.10).
Conclusion: These preliminary results suggest that: a) pASL may be able to identify CNS pathways involved in the regulation of pain in RA, and b) activity in these pathways may change in response to DMARD treatment. The aMCC and pgACC are brain regions that have been implicated in the cognitive modulation of pain affect in chronic, non-inflammatory pain states. Larger studies are needed to determine if rCBF in these regions will be useful as as an objective biomarker of pain in future studies evaluating the efficacy of pain interventions in RA.
To cite this abstract in AMA style:
Lee YC, Fine A, Protsenko E, Massarotti E, Edwards RR, Napadow V, Loggia M. A Pilot Pulsed Arterial Spin Labeling Study of Regional Cerebral Blood Flow in Response to Pain in RA, before and after DMARD Treatment [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/a-pilot-pulsed-arterial-spin-labeling-study-of-regional-cerebral-blood-flow-in-response-to-pain-in-ra-before-and-after-dmard-treatment/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/a-pilot-pulsed-arterial-spin-labeling-study-of-regional-cerebral-blood-flow-in-response-to-pain-in-ra-before-and-after-dmard-treatment/