Session Information
Session Time: 6:00PM-7:00PM
Background/Purpose: Improving outcomes for children with systemic lupus erythematosus (SLE) is imperative given the morbidity associated with this disease and the significant disparities. Social drivers of health (SDOH) – the conditions in which people live, work, learn, and play – are known to strongly influence health outcomes. After conducting a successful quality improvement project at our site to implement SDOH screening in our patients with SLE and refer patients to a social care platform linking our patients to community resources, we sought to assess for differences in outcomes based on patients that had identified social needs and/or were wanting assistance with housing, food, utilities, or transportation.
Methods: We assessed all of our patients with SLE seen between December 2024 and September 2025. A positive SDOH screen (pSDOH) included an identified social need and/or wanting assistance with housing, food, utilities, and/or transportation. A patient with at least 1 positive screen (even if additional screens were negative) was included in the pSDOH subset of patients. We collected demographic variables including race, ethnicity, and language in addition to diagnosis date, steroid use, emergency department visits, and hospitalizations. Outcomes related to disease activity include average SLEDAI score, low SLEDAI (score ≤4), and average physician global assessment of disease activity (PGA). Patient-reported outcomes include average patient/parent global assessment of overall wellbeing (PtGA) and low PtGA (score ≤2).
Results: We evaluated data from 76 patients. Twenty-one patients (27.6%) had a pSDOH (Table 1). A higher percentage of patients with a pSDOH identified as Black (23.8% vs 12.7%) or Hispanic (33.3% vs 23.6%) compared to patients with a negative SDOH screen. A non-English primary language was also higher in the pSDOH group (23.8% vs 9.1%). Additionally, the pSDOH group had higher no show and last-minute cancellation rates (Table 2). The average disease duration was less for the pSDOH subset (29.8 vs 41 months), but the range was similar. The pSDOH group had higher steroid use (48.1% vs 17.9%), greater SLEDAI scores (4.42 vs 2.67), and less visits with a low SLEDAI score (66.7% vs 82.9%). Average PGA and PtGA scores were also higher in the pSDOH group (1.41 vs 0.55 and 2.61 vs 1.75, respectively). Lastly, ED visits and hospitalizations per patient were higher in our pSDOH cohort.
Conclusion: Patients with pSDOH had increased no shows, last-minute cancellations, acute care visits, and steroid use compared to patients with consistently negative SDOH screens. Furthermore, both disease activity and patient-reported outcomes were worse in the pSDOH group. This data substantiates our continued efforts to do SDOH screening and refer patients/families to community-based organizations for resources and support. Future efforts will assess for changes in outcomes and healthcare utilization if families receive community services and no longer identify social needs.
Table 1. Demographic information of our patients with SLE. 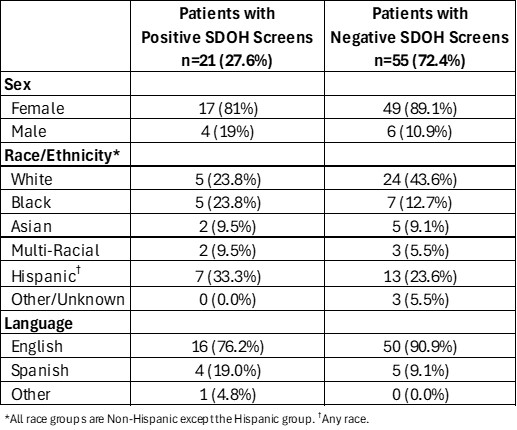
Table 2. Disease information and outcomes of our patients with SLE.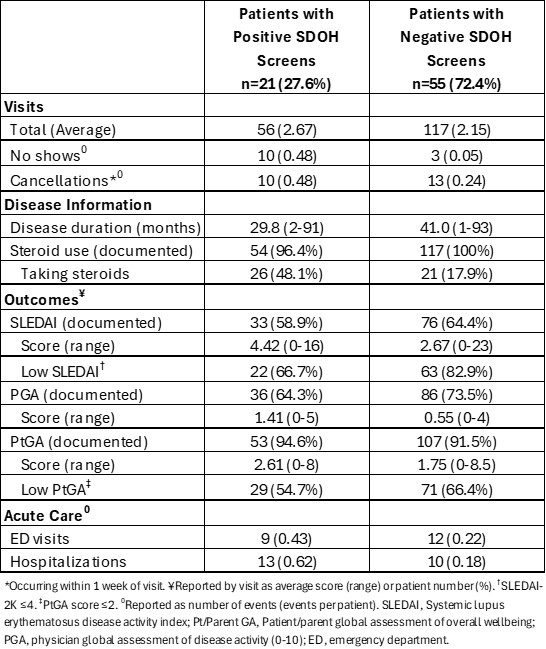
To cite this abstract in AMA style:
Harris J, Parish S, Holland M, Favier L, Fox E, Ibarra M, Jones J, Hoffart C, cooper a. Impacts of Social Drivers of Health on Outcomes for Patients with Pediatric Systemic Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2026; 78 (suppl 3). https://acrabstracts.org/abstract/impacts-of-social-drivers-of-health-on-outcomes-for-patients-with-pediatric-systemic-lupus-erythematosus/. Accessed .« Back to 2026 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/impacts-of-social-drivers-of-health-on-outcomes-for-patients-with-pediatric-systemic-lupus-erythematosus/
