Session Information
Session Type: ACR/ARHP Combined Abstract Session
Session Time: 9:00AM-11:00AM
Background/Purpose: Patients with SLE often require additional medical management outside of the outpatient setting from ED visits to hospital admissions. Previous studies in the general population showed that those who frequently visit the ED mostly do so over a limited time period (<12 months); however, a subgroup are persistent frequent ED users over years. We examined whether persistent and limited ED utilization in SLE patients are associated with patient characteristics, SLE history, long term opioid therapy (LTOT), and general health status.
Methods: We conducted a retrospective study of SLE patients who frequented the ED for ≥3 visits in a calendar year from 2013-2016. Limited use was defined as meeting criteria for frequent ED use for 1 out of the 4 years. Persistent users met these criteria for at least 2 out of the 4 years, consecutive or non-consecutive during the study period. Patient demographics, medical history, and ED encounter information were collected through in-depth electronic health record review. Each ED encounter was categorized into the following groups; SLE-, infection-, pain-related, or “other”. Multivariate logistic regression was used to evaluate factors associated with frequent ED utilization.
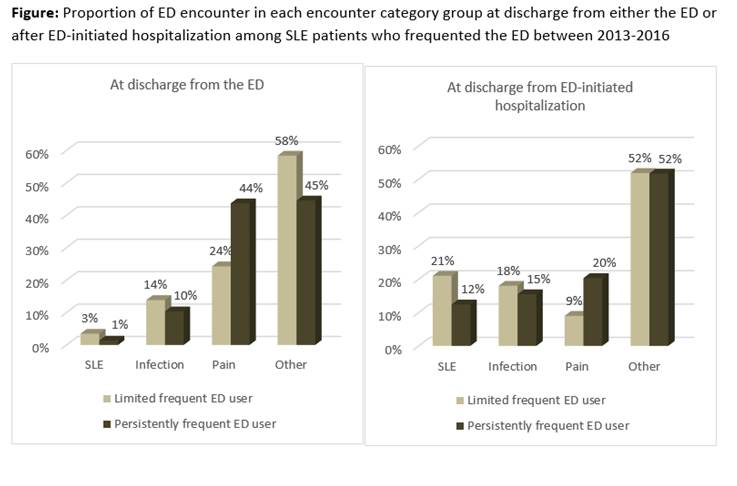
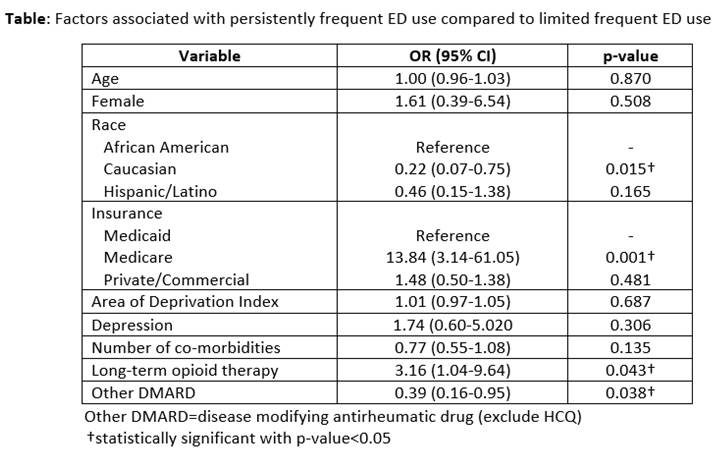
Results: We identified 52 limited users who had 335 ED encounters, and 77 persistent users who had 1143 encounters; average age 41.5 (SD 15.6), 116 (90%) female, 76 (58%) with Medicaid insurance coverage, and 77 (60%) African American, 27 (21%) Caucasian, and 25 (19%) Hispanic/Latino. Persistent users had more than twice the average number of ED visits (mean 14.8, SD 8.8) compared to limited users (mean 6.4, SD 2.0), and had more ED-initiated hospitalizations (49% vs 40%, respectively). Pain-related ED visits were more common among persistent users (32%) than limited users (18%) (see Figure). In multivariate analysis, persistently frequent ED users were more likely to be African American, have Medicare insurance coverage and be on LTOT, but less likely to be on other DMARD, than their respective counterparts who are limited frequent ED users (see Table).
Conclusion: Among SLE patients who persistently frequent the ED, pain is a major cause for both ED utilization and ED-initiated hospitalizations. This group of SLE patients who account for a high volume of healthcare resource utilization may be amenable to targeted interventions to improve pain management and care coordination in the outpatient setting. Further research is needed to improve quality of care and reduce healthcare resource utilization among SLE patients who frequently utilize the ED.
To cite this abstract in AMA style:
Lin J, Lee J, Suter LG, Fraenkel L. A Comparison of Persistent Versus Limited Frequent Emergency Department (ED) Utilization Among Systemic Lupus Erythematosus (SLE) Patients [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/a-comparison-of-persistent-versus-limited-frequent-emergency-department-ed-utilization-among-systemic-lupus-erythematosus-sle-patients/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/a-comparison-of-persistent-versus-limited-frequent-emergency-department-ed-utilization-among-systemic-lupus-erythematosus-sle-patients/