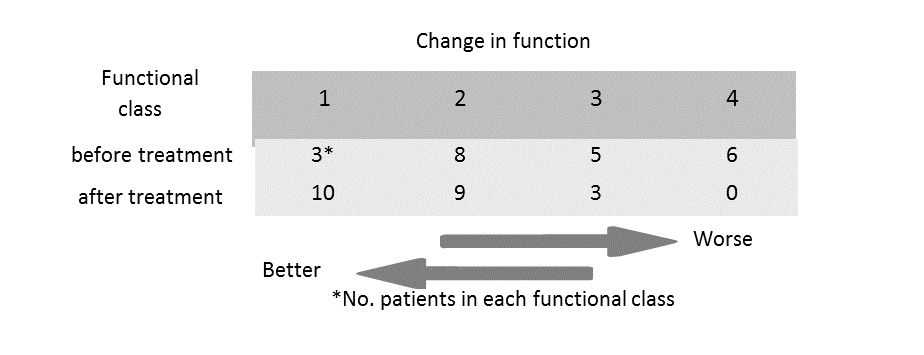Session Information
Session Type: Abstract Submissions (ACR)
Background/Purpose:
Pulmonary disease in patients with idiopathic inflammatory myopathies, polymyositis (PM), dermatomyositis (DM), and clinically amyopathic dermatomyositis (CADM) is a major cause of morbidity. Approximately 35-40% of patients with PM/DM/CADM develop interstitial lung disease (ILD) during the course of their illness. Mortality ranges from 45-71% in those with ILD. Treatment of ILD in patients with inflammatory myopathies remains a challenge. In the absence of evidence-based data from randomized control trials, corticosteroids are regarded as the mainstay of therapy, although their effect is variable.
Methods:
We retrospectively evaluated 62 patients with idiopathic inflammatory myopathies treated during the past ten years.
Results:
Of the 62 patients reviewed, 22 developed ILD with varying degrees of functional impairment; 11 of the 22 had PM, 8 had DM and 3 had CADM. Three eventually died of causes unrelated to their lung disease. Pulmonary disease severity was judged by measuring blood oxygen saturation, dyspnea and tachypnea at rest, and following exercise, radiographic evidence of pulmonary infiltration and signs of pulmonary restriction and impaired diffusion capacity by pulmonary function testing. Patients were followed for at least 24 months, with an average length of follow up of 121 months. All ILD patients received combination therapy with an average number of 3 immune modulating agents plus corticosteroids. Four out of the 7 patients with severe ILD received concomitant combination therapy with IVIG, cyclophosphamide and cyclosporine for up to 6 months; 7 other moderate to severely affected patients received IVIG plus cyclosporine in addition to corticosteroids. Patients’ functional capacity before and after treatment was evaluated according to the NYHA criteria developed for the assessment of patients with heart failure. The table (below) demonstrates that immunomodulatory therapy resulted in a statistically significant improvement, (Chi Square = 10.3, Df =3 p < 0.02). One patient developed Candida pneumonia and 3 who were treated with cyclosporine and other agents had reversible declines in renal function during therapy. Four patients developed Herpes Zoster during the follow up period, but long after the aggressive immunomodulatory therapy was finished. Treatment was otherwise well tolerated.
Conclusion:
Our results support the early use of aggressive immunomodulatory therapy with a combination of agents designed to interfere with T cell recruitment, activation and replication in patients with idiopathic inflammatory myopathies and ILD.
Disclosure:
R. Mihu,
None;
R. D. Rossen,
None;
J. Popovich,
None;
S. L. Sessoms,
None.
« Back to 2012 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/significant-functional-improvement-using-aggressive-immunomodulatory-therapy-in-patients-with-inflammatory-myopathy-and-interstitial-lung-disease/