Session Information
Session Type: Abstract Submissions (ACR)
Background/Purpose: Increased cardiovascular (CV) mortality in established rheumatoid arthritis (RA) is a widely accepted threat, but in early RA or inception cohorts, growing evidence suggests no increased CV mortality. The aim of this study was to assess the CV mortality in early RA patients diagnosed in the 2000s, and to compare it with the general population.
Methods: All incident RA patients over 16 years of age diagnosed in 2000–2007 were identified from a Finnish nationwide register maintained by the Social Insurance Institution (M05 for RF positive and M06 for RF negative RA). Death certificate data were obtained from the National Population Registry until the end of 2008, and CV disease was identified as the primary cause of death by the ICD-10 codes I00–99. The number of CV deaths was calculated in subgroups according to sex, age, RF status, and calendar year. The cumulative incidence of CV deaths was assessed with adjustment for competing risks—that is, deaths due to causes other than CV disease. The expected number of CV deaths in each subgroup was calculated on the basis of CV death rates in the age- and sex-specific general population (data obtained from Statistics Finland), and a standardized mortality ratio (SMR) was calculated with 95% CIs.
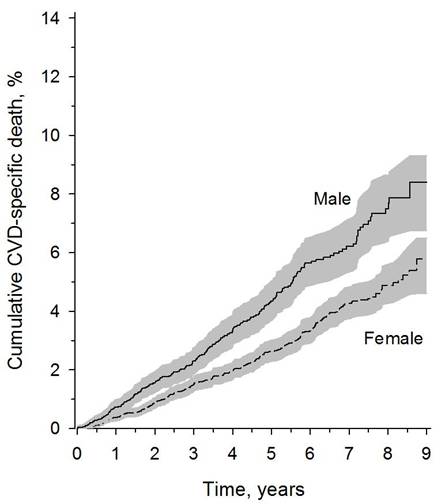
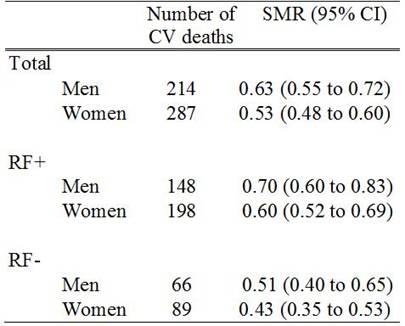
Results: During the 8-year follow-up period, 14,878 new RA patients were identified (68% women, 63% RF positive). The mean age was 55.8 (SD 15.8) years in women and 57.5 (SD 13.9) years in men at the time of RA diagnosis. By the end of 2008, 501 patients had died of CV causes. Cumulative incidence analysis adjusted for competing risks showed that CV mortality at five/eight years after the diagnosis of RA was 2.6%/5.8% in women and 4.4%/8.4% among men (Figure 1). The SMR in the entire RA cohort was 0.57 (95% CI 0.52 to 0.62). The SMRs in subgroups according to sex and RF status varied from the lowest value of 0.43 among the RF negative women to 0.70 among the RF positive men (Table 1). Male sex and the presence of RF increased the risk of CV death: the sub-hazard ratios (sHR) were 1.73 (95% CI 1.45 to 2.05, p<0.001) and 1.33 (1.10 to 1.60, p=0.003), respectively.
Conclusion: In this nationwide early RA cohort, CV mortality was substantially lower than in the age- and sex-specific general population. This reduction in CV deaths may reflect both the recent advances in the management of systemic inflammation and the improved recognition and treatment of CV risk factors in RA. With longer disease duration, this favorable CV prognosis may deteriorate.
Figure 1. Estimated cumulative incidence functions for cardiovascular-disease-specific (CVD-specific) death among patients with RA.
Table 1.
Disclosure:
A. M. Kerola,
None;
T. Nieminen,
None;
L. J. Virta,
None;
H. Kautiainen,
None;
K. Puolakka,
None;
T. Kerola,
None;
T. Pohjolainen,
None;
M. J. Kauppi,
None.
« Back to 2013 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/low-cardiovascular-mortality-among-early-rheumatoid-arthritis-patients-a-nationwide-register-study-2000-2008/