Session Information
Session Time: 6:00PM-7:00PM
Background/Purpose: Behçet’s disease (BD) is a systemic vasculitis primarily characterized by recurrent oral and genital aphthous ulceration. It is reported that 15-20% of all BD patients develop during childhood. Pediatric BD (pBD) differs from adult BD in the disease manifestations, severity, and outcome. Diagnosis, however, may be challenging due to the absence of specific testing and long time interval from initial disease features to diagnosis. It is described that pBD has a lower severity score and activity index compared to adults.
Methods:
With institutional review board approval, we retrospectively reviewed patients with a diagnosis of BD, from 2011 to 2024. Demographics, clinical manifestations, treatment modalities, and disease course were abstracted. Descriptive statistics were utilized for analysis.
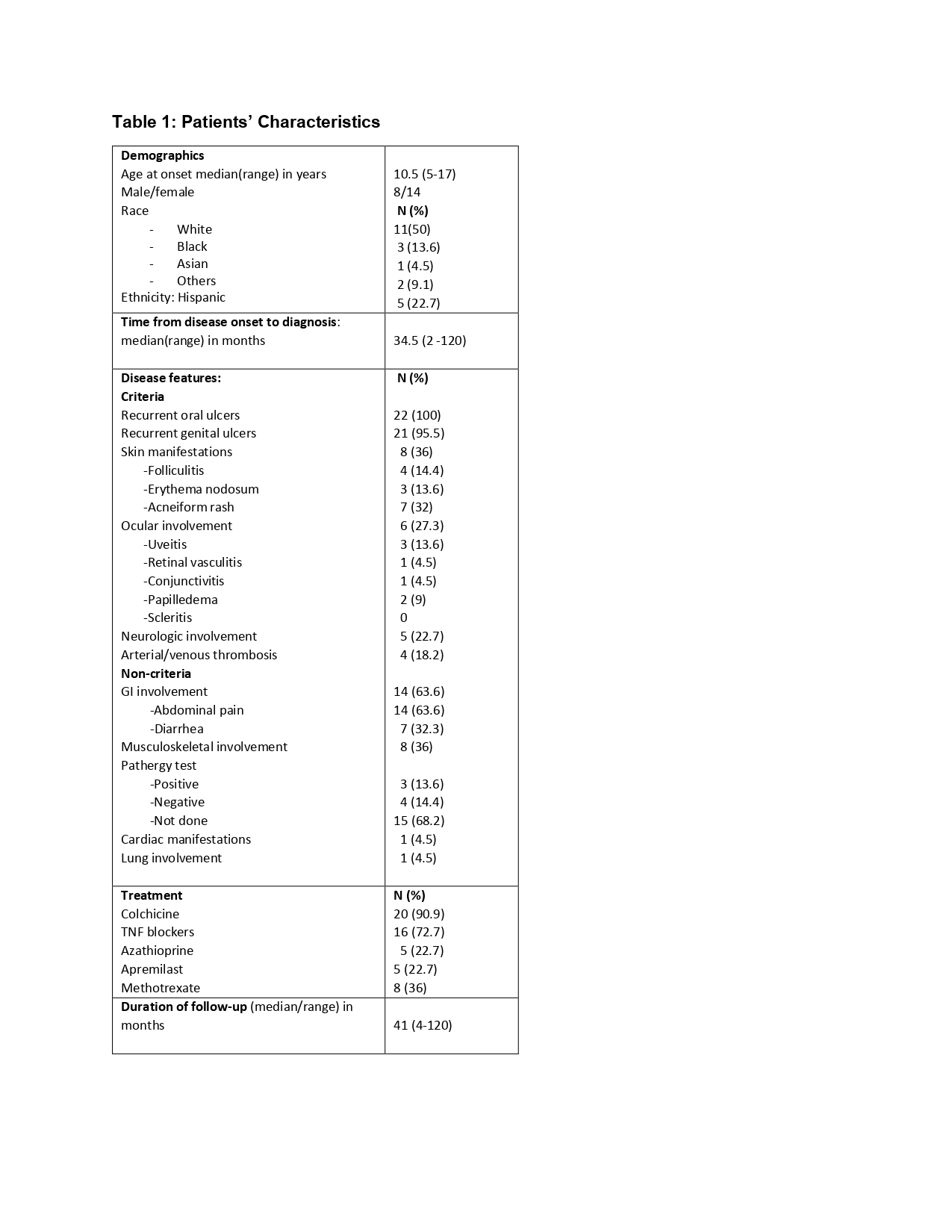
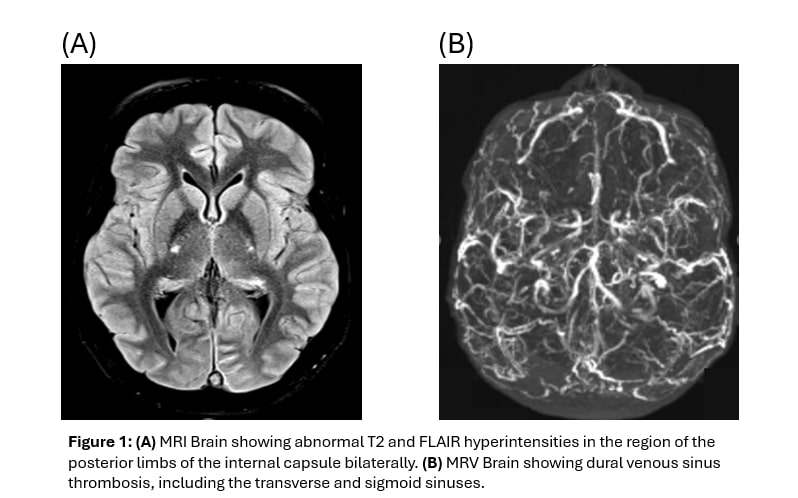
Results: A total of 25 patients were identified; 3 patients did not fulfill diagnostic criteria and were excluded. 14 (63.6%) of the patients were female, whereas 11 (50%) of the patients were Caucasian. The median time interval from disease onset to diagnosis was 34.5 months. Recurrent oral ulcers were the initial presentation in 80% of patients, while recurrent genital ulcers were initially noted in only 9.5%. Multiorgan involvement was common, with notably high neurological involvement at 22.7% (Table 1, 2).
The most common treatment modalities were colchicine (90.9%) and TNF blockers (72.7%). The majority of patients received steroids as part of induction therapy or during disease flares. Despite treatment, the course was characterized by disease flare, primarily of oral ulceration with genital involvement in 66%. While most patients achieved favorable outcomes with mild disease flares following appropriate treatment, those presenting with major organ involvement, particularly neuro-Behçet’s disease and severe vasculitis, required intensive immunomodulatory therapy. 4/5 (80%) of patients with Neuro-Behçet achieved a good outcome.
Conclusion: This study underscores the complex and challenging nature of pBD, with nearly a quarter of patients developing neurologic manifestations, indicating a higher burden of severe disease than traditionally recognized. The substantial diagnostic delay of almost three years, despite 80% initially presenting with oral ulcers, represents a modifiable gap in care that may contribute to progression toward major organ involvement. Improving prognosis in pBD, particularly for those at risk of Neuro-Behçet requires heightened clinical suspicion, earlier referral, systematic neurologic screening, and neuroimaging in high-risk patients. Timely escalation to targeted immunosuppressive and biologic therapy within coordinated multidisciplinary care pathways is essential for optimizing patient outcomes.
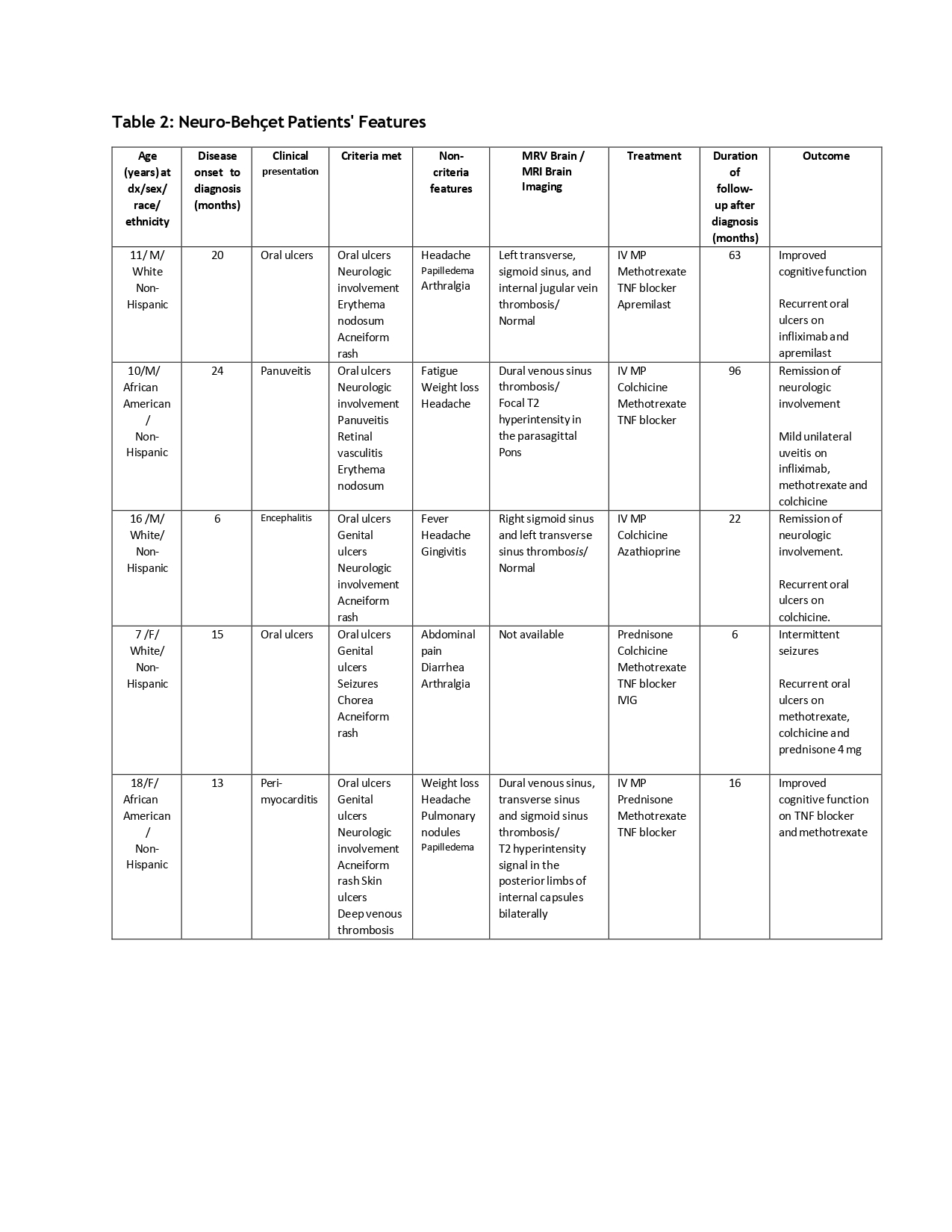 *MP: methylprednisolone; TNF: Tumor necrosis factor.
*MP: methylprednisolone; TNF: Tumor necrosis factor.
To cite this abstract in AMA style:
Elrefai R, Ramirez A, Lai J, Yildirim-Toruner C, Muscal E, DeGuzman M. Pediatric Behçet’s Disease: A 13-Year Single-Center Experience Highlighting Diagnostic Delays and High Neurological Burden [abstract]. Arthritis Rheumatol. 2026; 78 (suppl 3). https://acrabstracts.org/abstract/pediatric-behcets-disease-a-13-year-single-center-experience-highlighting-diagnostic-delays-and-high-neurological-burden/. Accessed .« Back to 2026 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/pediatric-behcets-disease-a-13-year-single-center-experience-highlighting-diagnostic-delays-and-high-neurological-burden/