Session Information
Session Time: 5:00PM-6:00PM
Background/Purpose:
The etiology of juvenile spondyloarthritis (SpA) remains unclear; however, interactions between genetic susceptibility and environmental triggers, particularly those originating in the gastrointestinal tract, are thought to play a role. Infancy is a critical period for establishing the gut microbiome, which subsequently stabilizes throughout childhood and adulthood. Disruptions in early-life microbial composition may impair immune development and increase vulnerability to immune-mediated diseases.The objective of this study was to investigate the independent association between early-life exposures that influence gut microbiome development, with a primary focus on antibiotic use, and the subsequent risk of SpA and juvenile SpA (JSpA).
Methods:
We conducted a matched case-control study using data from the Danish National Patient Registry (NPR), the Danish Medical Birth Registry (MBR), the Danish National Prescription Registry, and the Danish Civil Registration System spanning 1998–2024. Cases included individuals diagnosed with SpA, psoriatic arthritis (PsA), or inflammatory bowel disease-associated arthritis (IBD-AA) before age 21. Controls were matched 1:50 on birth year, sex, and calendar year of SpA diagnosis date. The primary outcome was a diagnosis of SpA (including PsA, SpA, and IBD-AA) diagnosed at ≤21 years. The primary exposure was antibiotic use during the first year of life. Secondary exposures of interest included: class of antimicrobial (penicillin, broad-spectrum penicillin, macrolides), number of antimicrobial courses, mode of delivery (cesarean or vaginal), upper respiratory tract infection (any), systemic nonbacterial antimicrobial agent (any). Odds ratios (OR) were computed using conditional logistic regression, with analyses stratified by SpA subtype (SpA, PsA, and IBD-AA ).
Results: A total of 560 cases met the inclusion criteria. Subject characteristics are presented in Table 1. Among cases, 59% had SpA, 28% PsA, and 13% IBD-AA. The median age at diagnosis was 16.8 years (IQR: 13.0-18.7). Antibiotic exposure during the first year of life occurred in 50% of cases and 42% of controls; 12% of cases and 10% of controls received ≥3 antibiotic courses. In adjusted analyses, any antibiotic exposure during the first year of life was associated with increased odds of SpA (OR 1.35, 95% confidence interval [CI] 1.14–1.59). A dose–response relation was observed (OR 1.47 for ≥3 courses vs OR 1.24 for 1 course; Table 2). Other early-life exposures that were significantly associated with SpA risk included upper respiratory infections (OR 1.99, 95% CI 1.40–2.82).
Conclusion:
Early-life antibiotic exposure was independently associated with increased risk of SpA, with evidence of a dose–response relation. Additional early-life infections also contributed to higher disease risk. These findings support the hypothesis that microbiome-altering exposures during infancy may influence later susceptibility to juvenile spondyloarthritis and related conditions.
Table 1. Cases and matched controls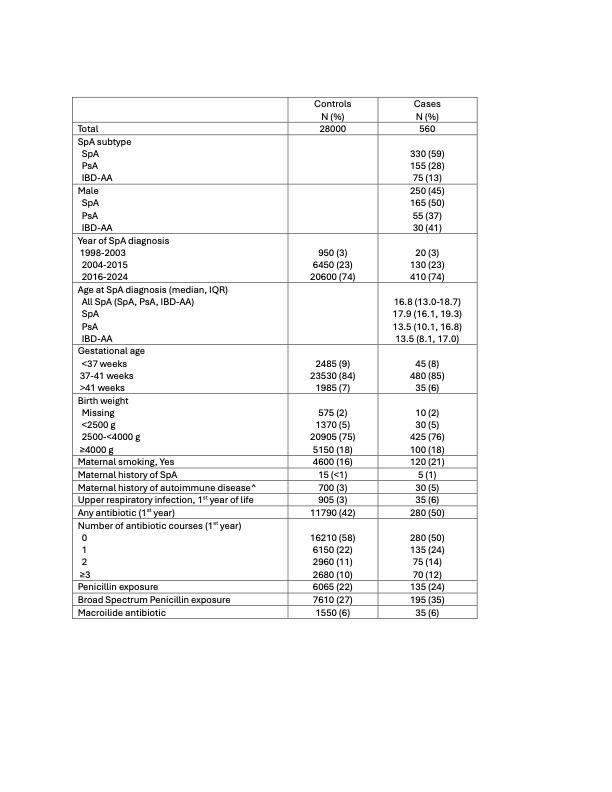 Legend. Numbers are rounded to the nearest 5, in accordance with data protection rules. ^
Legend. Numbers are rounded to the nearest 5, in accordance with data protection rules. ^
Included PsA, other JIA or rheumatoid arthritis, acute anterior uveitis, psoriasis, inflammatory
bowel disease, celiac disease, Type I diabetes, and autoimmune thyroid disease. Data for
tetracycline, metronidazole, clindamycin, vancomycin, carbapenems, cephalosporins,
sulfonamides, fluoroquinolones, aminoglycosides, antifungal, and antivirals are not shown due to
counts < 5.
Table 2. Antibiotic Exposure and Risk of SpA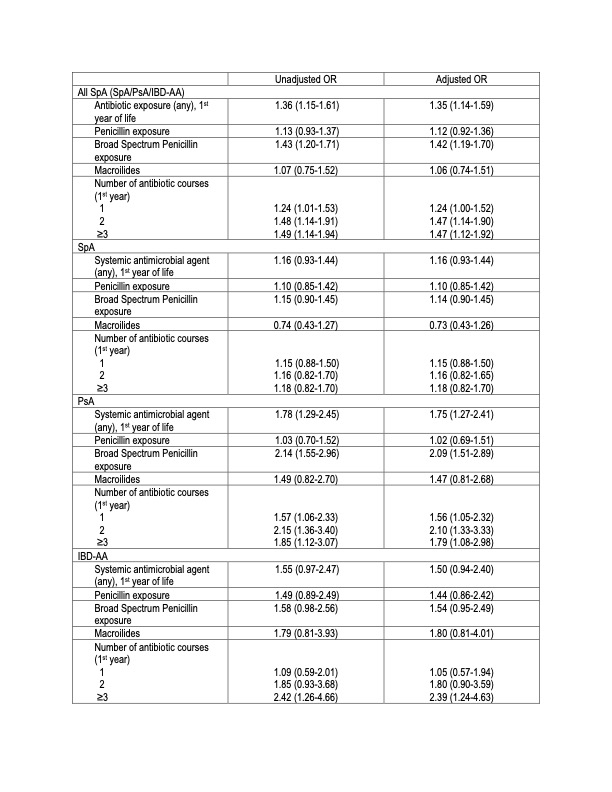 Legend. Adjusted model controlled for matching variables (sex, year of birth, calendar year of index date) by study design, plus maternal smoking, maternal age, maternal antibiotic use in the 3rd trimester, mode of delivery, and gestational age.
Legend. Adjusted model controlled for matching variables (sex, year of birth, calendar year of index date) by study design, plus maternal smoking, maternal age, maternal antibiotic use in the 3rd trimester, mode of delivery, and gestational age.
Table 3. Other Early Life Exposures and Risk of SpA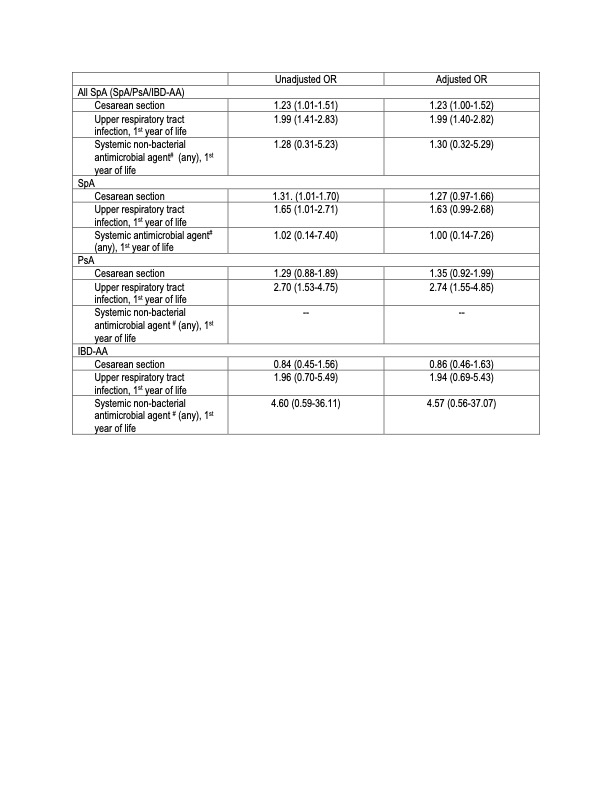 Legend. All adjusted logistic regression models included controlled for matching variables (sex, year of birth, calendar year of index date) by study design, plus use of antibiotics in the first year of life, maternal smoking, maternal age, maternal antibiotic use in the 3rd trimester, mode of delivery, and gestational age, and use of antibiotics in the first year of life. # Included any use of antifungals, antivirals, and antimycobacterials
Legend. All adjusted logistic regression models included controlled for matching variables (sex, year of birth, calendar year of index date) by study design, plus use of antibiotics in the first year of life, maternal smoking, maternal age, maternal antibiotic use in the 3rd trimester, mode of delivery, and gestational age, and use of antibiotics in the first year of life. # Included any use of antifungals, antivirals, and antimycobacterials
To cite this abstract in AMA style:
Altaffer A, Weisman M, Kaplan R, Horvath-Puho E, Toft Sorensen H, Weiss P. Early Life Exposures and Risk of Spondyloarthritis: A Population-Based Case-Control Study [abstract]. Arthritis Rheumatol. 2026; 78 (suppl 3). https://acrabstracts.org/abstract/early-life-exposures-and-risk-of-spondyloarthritis-a-population-based-case-control-study/. Accessed .« Back to 2026 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/early-life-exposures-and-risk-of-spondyloarthritis-a-population-based-case-control-study/
