Session Information
Session Time: 6:00PM-7:00PM
Background/Purpose: Chronic uveitis is an immune-mediated disease that can cause severe complications, including blindness. Chronic uveitis care involves numerous medical visits, frequent laboratory monitoring and complex medication regimens that impose considerable expense. Social determinants of health (SDoH) influence health outcomes but little is known about the specific impacts of SDoH on outcomes in pediatric uveitis. The aim of this study is to assess the extent to which various SDoH impact visual outcomes in pediatric uveitis through a survey of patients treated in a multi-disciplinary pediatric uveitis clinic.
Methods: Patients from a multidisciplinary uveitis clinic at a large children’s hospital in the Midwestern United States were prospectively enrolled and completed a novel survey designed to assess various SDoH. Demographics, uveitis clinical features, treatments, clinical outcomes and complications were obtained through retrospective chart review. The Child Opportunity Index (COI), a composite measure of neighborhood opportunities influencing child health, was determined for each participant based on home zip code. Descriptive statistics were used to describe the patient population. The impact of various SDoH on outcomes was assessed using Wilcoxon rank-sum test for continuous variables and chi-square or Fisher’s exact test for categorical variables.
Results: Sixty-four subjects were enrolled. Demographics and clinical characteristics of the population are described in table 1. Most subjects were white (84.4%), non-Hispanic (85.9%) and female (67.2%). Juvenile idiopathic arthritis (JIA) was the most common underlying condition. Thirty-nine (60.9%) had at least one uveitis complication, 15 (23.4%) required eye surgery, and 15 (23.4%) had moderate or severe visual impairment (best corrected visual acuity (BCVA) worse than 20/50) in at least one eye. Subjects who identified as black or African American were more likely to have ocular complications of uveitis (p=0.018). Median LogMAR BCVA among subjects with low or very low COI was worse compared to those with moderate, high or very high COI (0.18 (IQR 0,0.48) vs 0 (IQR 0,0.1), p=0.046), though difference in rates of moderate or severe visual impairment (BCVA worse than 20/50 (LogMAR 0.4) in at least one eye)) between the groups did not reach statistical significance (p=0.322). Other SDoH evaluated were not associated with statistically significant differences in visual acuity, complications or surgery.
Conclusion: Among children with uveitis followed in a specialized, multidisciplinary clinic, outcomes were similar across most social determinants of health assessed. Black race was associated with more uveitis complications and children with lower COI had slightly worse visual acuity, though not reaching the threshold of a clinically significant visual impairment. These results may not be translatable to all patient populations given the highly coordinated care provided in our clinic setting.
Subject Demographics and Clinical Characteristics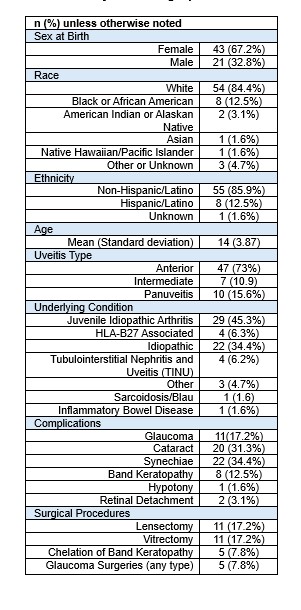
Social Determinants of Health Impact and Clinical Outcomes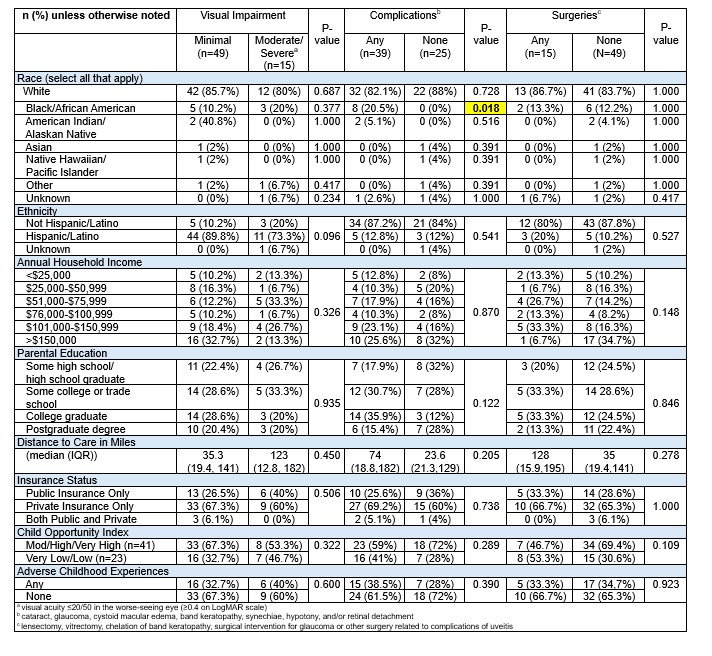
To cite this abstract in AMA style:
stahl e, lytch a, Noel-Macdonnell J, cooper a. Impact of Social Determinants of Health on Outcomes in Pediatric Uveitis [abstract]. Arthritis Rheumatol. 2026; 78 (suppl 3). https://acrabstracts.org/abstract/impact-of-social-determinants-of-health-on-outcomes-in-pediatric-uveitis/. Accessed .« Back to 2026 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/impact-of-social-determinants-of-health-on-outcomes-in-pediatric-uveitis/
