Session Information
Session Type: Abstract Submissions (ACR)
Results: A total of 9440 RA and 31,009 matched non-RA pts were included in the study. Mean [SD] age was 56.8 [14.1] for RA and 56.5 [13.9] years for non-RA pts, and 76% were female in both groups. At baseline, 42.9% of RA pts had hypertension, 30.2% had dyslipidemia, 22.9% were obese, and 11.6% were smokers, whereas 32.4% of non-RA pts had hypertension, 35.8% had dyslipidemia, 23.1% were obese, and 10.5% were smokers. Mean [SD] number of office visits during the first yr of follow-up was higher in RA compared with non-RA pts (13.2 [10.8] vs 8.2 [9.1], p<0.001). Rates of BP measurement for treated hypertension and low-density lipoprotein (LDL) cholesterol measurement for treated dyslipidemia were higher in pts with RA compared with non-RA pts (BP: 99.4 vs 91.8%, p<0.001; LDL: 89.6 vs 84.9%, p<0.001). Treatment rates for hypertension were slightly higher in pts with RA compared with non-RA pts (95.0 vs 92.5%, p<0.001) and similar for dyslipidemia (75.1 vs 74.5%, p=0.393). RA pts and non-RA pts had similar rates of BP control but higher rates of LDL and A1C control (BP: 65.2 vs 60.2%, p=0.996; LDL: 65.5 vs 59.7%, p=0.005; A1C: 51.8 vs 42.6%, p<0.001). These results were consistent with results for pts with osteoarthritis as a matched non-RA group.
Conclusion: CRF management in pts with RA was slightly better than the management in non-RA pts in a US managed care setting. The finding of this analysis indicates that the higher CV risk in pts with RA is unlikely to be driven by poor control of traditional CV risk factors.
Figure. Traditional CRF Management for RA and Matched Non-RA Pts 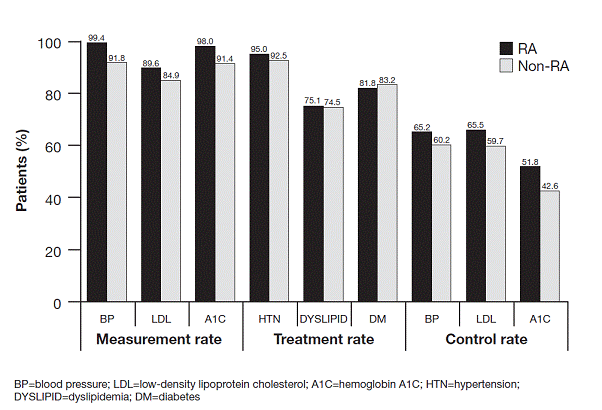
Disclosure:
J. An,
BMS, Genentech, Merck ,
2;
K. Reynolds,
None;
E. Alemao,
Bristol-Myers Squibb,
1,
Bristol-Myers Squibb,
3;
H. Kawabata,
Bristol-Myers Squibb,
1,
Bristol-Myers Squibb,
3;
D. H. Solomon,
None;
K. P. Liao,
None;
T. C. Cheetham,
BMS, Gilead,
2.
« Back to 2014 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/traditional-cardiovascular-risk-factor-management-in-patients-with-rheumatoid-arthritis-compared-with-matched-non-rheumatoid-arthritis-patients-in-a-us-managed-care-setting/
